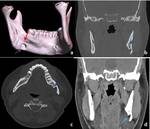
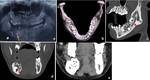
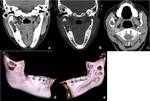
All suspected patients of Mandibular lesions underwent Computed tomography (CT) FACE on 256 Slice Dual Source SEIMENS CT Scanner.
All radiologically diagnosed focal or diffuse suspicious lesions underwent biopsy.
All biopsy-proven benign Mandibular lesions were included in this exhibit.
WHO histological classification of benign odontogenic tumors
Odontogenic epithelium with mature,
fibrous stroma without odontogenic ectomesenchyme
1. Ameloblastoma,
solid/multicystic type
2. Ameloblastoma,
extraosseous/peripheral type
3. Ameloblastoma,
desmoplastic type
4. Ameloblastoma,
unicystic type
5. Squamous odontogenic tumor
6. Calcifying epithelial odontogenic tumors
7. Adenomatoid odontogenic tumor
8. Keratocystic odontogenic tumor
Odontogenic epithelium with odontogenic ectomesenchyme,
with or without hard tissue formation
1. Ameloblastic fibroma
2. Ameloblastic fibrodentinoma
3. Ameloblastic fibro-odontoma
4. Odontoma,
complex type
5. Odontoma,
compound type
6. Odontoameloblastoma
7. Calcifying cystic odontogenic tumor
8. Dentinogenic ghost cell tumor
Mesenchyme and/or odontogenic ectomesenchyme with or without odontogenic epithelium
1. Odontogenic fibroma
2. Odontogenic myxoma/myxofibroma
3. Cementoblastoma
Bone-related lesions
1. Ossifying fibroma
2. Fibrous dysplasia
3. Osseous dysplasia’s
4. Central giant cell lesion (granuloma)
5. Cherubism
6. Aneurysmal bone cyst
7. Simple bone cyst
CYSTIC LESIONS OF JAW
Majority of cysts are odontogenic in origin and are epithelium-lined.
[2]
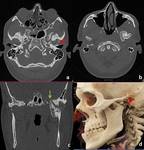
Radicular cyst (Periapical cyst): They are the most common odontogenic cyst resulting due to inflammation secondary to caries.
The cyst arises from epithelial remnants called rest of Malassez that are located in the periodontal ligament.
[1] The infection spreads to the root of the tooth resulting in periapical periodontitis,
granulomas,
abscess and finally a cyst formation.
Peak incidence is between 30 and 50 years of age.
[2] On radiography,
occur as well-circumscribed radiolucent lesions at the apex of the tooth,
usually measuring less than 1 cm,
may lead to root resorption in long-standing lesions.
(Figure 1) The term residual cyst should be used when the lesion persists even after tooth extraction.
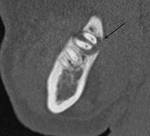
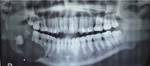
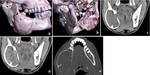
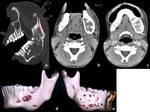
Dentigerous (Follicular) cyst: It is the second most common odontogenic cyst that develops around the crown of an unerupted tooth,
usually the third molar tooth.
The enamel epithelium lining the crown of tooth proliferates and secretes fluid.
Fluid collects between the layers of epithelium or between epithelium and enamel.
The wall of the cyst tends to converge to the cement-enamel junction.
Hence,
the presence of cystic cavity with the crown inside the cavity is virtually diagnostic.
[1,2] Displacement of the teeth is seen and resorption is not a feature of the follicular cyst.
Ameloblastoma,
mucoepidermoid tumor,
and carcinomas may develop in the wall of the cyst.
[1] (Figure 2,3)
Lateral periodontal cyst: It is a developmental cyst that arises from epithelial remnants in periodontal ligament along the lateral aspect of the tooth root.
Lateral radicular cyst: It is analogous to periapical cyst but occurs along the lateral aspect of the root.
Non-odontogenic cysts
Simple/Hemorrhagic/Traumatic bone cyst is a pseudocyst without an epithelial lining that usually is seen in young people in the second decade of life.
These are usually asymptomatic,
discovered incidentally and most commonly located in premolar region rather in incisor area of the mandible.
[1] On imaging,
they are slightly irregular in shape,
poorly defined borders; give scalloped appearance between the roots of the teeth.
On CT,
the high density may confirm blood products but density is variable.
