39 patients were included in the study,
with a mean age of 44.5 years (36-55).
24 months follow up was completed in 18 cases (46.2%),
21 patients were followed up during 12 month (53.8%) and all them during 6 months (100%).
Pre-embolization ultrasound was performed at 27 (69.2%),
pre-embolization MRI at 39 (100%),
c-US scan and c-MRI scan follow up were performed in all cases (100%).
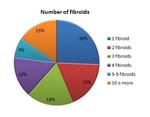
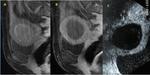
26% of patients had a single myoma (Figure 2). 77% of treated myomas were transmural,
while the remaining 23% were transmural with a submural component.
Of the total sample,
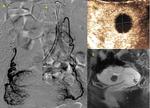
8 patients (17.9%) were re-admitted post UAE: 4 for severe pain,
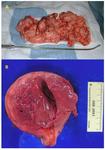
3 for expulsion of myoma (2 ended in hysterectomy) (Figure 3) and 1 for high fever.
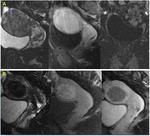
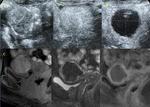
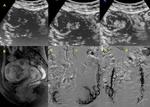
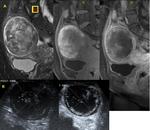
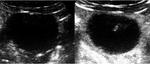
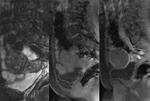
Post-treatment Sonovue ultrasonography as well as contrast-enhanced MRI demonstrated avascular tumor in 30 patients (82.1%) and persistence of tumor vascularization in 9 patients (17.9%).
(Figures 4,
5,
6,
7,
8,
9,
10,
11 and 12) those results showed a 100% PPV and 100% NPV of Sonovue ultrasound findings vs c-MRI findings (Figure 13).
Studying the 9 patients with persistent vascularization,
7 had transmural myomas and 2 transmural myomas with serous component.
The type of persistence vascularity was 2/9 peripheral uptake,
6/9 partial uptake less than 50% and 1/9 presented partial uptake vascularization but greater than 50% of the myoma.
Clinical review of these 9 patients showed persistent symptoms in 5 patients.
A second UAE was performed in all 5 cases,
and in 4 of them,
one or both ovarian arteries were now embolised.
Unfortunately,
one of these 5 patients required hysterectomy even though the second UAE was attempted.
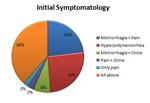
Figure 14 shows initial patients’ symptomatology.
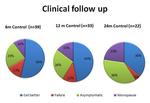
Figure 15 shows clinical symptoms evolution at 6,
12,
24 months Post UAE,
recording whether the patient presented 1) improvement 2) failure 3) asymptomatic 4) menopause.
Clinical evolution shows improvement of symptoms after 6-12 months post treatment with tendency to increase menopause and asymptomatic symptoms after 12-24 months,
as expected.
Analytical blood test follow up (HB,
FSH,
and LH) shows an increase in hemoglobin levels after UAE in patients with clinical and imaging successful treatment (Figure 16).
Interestingly,
patients with therapeutic failure had minimal increase in hemoglobin levels until a new embolization was performed.
Analytical data evolution evaluation of FSH and LH demonstrated a tendency to menopause hormone patron  in the group of patients with therapeutic success (Figure 17).
in the group of patients with therapeutic success (Figure 17).