Keywords:
Breast, Ultrasound, Screening, Diagnostic procedure, Localisation, Cancer, Image registration
Authors:
M. Horn1, D. Kim2, G. Ng3, B. N. Bloch1; 1Boston, MA/US, 2Toronto/CA, 3Bothell/US
DOI:
10.1594/ecr2018/C-2794
Methods and materials
The AI Breast solution on EPIQ Ultrasound (Philips Ultrasound Inc.),
was used with a standard ultrasound (US) probe (eL18-4 Linear PureWave Transducer,
Philips Ultrasound Inc.).
Supplemental components to support AI Breast include the Aurora Tabletop Field Generator and mattress (Northern Digital Inc.).
Patients are positioned the same as a routine breast ultrasound,
with their ipsilateral arm raised over their head.
A positioning aid is used to immobilize and flatten the breast parenchyma.
Efforts in immobilizing the breast tissue is essential for maintaining the system's calibration for optimal tracking [2].
The Tabletop Field Generator (TTFG) itself emits a very weak magnetic field.
Signals received from sensor coils while within the magnetic volume will translate to positional data onto the image display.
As such,
the patient's breast must be positioned on the mattress well within the magnetic tracking volume.
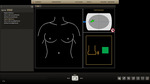
The top-right corner (Figures 1&2) shows a virtual display of the TTFG which is physically housed in a specially designed mattress.
This virtual display is used as a visual cue to ensure the patient`s breast is positioned for optimal tracking.
To begin the system calibration,
the eL18-4 probe with embedded electromagnetic sensor coils (6 degrees-of-freedom) is used in conjunction with the TTFG inside a gurney mattress.
The green indicator light confirms that the transducer is within the tracking volume.
After selecting Right/Left Breast,
the operator follows the dynamic prompt display.
This includes marking the nipple location in two orthogonal planes,
as well as the inferior,
medial and lateral boundaries of the breast to create a virtual map of the breast anatomy (Figure 2).
While performing the breast exam,
a series of short cine-loops were acquired through targeted areas to capture the full volume of each clinical finding.
As each image frame is acquired,
the transducer’s positional data is stored simultaneously for each image frame.
The stored position information is then used to automatically generate annotations for the identified lesions.
A prospective study approved by local IRB examined 25 patients using the AI Breast technique to evaluate its clinical effectiveness in standardizing imaging techniques across various operators,
and improving clinical practice efficiency through automation.