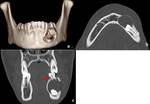
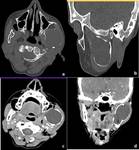
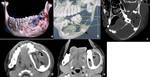
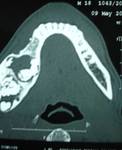
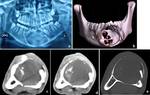
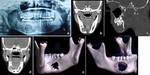
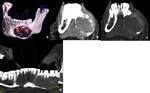
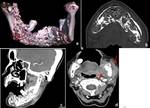
Aneurysmal bone cyst (ABC) is often expansile,
multilocular lesion shows cortical thinning or destruction and contains blood-filled spaces separated by fibrous septa.
The appearance is similar as in long bones.
On CT/MRI,
Presence of fluid-fluid levels may be present,
strongly suggestive of ABC.
In our case,
Fluid levels were not seen,
however expansile fluid density lesion causing marked bone remodeling and thinning was seen.
(Figure 4)
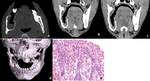
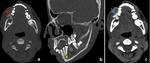
Stafne cyst (static bone cavity) is a radiolucency usually located on the medial surface of the posterior mandible near the angle of mandible below the mylohyoid line and mandibular canal.
These are more common in males with age range 20-70years.
The bone defect usually contains submandibular salivary gland or fatty tissue.
(Figure 5)
ODONTOGENIC TUMORS
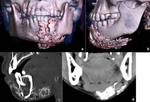
Ameloblastoma is a benign odontogenic tumor that arises from ameloblasts (enamel-forming cells),
has peak incidence in 3rd to 4th incidence of life with the majority of lesions occur in the mandible and in the posterior region.
Multiloculated/solid type give honeycombing like appearance,
may invade cortex to extend into adjacent tissues,
may lead to scalloping and bony expansion.
On MRI,
mixed solid and cystic components,
thick walls,
papillary projections with enhancing solid component and septae may be seen. Loss of lamina dura,
erosion of tooth apex and displacement of teeth may also be seen.
Presence of enhancing soft tissue component and papillary projections differentiates it from other cystic lesions.
[1] (Figure 6)
The Extra osseous/Peripheral type leads to superficial erosion of the bone due to pressure resorption with rare significant involvement of bone.
Desmoplastic type occurs mainly in anterior mandibular region,
has mixed lucent-opaque appearance with ill-defined borders,
hence difficult to distinguish from bone related lesions.
Unicystic type usually present at a younger age in second decade of life with the predilection for posterior mandible.
[3] Up to 80% are associated with an unerupted tooth usually the mandibular third molar.
Radiographically,
present as well corticated unilocular lesion with other features similar to other classical ameloblastoma.
(Figure 7,8).
Calcifying Epithelial Odontogenic Tumor (Pindborg tumor) is a locally invasive epithelial odontogenic neoplasm made of epithelial cells in fibrous stroma containing acidophilic homogenous structures that often calcify.
[1] They most commonly occur between 20 and 60 years of age (mean 40 years).
[4] Many of the lesions are seen in molar and premolar region and half of the cases are associated with crown of an impacted or unerupted tooth.
[4] Radiographically,
mixed lucent-opaque lesion,
may be uni or multilocular and has poorly defined margins.
Calcified components are seen close to crown of an impacted tooth.
(Figure 9)
Odontoma are the most common benign odontogenic tumors of epithelial and mesenchymal origin considered as hamartomas.
They are developmental lesions as dentin and enamel are laid down in an abnormal pattern.
They are made up of various components of teeth (enamel,
dentin,
cementum or pulp).
[5] They are of two types: Complex and compound.
Complex odontomas consist of radio-opaque masses usually associated with an unerupted tooth,
most commonly seen in molar and premolar region in mandible,
also seen in maxilla.
Occasionally,
surrounding lucent rim is seen.
Compound odontomas contain variable amount of tooth-like elements,
most commonly seen in incisor- canine region of maxilla.
(Figure 10)
Adenomatoid odontogenic tumor is an uncommon odontogenic neoplasm more common in young females in second decade of life and maxilla is more commonly involved than mandible often associated with unerupted permanent tooth mimicking dentigerous cyst.[6] The lesions have well demarcated radiolucent centres with punctuate calcifications.
If attached to tooth,
lesions are found more apically on root than dentigerous cyst.
[2] (Figure 11)
Ameloblastic fibroma is a rare odontogenic tumor that resembles the dental papillae and small islands of odontogenic epithelium that resembles the dental lamina.
More commonly seen in children with mandible more often affected than maxilla.
Radiographically,
lesions appear as well-defined to poorly-defined unilocular or multilocular radiolucency.
[7]
Keratocyst odontogenic tumor is a benign odontogenic tumor with a characteristic para keratinised stratified squamous epithelium.
