Tumors of the renal sinus
Various types of benign and malignant lesions can be found involving the renal sinus.
Observation of renal sinus fat is important in detecting a small tumor and determining the tumor stage.
Malignant tumors arising from the renal pelvis constitute only 5% of urinary tract neoplasms.
[5]
Transitional cell carcinomas (TCC) account for 95% of all uroepithelial tumours of the renal pelvis (the remaining 5% being made up of squamous cell carcinoma (SCC) (the majority) and adenocarcinoma (rare).
TCC have one of two main morphologic patterns: papillary (account for >85% tumours as multiple frond like papillary projections that tend to be low grade and invasion beyond the mucosa is a late feature) and non-papillary (sessile or nodular tumours that tend to be high grade with early invasion beyond the mucosa).
Clinical presentation is most frequently with microscopic or macroscopic haematuria.
If the tumor is located at the pelviureteric junction,
then symptomatic hydronephrosis may be the presenting symptom (flank pain) and clot-related renal colic may mimic renal calculi.
[6]
Some patients only present once metastatic disease becomes symptomatic,
with constitutional symptoms or focal symptoms due to a metastatic deposit.
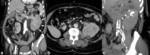
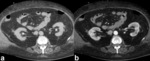
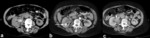
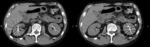
On CT examination transitional cell carcinomas are typically of soft tissue density (8-30 HU) (Fig. 1) with only mild enhancement (18-55HU),
usually significantly less enhancing than renal parenchyma or renal cell carcinomas (although the distinction cannot always be made).
They are usually centered on the renal pelvis (rather than the renal parenchyma as is the case with renal cell carcinoma) and range in size from small filling defects (difficult to see without distension or collecting system contrast) to large masses which obliterate the renal sinus fat (TCC is one of the causes of the so-called faceless kidney).
Unlike renal cell carcinomas that tend to distort the renal outline,
even large infiltrating TCC's maintain a normal renal shape.
[7] Larger tumours may have areas of necrosis.
In cases of the tumor being small and located at the pelviureteric junction (PUJ) with resultant hydronephrosis,
a small soft tissue mass should be sought.
In contrast to congenital PUJ obstruction,
the calyces are typically dilated,
and the renal pelvis wall may be thickened.
Occasionally numerous small calcification may be present,
located on the surface of papillary projections.
[8]
Squamous cell carcinoma comprises 1-7% of upper tract urothelial tumors.
Squamous cell carcinoma is frequently associated with longstanding infected staghorn calculi.
Affected patients frequently present with moderately to poorly differentiated tumors and advanced disease.
Imaging findings of squamous cell carcinomas are indistinguishable from those of transitional cell carcinomas.
Squamous cell carcinomas are strongly associated with renal calculi,
and chronic irritation of the urothelium appears to be an important etiologic factor in the development of squamous cell carcinoma.
The presence of a renal stone in association with a geographic infiltrating renal lesion with a large renal sinus component is suggestive of squamous cell carcinoma.
[9]
Adenocarcinoma accounts for less than 1% of upper tract tumors.
Patients with adenocarcinoma of the upper urinary tract may also have associated calculi and long-term obstruction,
suggesting an etiologic origin for these processes.
[10]
Mesenchymal tumors are defined as neoplasms with vascular,
fibrous,
adipose,
or other mesenchymal tissue differentiation.
On the basis of the histological features and clinicobiologic behavior,
adult renal mesenchymal tumors may be further classified into benign and malignant tumors.
Primary mesenchymal origin tumors of the kidney are rare but may develop in the renal sinus space as well as in the renal capsule and renal parenchyma.
The benign mesenchymal renal tumors include angiomyolipoma,
leiomyoma,
hemangioma,
lymphangioma,
juxtaglomerular cell tumor,
renomedullary interstitial cell tumor (medullary fibroma),
lipoma,
solitary fibrous tumor,
and schwannoma.
Malignant renal tumors of mesenchymal origin include leiomyosarcoma,
rhabdomyosarcoma,
angiosarcoma,
osteosarcoma,
synovial sarcoma,
fibrosarcoma,
malignant fibrous histiocytoma,
and solitary fibrous tumor.
