1. Epidemiology:
· Our study regroups:
o 14 branch ducts or mixed intraductal papillary mucinous neoplasms cases (IPMN)
o 6 mucinous cystadenomas (MCADm) and 4 mucinous cystadenocarcinomas (MCADc)
o 8 serous cystadenomas(SCAD)
o 7 solid pseudo papillary tumors (SPPT)
o 2 Hydatic cysts of the pancreas
o 2 Neuroendocrine tumors
o 2 carcinosarcomas of the pancreas,
3 cystic adenocarcinomas of the pancreas,
1 cystic hemangioma and 1 multiple simple pancreatic cysts occurred on a patient presenting a Von Hippel Lindau syndrome
· Patients were aged between 22 and 87 years with a mean age of 54.2
· 18 patients were followed up and were non-surgical cases
· 32 among our patients were histopathologically proven.
· Pathology proved us wrong in 6 of these patients,
who presented atypical imaging features and/or very rare tumors.
2. IPMN:
· Our study included 14 patients:
o 9 BD (Branch ducts) IPMNs
o 3 Mixed IPMNs
o 2 Degenerated IPMNs
· Patients were aged 42 to 85 years,
with a mean age of 66,6.
| |
Fortunate |
Epigastric pain |
Acute pancreatitis |
| Motive of exploration |
8 |
5 |
1 |
Table 1: Motive of exploration
· All 14 patients had at least a cross sectional Imaging procedure:
o 13 had at least an MRI
o 12 had at least a CT scan
· Follow up duration was at least two years for non-surgical patients.
· Surgical resection was performed on two patients.
a) Morphology:
· CT imaging showed less complex type lesion,
than MRI ( 4 Vs 9).
· Less lesions were described as rounded or oval on MRI than CT (2 Vs 5).
| Shape |
Rounded/oval |
Lobulated |
Complex |
Clubbed fingers |
Total |
| CT |
5 |
2 |
4 |
1 |
12 |
| MRI |
2 |
2 |
9 |
0 |
13 |
Table 2: Lesions' morphology
Table 2: lesions’ morphology
b) multiplicity:
· MRI showed more lesions than CT .
· Lesions were multiple in 11/13 patients on MRI and 6/12 patients on CT.
| |
Unique |
Two to three |
multiple |
| CT |
3 |
3 |
6 |
| MRI |
1 |
1 |
11 |
Table 3: Lesions’ number
c) Communication with pancreatic ducts and MPD (Main pancreatic duct) caliber:
· CT imaging clearly detected the communication in 6/12 patients.
· MRI without MRCP detected the communication in 10/13 patients.
· MRCP clearly showed the communication in 11/12 patients.
· Half the patients showed dilated MPD (7/14).
· Dilatation was > 10 cm in only one patient,
who had a degenerated IPMN on pathology.
| |
No evidence of communication |
Uncertain |
MPD |
SPD |
MDP+SPD |
| CT |
3 |
3 |
5 |
1 |
0 |
| MRI: T2 |
2 |
0 |
8 |
2 |
1 |
| MRI: Post Gadolinium T1 |
2 |
0 |
5 |
1 |
1 |
| MRI: MRCP |
1
|
0 |
8 |
3 |
2 |
Table 4: Communication with pancreatic ducts
| Non dilated |
7 |
| Diffuse MPD dilatation |
3 |
| Localized dilatation |
4 |
| Dilated MPD |
7 |
| 5-6 mm |
3 |
| 6-10 mm |
3 |
|
> 10 mm
|
1 |
Table 5: MPD’s caliber
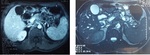
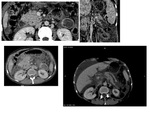
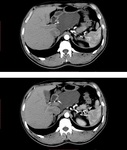
d) Wall thickness (Fig.
1):
· 13/14 patients showed thin walls with no mural nodules on their initial and follow up examination.
· Wall thickening was observed in one patient on both CT and MRI,
which presented as a mixed solid and multi cystic mass,
and was proven to be an invasive degenerated IPMN.
e) Lesions’ size:
· No significant differences were depicted in lesions’ size on MRI and CT
| |
Minimum |
Maximum |
Mean |
n |
| CT |
7 mm |
32 |
16.9 |
13 |
| MRI |
5 |
34 |
16.5 |
14 |
Table 6: Lesions' size on CT and MRI
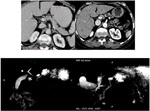
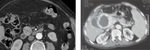
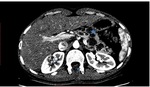
f) Outcome (Fig.
2):
· 10/14 patients showed no significant changes during follow up
· In our study,
two patients showed significant progression in size,
with no thickened walls or nodular enhancement
· Lesions were initially 8 and 21 mm in size,
· Close follow up was decided,
showing no further growth or morphological modification.
· Lesions were deemed benign,
and yearly MRI follow up was decided.
· 2/14 patients were surgically treated due to worrisome imaging features ( solid infiltrative component – Important main pancreatic duct dilatation )
3. Mucinous cystadenoma/carcinoma:
· Our study included 10 patients:
- 6 mucinous cystadenomas
- 4 mucinous cystadenocarcinomas
· Patients were aged 22 to 69 years,
with a mean age of 47.2.
· Motive of exploration was epigastric pain in 7 out of out 10 patients.
Three patients were incidentally diagnosed.
In addition,
a patient developed an acute pancreatitis during follow up.
