In this educational exhibit we classify common fourth ventricle masses according to the patient´s age.
But for a better understanding of the behavior of these lesions,
we must first know the anatomy of the fourth ventricle and its anatomical relationships,
so we will explain and illustrate them.
Subsequently,
we will describe and in most cases illustrate with CT and MR,
the typical radiological findings of each mass,
using in some masses advanced MRI features to get a better characterization.
Finally we will expose a clear classification of these masses and provide key points to facilitate their differential diagnosis.
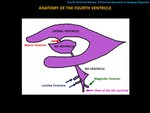
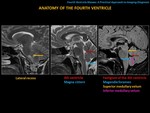
A) ANATOMY OF THE FOURTH VENTRICLE
The fourth ventricle is located in the posterior fossa and it has a “diamond shape”.
At the level of the apex (upper portion),
it communicates through the cerebral aqueduct (of Sylvius) with the third ventricle.
In its lower half,
the fourth ventricle communicates anterolaterally,
through the lateral recesses and Luschka foramina,
with the pontocerebellar cisterns.
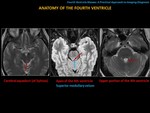
At the level of the obex (lower portion) it communicates inferiorly with the central canal of the spinal cord.
And,
in its lower half,
the fourth ventricle communicates dorsally and inferiorly,
through the foramen of Magendie,
with the Magna cistern.
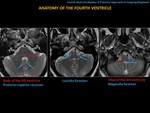
The choroidal plexus of the fourth ventricle are located in the lateral recesses and in the Luschka foramina (should not be mistaken for an enhancing mass at this level),
unlike the Magendie foramen,
which does not contain choroid plexus.
The posterior superior recesses are located at the level of the body (dorsally) of the fourth ventricle and they are thin,
fluid-filled,
blind sacs,
that line the cerebellar tonsils.
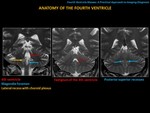
The limits of the fourth ventricle are formed by the protuberance (anteriorly),
the superior and inferior medullary velum and the cerebellum (dorsally). The roof of the fourth ventricle is its upper portion and the floor is its lower portion.
(Fig. 1 ,
Fig. 2 ,
Fig. 3 ,
Fig. 4 and Fig. 5).
B) FOURTH VENTRICLE MASSES
1.
MORE FREQUENT IN CHILDREN:
-MEDULLOBLASTOMA
GENERALITIES:
It is a malignant and invasive embryonic tumor.
It is a highly cellular and a high-grade tumor,
qualities that are reflected in imaging studies.
It is usually located in the posterior fossa,
most often in the vermis or cerebellar hemispheres,
invading the fourth ventricle (affecting the roof of the fourth ventricle in most cases).
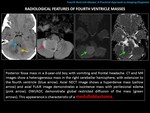
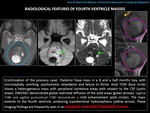
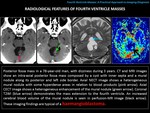
RADIOLOGICAL FINDINGS:
Posterior fossa mass,
homogeneous or heterogeneous,
which may contain cystic areas and,
less frequently,
calcifications or hemorrhage.
Perilesional edema is frequent.
NECT (Non-Enhanced-CT): hyperdense with respect to the cerebral parenchyma (hypercellular mass.
Hypodense areas may be present (cystic areas) or hyperdense areas (calcium or hemorrhage,
depending on the density in each case).
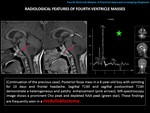
MR: T1: hypointense relative to GM (gray matter).
Hyperdense areas may be present (hemorrhage).
T2/FLAIR (Fluid Attenuation Inversion Recovery): heterogeneous mass,
with hyperintense (cystic areas) and hypointense areas (solid-hypercellular areas).
DWI/ADC (Diffusion-weighted imaging/apparent diffusion coefficient): marked high DWI and low ADC signal (“restricted diffusion”- hypercellular mass).
Perfusion-MR: increased cerebral blood volume.
MR-spectroscopy: prominent Cho (choline) and lipid peaks,
depleted NAA (N-acetyl-aspartate) and high taurine.
Enhancement: varied.
Medulloblastoma can enhance from a homogenous and diffuse way,
to a more heterogeneous and patchy form.
These tumors may present microscopic nodular seeding in the subarachnoid space,
so that at the time of diagnosis,
a MR study of the entire spinal column should be performed to detect the possible leptomeningeal tumor extension.
(Fig. 6 and Fig. 7).