Imaging findings of these rare tumors are usually nonspecific and MRI imaging has more advantages than CT in revealing the invasion of the renal vein and inferior vena cava,
however the CT features of primary renal sinus tumors are: commonly located within the renal sinus,
and the renal parenchyma and pelvis may be encroached by a malignant tumor; an obvious boundary between tumors and the renal collective system,
with frequently compressed pelvis and calyces; enhanced CT scanning demonstrates compressed vessels situated in the renal hilum and the excretion period of the enhancing CT scan reveals compressed renal pelvis and calyceal without filling defects.[11]
Tumors of the renal parenchyma that projects in to the renal sinus
Most renal parenchymal origin tumors grow by expansion,
manifesting as ball-like masses.
The medially growing renal parenchyma mass may project into the renal pelvis and compress or infiltrate the renal sinus fat.
The representative tumors are renal cell carcinoma (RCC) and benign multilocular cystic nephroma.
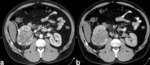
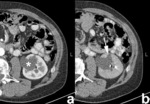
Renal cell carcinomas (Fig. 2) are primary malignant adenocarcinomas derived from the renal tubular epithelium and are the most common malignant renal tumor.
On imaging,
they have a variety of appearances,
from solid and relatively homogeneous to markedly heterogeneous with areas of necrosis,
cystic change,
and hemorrhage.
Most RCC grow by expansion and commonly extend into the renal pelvis,
leading to focal hydronephrosis or caliceal displacement.
[12]
Unlike TCC,
RCC has a tendency to extend into the venous system.
Three-dimensional CT or MR imaging helps delineate the precise location of the renal mass and its relationship to the collecting system and renal vessels.
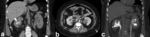
Multilocular cystic nephroma
Grossly,
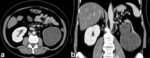
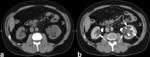
multilocular cystic nephroma (MCN) are typically unifocal multiloculated cystic masses surrounded by a thick fibrous capsule and compresses parenchyma (Fig. 3).
Calcification,
hemorrhage and necrosis are unusual.
CT imaging may present as large multilocular encapsulated cystic mass that often herniates into the renal pelvis,
with variable septal enhancement and no nodular or solid enhancement.
It may or may not associate streakiness in perirenal fat.
[13]
Radical or partial nephrectomy is usually done,
with lymph node excision.
Retroperitoneal tumors that extend to the renal sinus
As the renal sinus is a medial extension of the perinephric space,
any retroperitoneal tumor can extend to the renal sinus.
Many retroperitoneal tumors,
particularly lymphoma,
sarcomas,
multiple myelomas,
Castleman disease may involve the perinephric space and renal sinus by direct contiguous extension.
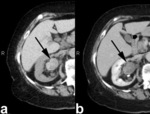
On CT imaging,
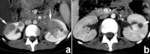
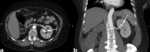
retroperitoneal lymphoma (Fig. 4) appears as an infusive tissue mass involving the perinephric region and the renal sinus. The renal vessels remain patent despite tumor encasement,
a finding that is characteristic for lymphoma; and obstructive hydronephrosis is often caused by direct involvement of the renal collecting system.
[14]
This situation is most common in patients with advanced non-Hodgkin lymphoma.
At CT and US,
lymphomatous masses are characteristically homogeneous.
At CT,
the mass enhances less.
Renal lymphoma is usually hypoechoic at US,
a finding that reflects tissue homogeneity.
Metastasis
Metastasis to the sinus lymph nodes occurs either as part of a generalized retroperitoneal process or as isolated involvement,
as with primary gonadal tumors,
because of the rich supply of perforating capsular vessels and lymphatic channels passing into the renal sinus.
[15]
Lipomatosis
The normal renal sinus contains fat that envelops the other structures within it.
Renal sinus lipomatosis (Fig. 5) refers to a condition where there is excessive renal sinus fat replacement.
The quantity of fat in the renal sinus normally and gradually increases with age and obesity.
Proliferation of sinus fat it results from renal parenchymal atrophy,
inflammation,
calculous disease,
ageing or exogenous or endogenous steroids.
Also,
there is an advanced form of massive renal sinus lipomatosis,
in which infection,
renal calculi and long-standing hydronephrosis are accompanied by severe renal parenchymal atrophy.
[14,
16]
Renal replacement lipomatosis is a rare condition characterized by fatty tissue proliferation in renal sinus and perinephric space with marked destruction/atrophy of renal parenchyma (due to chronic inflammation).
CT imaging is diagnostic and shows typical features including: renal parenchymal atrophy/destruction,
perinephric and hilar lipomatosis,
renal calculi,
perinephric abscesses which may extend to psoas muscle.
[17]
Renal sinus cysts are common simple renal cyst that lies within the renal sinus with a reported prevalence between 1.28% and 1.5% in autopsy cases.