The lesion is more commonly seen in posterior mandible and occurs in 2nd and 3rd decades of life.
The lesions can be multiple in Basal cell nevus syndrome.
The lesion can be unilocular or multilocular with smooth scalloped margins,
bulging of bony cortex,
occur commonly in body and ramus of mandible and may be associated with impacted tooth.
The lesion grows along the length of mandible and does not usually resorb teeth roots.
On MRI,
lesion has cystic appearance with thin wall,
heterogeneous intensity of fluid contents and weak contrast enhancement of the cyst wall.
[1] (Figure 12,13).
Odontogenic myxoma is an odontogenic tumor of mesenchymal in origin,
seen in 2nd and 3rd decade of life.
Mandible and maxilla are both equally involved and body and ramus are most commonly involved in the mandible.
The lesion contains stellate and spindle-shaped cells with an abundant myxoid or mucoid extracellular matrix.
The lesion appears multilocular or unilocular,
may give honeycombing like appearance mimicking ameloblastoma and other tumors and may cause extensive destruction of bone with marked cortical expansion.
[1,8]
Cementoblastoma is a rare odontogenic tumor characterized by cementum-like mass connected at the tooth root.
More commonly seen in males younger than 20 years of age with the predilection for mandibular first molar followed by premolar teeth.
Radiographically,
they appear as radiopaque mass confluent with the tooth root surrounded by a thin radiolucent periphery fused with roots of vital teeth.
[9]
BONE RELATED LESIONS
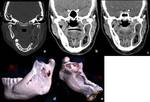
Ossifying fibroma: Fibro-osseous lesions constitute a spectrum of diseases in which normal bone tissue is replaced by fibroblasts and fibrous tissue with the presence of mineralized matrix.
Fibrous dysplasia,
bony dysplasia,
and ossifying fibroma constitute fibro-osseous lesions.
First two are reactive lesions while ossifying fibroma is a true neoplasm.
[10] They are more common in women in 3rd to 4th decade of life with premolar and molar area more commonly affected.
[11] Radiographically,
the lesion has a distinct boundary with normal bone in contrast to fibrous dysplasia.
The lesion is lucent in early stages,
becomes radiopaque as lesion grows surrounded by a halo of less ossified tissue.
[1] (Figure 14,15,16)
OTHER BENIGN NON ODONTOGENIC TUMORS
Osteochondroma (Exostosis) are the bony outgrowth of normal cancellous and compact.
(Figure 17)
Torus mandibularis is a type of exostosis on the lingual surface of mandible.
Osteoma contains is a benign neoplasm of cortical or cancellous bone with the most common site is in paranasal sinuses followed by the jaw.
Central giant cell granuloma is most commonly seen in females in 2nd and 3rd decade of life,
more common in anterior mandible between 2nd molar and 2nd premolar and have a tendency to cross midline.
Radiographically,
the lesion is often multilocular lucent with honeycombing appearance,
thin bony septae but may have unilocular appearance.
Lesions often are expansile,
can cause tooth displacement and resorption and may produce ground-glass opacities and occasional calcification.
[1]
Paget’s disease- Radiographically,
depending upon the stage of progression,
there can be punched out radiolucent lesions,
mixed areas and more sclerotic areas.
In the mandible,
both rarefaction and sclerosis is common.
In our case,
mixed lytic and ground glass opacity is seen with multiple areas of perforated cortex and air foci within to suggest secondary infection.
[1] (Figure 18)
Hemangioma is a benign neoplasm of proliferating endothelial cells.
They are more common in females and rarely involve jaw.
Radiographically,
appear as radiolucent lesions and may appear multilocular in shape.
Doppler may be useful and angiography shows prolonged parenchymal staining and tissue blush.
In our case,
hyperdense soft tissue component was seen within the lytic component of the lesion which may suggest locule of blood. (Figure 19)
Neurogenic tumors – Radiographically,
schwannoma arising from inferior alveolar nerve lesions may present as radiolucency which can lead to widening and expansion of inferior alveolar canal.
Neurofibroma adjacent to bone may produce pressure defect on the surface of the bone.
INFLAMMATORY CONDITIONS
Osteoradionecrosis may occur as a sequel to heavy irradiation which leads to painful necrosis followed by sequestration of bone.
Radiographically,
in late stages,
ill-defined radiolucent areas giving moth-eaten appearance with areas of sequestra and variable areas of cortical breach may develop.
Osteomyelitis may develop in jaw secondary to odontogenic infection.
The presentation and radiographic findings are similar as in other parts of the body.