-ATYPICAL TERATOID/RHABDOID TUMOR
GENERALITIES:
It is a high-grade embryological tumor,
whose cells are composed of a variety of histological components (neuroectodermal,
mesenchymal,
rhabdoid or epithelial),
without being considered a teratoma.
It is very similar to medulloblastoma,
although atypical teratoid/rhabdoid tumor usually occurs in patients less than 3 years old and can now be differentiated from medulloblastoma with immunohistochemical techniques.
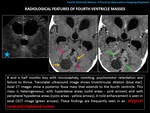
RADIOLOGICAL FINDINGS:
This tumor has very similar radiological characteristics to medulloblastoma.
Some of the findings that can support the diagnosis of this tumor versus medulloblastoma (apart from the patient's age) are the presence of peripheral cysts,
calcifications,
internal bleeding,
invasion of the cerebellopontine angle or the location outside the midline.
This tumor usually shows a heterogeneous enhancement,
due to its complex histopathology.
The aggressive behavior of this tumor,
such as the invasion of the base of the skull,
is a characteristic that may differentiate it from other cystic tumors of the posterior fossa such as pilocytic astrocytoma.
(Fig. 8 and Fig. 9).
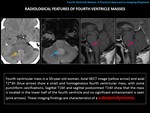
-EPENDYMOMA
GENERALITIES:
It is a slow-growing tumor,
which originates in the ependymal cells,
usually from the floor of the fourth ventricle.
It usually presents a plastic growth ("soft tumor"),
entering the foramina and cisterns.
It is a tumor of low relative cellularity,
comparing with medulloblastoma and it is usually located in the floor of the fourth ventricle.
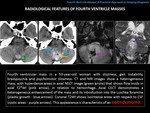
RADIOLOGICAL FINDINGS:
Mass with irregular morphology and plastic growth.
It is a heterogeneous tumor,
frequently presenting cysts,
calcifications and/or hemorrhage.
NECT: heterogeneous,
with hyperdense areas (hemorrhage or calcifications) and hypodense (cystic areas).
MR: T1: usually iso or hypointense,
with hyperintense areas (hemorrhage).
T2/FLAIR: usually iso/hyperintense,
with markedly hyperintense areas (cystic areas).
T2* (gradient-echo): flow voids (hemorrhage or calcifications).
DWI/ADC: no significant restricted diffusion (usually low cellularity tumor).
Perfusion-MR: increased cerebral blood volume (due to the fenestration of the blood vessels).
MR-spectroscopy: increased Cho peak and decreased NAA peak,
but the ratio of NAA/Cho is higher than in medulloblastoma.
Enhancement: variable and heterogeneous.
(Fig. 10 and Fig. 11).
-PILOCYTIC ASTROCYTOMA
GENERALITIES:
It is a low-grade and slow growth astrocytic tumor,
which is usually located in the cerebellar hemispheres,
causing a mass effect in the fourth ventricle,
although in some cases it can extend into its interior.
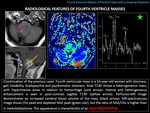
RADIOLOGICAL FINDINGS:
Posterior fossa mass,
well-defined,
composed most of the time by a cyst with a mural nodule; although in some occasions it can be visualized as a solid mass without cystic areas or with small cystic areas.
It shows less perilesional edema,
compared to high grade tumors,
and calcifications and hemorrhage are infrequent.
NECT: hypodense with respect to gray matter (cyst) with an isodense-hypodense mural nodule (solid nodule).
MR: T1: cystic area (iso-hyperintense with respect to cerebrospinal fluid-CSF) and mural nodule (iso-hypointense with respect to GM).
T2/FLAIR: cystic area (iso-hyperintense with respect to CSF) and mural nodule (hyperintense with respect to GM).
DWI/ADC: no restricted diffusion (low grade tumor).
MR-spectroscopy: mural nodule with elevation of the Cho/NAA ratio and increased lactate levels (paradoxical spectroscopic pattern,
which does not reflect the quiescent state of this tumor).
Enhancement: enhancement of the mural nodule.
(Fig. 12).
The main differential diagnosis in imaging studies of this tumor is the haemangioblastoma,
although the latter usually occurs in adults.
In addition,
relative blood brain volume is higher in haemangioblastoma in Perfusion-MR studies than in pilocytic astrocytoma,
one of the main qualities that makes it possible to differentiate them.
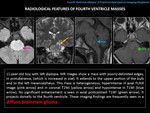
-BRAINSTEM GLIOMA
GENERALITIES:
Brainstem gliomas encompass a heterogeneous group of gliomas that affect the mesencephalon,
pons,
bulge and/or medulla.