[3]
They can be subdivided into: parapelvic cysts originate from the adjacent parenchyma and protrude into the renal sinus and peripelvic cysts originate within the sinus itself and have a lymphatic origin.
[18]
Parapelvic cysts (Fig. 6) are simple renal cysts that plunge into the renal sinus from the adjacent renal parenchyma.
They are usually single or few and resemble simple renal cortical cyst in morphology.
A parapelvic cyst at times may cause compression of the pelvicalyceal system resulting in hydronephrosis.
They may also mimic hidronephrosis,
termed pseudohydronephrosis.
Peripelvic cysts (Fig. 7) are frequently bilateral.
They appear as fluid-density cysts closely abutting the pelvis and infundibula,
rarely cause functional renal derangement by compression.
When followed up they remain unchanged in size.
They may be confused with hydronephrosis on noncontrast enhanced CT (NECT) and US,
but on contrast enhanced CT (CECT) the differentiation is obvious.
[6]
Vascular lesions
Vascular lesions,
such as renal artery aneurysm (Fig. 8),
pseudoaneurysm fistulating into the pyelocaliceal system (Fig. 9),
arteriovenous communication,
or renal vein varix,
can involve the renal sinus and manifest as a parapelvic mass or peripelvic lesion.
Their vascular nature is readily identifiable at color Doppler US,
contrast-enhanced CT or MR imaging,
and angiography.
There are three types of renal arteriovenous communications: congenital arteriovenous malformations; acquired arteriovenous fistula (associated with renal biopsy,
other renal operations,
trauma - usually penetrating,
postpartum (Fig. 10),
or malignant tumors) and idiopathic arteriovenous fistula.
[13]
Acquired lesions account for 70%–80% of all renal arteriovenous communications,
and biopsy-related lesions are the most common among them.
Most renal arteriovenous fistulas are clinically silent,
but they may manifest with at least one of the following signs: gross hematuria,
abdominal bruit,
high-output cardiac failure,
hypertension,
or abdominal pain.
An arteriovenous fistula may cause only subtle extrinsic impressions on the pelvicaliceal system by collateral vessels at excretory urography and can be easily missed even at crosssectional imaging,
depending on the lesion size.
[9]
Hematomas
Hemorrhage may be secondary to trauma,
related to a areteriovenous malformation or a complication of anticoagulant therapy (Fig. 11).
Renal sinus hematoma as a rare complication of anticoagulant therapy with effusion of blood into the renal sinus may be seen under certain circumstances (patients with prolonged protrombin time).
CT examination shows an amorphous high-density substance highly suggestive of fresh blood and no contrast enhancement.
[20]
Urinomas
Urinomas are urine collections usually found in the retroperitoneum,
most commonly in the perirenal space,
as a consequence of renal track leakage caused by urinary obstruction,
trauma,
or post-instrumentation.
Urine leakage is usually directly demonstrated on contrast-enhanced studies on the excretory phase due to direct contrast extravasation from the urinary tract.
[17]
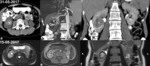
Urolithiasis
Urolithiasis is the most common cause of calcification in the kidney and a common cause of obstructive uropathy (Fig. 12).
The lifetime incidence of renal stones is high,
seen in as many as 5% of women and 12% of males.
By far the most common stone is calcium oxalate,
however,
the exact distribution of stones depends on the population and associated metabolic abnormalities.
Ninety-nine percent of renal tract calculi are visible on a non-contrast CT.
On CT almost all stones are "opaque" but vary considerably in density,
for example a calcium oxalate +/- calcium phosphate stone has a density around 400-600 HU,
and an uric acid stone between 100 and 200 HU.
Inflammatory lesions
Although it is rare to encounter a primary inflammatory lesion involving primarily the renal sinus,
extension of renal inflammatory lesions into the renal sinus and perinephric space is not uncommon in chronic or severe pyelonephritis.
Conglomerated inflammatory cells can cause a pseudotumor within the renal sinus.
[12]
Encrusted uretero-pyelitis (Fig. 13) is a rare and serious disease,
related to the presence of calcifications in the pelvicalyceal system and ureter,
associated with chronic urinary tract infection.
In most cases,
the causal agent of this infection is corynebacterium urealyticum.
The specific aspect of calcifications on CT scan can help to suggest diagnosis.
Miscellaneous
Heavy metal poisoning. The presence of metal objects in the scan field (Fig. 14) can lead to severe streaking artifacts.
They occur because the density of the metal is beyond the normal range that can be handled by the computer,
resulting in incomplete attenuation profiles.