· Only 3 patients had and an MRI,
with all of our 10 patients being explored by CT.
a) Morphology:
· All cystadenomas were oval or rounded
· All cystadenocarcinomas had lobulated margins
b) Lesions’ diameter:
| |
Minimum |
Maximum |
Mean |
| 10 Patients |
25 mm |
116 |
68 |
Table 7: Lesions' diameter
c) Wall thickening:
| < 5 mm |
> 5 mm |
Minimum |
Maximum |
| 6 patients |
4 patients |
2.5 mm |
21 mm |
Table 8: Wall thickening
d) Septation:
| |
None |
One |
Multiple |
| Septa |
4 |
1 |
5 |
Table 9: Septation
e) Localization:
| |
Body-Tail |
Tail |
Other |
| Localization |
4 |
6 |
0 |
Table 10: Localization
f) Outcome:
· All patients underwent surgical exploration
· All 6 patients,
deemed cytadenomas on CT and/or MRI,
were pathologically proven as so.
Only one patient developed a post-operative complication (pancreatic pseudo cyst)
· The cystadencarcinoma patients were un-resectable and died within two years post diagnosis.
4. Serous cystadenoma:
· Our study included 8 patients.
· Patients were aged 24 to 82 years,
with a mean age of 52,5.
· Motive of exploration was epigastric pain with one patient presenting also with worsening general status.
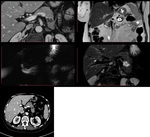
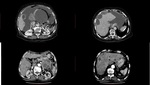
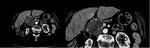
a) Morphology (Fig.
3):
· Our study included 8 patients.
· Patients were aged 24 to 82 years,
with a mean age of 52,5.
· Motive of exploration was epigastric pain with one patient presenting also with worsening general status.
| Diameter
|
Mean |
Minimum |
Maximum |
| 56 mm |
22 |
204 |
| Shape
|
Oval |
Lobulated |
| 1 Patient |
7 Patients |
| Septation |
None |
Multiple microcystic |
Multiple macrocystic |
| 2 |
4 |
1 |
|
Central scar
|
None |
Enhancing |
| 5 |
5 |
Table 11: Morphological characteristics of SCAD
b) Outcome:
· 3 lesions were resected,
due to:
o A unilocular appearance,
mimicking a MCAD
o Compression on the MPD and bile ducts
o Symptomatic lesion with a surgery demanding patient
· Follow up for the remaining 5 patients didn’t show any significant morphological changes.
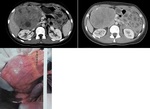
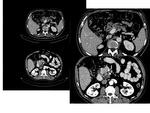
5. Solid pseudo papillary tumors (Fig 4):
· Our study included 7 cases.
· Patients,
all female,
were aged between 19 and 50 years at the time of diagnosis.
· The lesions’ size was between 31 and 130 mm with a mean of 66,1 mm.
· The masses were oval in shape in 6 cases and had lobulated margins in only one case.
All lesions presented a peripheral capsule with non-infiltrating,
sharp demarcated margins.
· All lesions presented a mass like enhancement on both CT and MRI.
· All patients underwent surgical resection with no post-operative complications.
· Calcifications:
| |
None |
Peripheral egg shell like |
Peripheral/irregular |
| Calcifications |
1 |
3 |
3 |
Table 12: Calcification in SPPT
6. Hydatic cyst of the pancreas:
· 2 cases were found in our study.
· Both patients presented mild nonspecific epigastric pain.
· Patients were aged 43 and 31 years on the time of diagnosis.
· Both patients were of rural origins.
· Lesions were both multilocular and presented thin non enhancing walls and septa.
Diagnosis was suggested on the bases of two main imaging features (Fig 5 and 6)
7. Neuroendocrine tumors (Fig 7):
· 2 cases were found in our study.
· Patients were aged 75 and 76 years on the time of diagnosis.
· Both were surgically treated with no post-operative complications.
· Diagnosis was suggested on CT,
no MRI imaging was performed.
· Both lesions were mixed solid and cystic,
presenting a peripheral vivid arterial enhancement.
8. Miscellaneous:
· Carcinosarcoma
· Cystic adenocarcinoma
· Pancreatic hemangioma
· multiple simple pancreatic cysts in VHL patients
a. Carcinosarcoma (Fig 8):
· Both patients presented with large pancreatic lesions with cystic liver and peritoneal metastasis.
b. Cystic adenocarcinoma (Fig 9):
– Infiltrating hypo attenuating masses presenting with cystic lesions with or without central,
ill defined,
central necrosis.
c. Cystic hemangioma (Fig 10):
• Thin walled cystic lesion,
with no septations,
presenting a thin rim of arterial peripheral enhancement,
in a 22 years old patient
• CT imaging suggested a cystic lymphangioma
• Pathology proved otherwise,
and pancreatic hemangioma was the final diagnosis.
d. Multiple simple pancreatic cysts in VHL patients (Fig 11):
9. Misdiagnosed cases (Fig 12 and 13):
· 6 out of our 50 patients (12 %) were misdiagnosed on pre-operative imaging
· These cases were:
o A serous cystadenoma mistaken for a solid pseudo papillary tumor.
o A serous cystadenoma mistaken for a cystic lymphangioma.
o A cystadenocarcinoma mistaken for a pancreatic adenocarcinoma.
o A pancreatic hemangioma mistaken for a serous cystadenoma.
o Two carcinosarcomas mistaken for infiltrating adenocarcinomas of the pancreas.
· Thus,
errors that we encountered in our study were due to:
o Rare tumours ( two carcinosarcomas and one hemangioma).
In that case imaging should define the infiltrating or benign character of these lesions and indicate biopsy or surgical resection.
o Atypical presentation of lesions,
especially unilocullar serous cystadenoma Vs mucinous cystadenoma and solid pseudo and papillary tumors,
mucinous cystadenoma Vs cystadenocarcinoma and IPMN vs Pseudo cyst.