They are broadly classified into diffuse intrinsic gliomas (more frequent) and non-diffuse brainstem tumors (exophytic lower brainstem gliomas and tectal gliomas.) Even they use to be intrinsic to the brainstem,
they can be exophytic and project dorsally to the 4th ventricle.
RADIOLOGICAL FINDINGS:
-Diffuse intrinsic glioma: when the glioma affects the protuberance,
the last is usually enlarged.
Generally it has poorly-delimited edges.
It is usually hypodense in NECT,
hypointense in T1MR and hyperintense heterogeneous in T2/FLAIR MR images.
The enhancement is frequently absent or mild and does not usually restrict diffusion.
-Non-diffuse brainstem tumors:
Exophytic glioma of the lower brain stem: well-defined tumor,
which usually originates in the posterior wall of the brainstem.
It tends to present a density and intensity similar to diffuse intrinsic glioma,
although it frequently presents moderate-intense homogenous or heterogeneous enhancement after contrast administration.
Tectal glioma: tumor that originates in the tectal plate.
It´s usually observed as a focal mass with density and intensity similar to the previous tumors,
although it frequently presents a slight enhancement after the administration of the contrast.
Perilesional edema is not usually present.
(Fig. 13).
2.
MORE FREQUENT IN ADULTS:
-METASTASIS
GENERALITIES:
Intraventricular metastases in adults are usually secondary to renal,
lung and colon neoplasms; in children they are usually due to neuroblastoma,
retinoblastoma or Wilms tumor.
They are usually located in the lateral ventricles,
although they can also be located in the third ventricle and less frequently in the fourth ventricle.
RADIOLOGICAL FINDINGS:
Although they are masses that may have a different radiological appearance,
they are usually masses that grow in the choroid plexus and tend to enhance intensively,
so they can be very similar to the choroid plexus neoplasms.
They may be accompanied by vasogenic edema of the adjacent cerebral or cerebellar parenchyma.
Metastases that are located in the union of the gray-white substance are more frequent.
- We must think of metastasis when we are in the context of a known primary tumor.
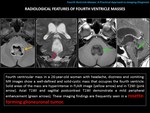
-SUBEPENDYMOMA
GENERALITIES:
It is a slow growing,
benign and rare tumor.
It is attached to the wall of the ventricle and is believed to originate from subependymal glial cells.
It is usually located in the fourth ventricle (especially in its lower half),
although some cases they have also been described in the lateral ventricles and third ventricle,
as well as in the spinal cord.
RADIOLOGICAL FINDINGS:
It is usually a small size and well-defined mass,
with solid or less frequently solid-cystic components and often presents calcifications.
Perilesional edema and hemorrhage are not usually present.
NECT: generally isodense relative to the adjacent parenchyma with hyperdense areas (calcifications).
MR: T1: isointense.
T2/FLAIR: hyperintense.
T2*: flow voids (calcifications).
Enhancement: none or mild.
(Fig. 14).
-HAEMANGIOBLASTOMA
GENERALITIES:
It is a highly vascular tumor.
It is usually an intraaxial,
posterior fossa mass,
most of the time located in the cerebellar hemispheres.
It can also be located in the cerebellar vermis,
in the fourth ventricle or in the spinal cord.
25-40% of these tumors are associated with Von Hippel Lindau syndrome.
RADIOLOGICAL FINDINGS:
Posterior fossa mass,
well defined,
composed frequently by a cyst with a mural nodule,
although in some cases it can be visualized as a solid mass.
NECT: hypodense component (cyst) and nodular isodense component (mural nodule).
MR: T1: hypo/isointense relative to GM.
T2/FLAIR: hyperintense relative to GM.
Perfusion-MR: higher relative blood brain volume of the mural nodule than pilocytic astrocytoma.
Enhancement: intense enhancement of the mural nodule.
The cyst wall does not usually enhance,
unless it is covered by tumor.
(Fig. 15).
-ROSETTE-FORMING GLIONEURONAL TUMOR
GENERALITIES:
It is a rare and slow growth tumor,
which derives from the pluripotent cells of the subependymal plate.
It is usually located in the midline of the posterior fossa,
frequently in the fourth ventricle (in most cases affecting its wall and floor).
RADIOLOGICAL FINDINGS:
Well-defined and solid-cystic mass,
sometimes with calcifications and hemorrhage.
Perilesional edema is not usually present.
NECT: heterogeneous,
with hypodense areas (cystic component) and isodense areas (solid component).
There may be hyperdense areas (hemorrhage or calcifications).
MR: T1: iso-hypointense.
T2/FLAIR: hyperintense.
DWI/ADC: no significant restricted diffusion.
Enhancement: none or mild heterogeneous (peripheral,
nodular ...
etc).
(Fig. 16).
3.
ALL AGES (age is not a key data to be taken into account):
-CHOROID PLEXUS NEOPLASMS
GENERALITIES:
They are tumors that derive from the epithelium of the choroidal plexus (very vascular tumors),
so they can be located in any region where the choroidal plexus are located,
however,
they are located more frequently in the atria of the lateral ventricles.
Tumors that are located in the fourth ventricle are evenly distributed across all age groups.
Histologically they are divided into choroid plexus papilloma (CPP) (WHO grade I),
atypical CPP (WHO grade II),
or choroid plexus carcinoma (CPC) (WHO grade III).
RADIOLOGICAL FINDINGS:
Although CPC is usually more heterogeneous than CPP,
radiological findings do not provide the distinction between these neoplasms.
CPP and atypical CPP usually present a lobulated morphology and CPC a more irregular morphology.
Calcifications,
cystic areas and perilesional edema may be present.
NECT: iso/hyperdense.
MR: T1: iso/hypointense.
T2/FLAIR: iso/hyperintense.
T2*: sometimes flow voids (calcifications).
Perfusion-MR: high relative blood brain volume of the tumor.
MR-spectroscopy: presence of Cho peak without the presence of creatine and NAA peaks.
CPC usually has a lactate peak.
Enhancement: intense and frequently homogeneous.
-All of them can produce dissemination by CSF (cerebrospinal fluid),
so it is recommendable to perform a study of the entire neuroaxis.
-In an adult with these radiological findings,
we must rule out metastasis of the choroid plexus,
since they are much more frequent than the primary neoplasms of the choroidal plexus.
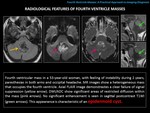
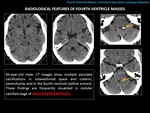
-EPIDERMOID CYST
GENERALITIES:
The epidermoid tumor is a congenital inclusion cyst.
It is usually located in the pontocerebellar cistern and the fourth ventricle is the second most frequent location in the posterior fossa.
RADIOLOGICAL FINDINGS:
Lobulated,
polypoid or irregular morphology mass,
with similar density and intensity to CSF,
except in FLAIR and DWI/ADC sequences.
Calcifications may be seen.
NECT: hypodense.
MR: T1 and T2: isointense with respect to the CSF.
FLAIR: usually does not completely null (hyperintense areas).
DWI/ADC: restricted diffusion.
Enhancement: frequently none and sometimes mild.
-FLAIR and DWI/ADC sequences allow differentiating these masses for example,
from arachnoid cysts,
since the latter are usually hypointense in FLAIR sequences and do not restrict diffusion.
(Fig. 17).
-DERMOID CYST
GENERALITIES:
It is an ectodermal inclusion cyst that may contain dermal elements with hair follicles and fat.
They are usually located in the sellar and parasellar region as well as in the frontonasal region,
although they can be visualized as a primary mass in the fourth ventricle.
RADIOLOGICAL FINDINGS:
Unilocular cystic and well-defined mass,
with fatty component.
NECT: hypodense and negative Hounsfield Units (HU) mass (fatty component).
MR: T1: hyperintense areas (fatty component).
T2: heterogeneous,
hypo/hyperintense.
Enhancement: generally null.
-These cysts can break and secondarily produce a seeding of fat droplets through the cisterns,
grooves and ventricles.
-NEUROCYSTICERCOSIS
GENERALITIES:
Intracranial parasitic infection,
caused by the larva Taenia Solium.
It presents different pathological stages: vesicular,
colloidal vesicular,
granular nodular and nodular calcified.
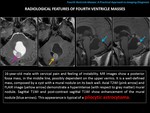
RADIOLOGICAL FINDINGS:
Cysts with "dot" inside are usually visualized,
frequently located in the subarachnoid spaces of the convexities.
They can also be located in the cisterns,
parenchyma and ventricular system (especially in the fourth ventricle).
The size of the cysts is variable,
usually from 5 to 20 mm.
- Vesicular: cyst with "dot" inside,
with density and intensity similar to CSF.
The wall enhancement is not usually present.
- Colloidal vesicular: cyst fluid is usually more hyperdense in NECT and more hyperintense in T1-MRI with respect to CSF.
The walls of the cyst tend to be thicker and enhance.
Perilesional edema is frequently present.
- Granular nodular: the cyst retracts and the edema and enhancement decrease.
- Nodular calcified: it is the final quiescent state.
There is usually no enhancement or edema.
The signal decreases in T2 and T2 *.
If long-term enhancement is visualized,
that can predict continuous seizures.
(Fig. 18).
(Fig. 19).