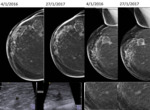
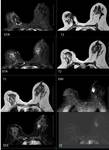
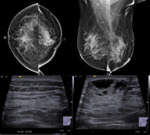
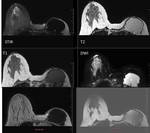
The various appearances in post-op breast in advanced techniques like Elastography,3D Tomo,
help in studying the morphology of the lesion.
MRI is of great value in conventional Birads IV lesions it is able give better clarity on elements of tissue composition especially in haematomas,fat necrosis & recurrance.
Functional imaging MRI (diffusion & ADC) and PET CT & is used for response assessment & recurrance in the adjuvant & neo-adjuvant settings and detect local & distant disease effectively.However there are pitfalls & fallacies and timing and the various appearances of the imaging needs to be understood in all these methods for effective management.
Role of Elastography & 3D Tomo:
Elastography has been incorporated in the 5th edition of Birads Lexicon.
Post-op seroma,
haematoma can present as mass like lesions & in B-Mode as complex & complicated cysts .
Softness & and a low strain ratio values in elastography helps to confirm the lesion as benign.
3D tomo helps in deciding the plane of the lesion and helps in confirming skin thickening (as they are seen in the superficial plane) ,scars (predominently 2-dimensional )also helps in assessing the contents & margins of lesions(Fig 5 ,6 &7).
But there are pitfalls and biopsy or MRI maybe needed to resolve certain lesions.( Fig 8)
Role of MRI:
MRI is done in post-op breasts in women with a history of breast cancer having suspicion for recurrence when clinical,
mammographic,
or ultrasound findings are inconclusive.
Dynamic Contrast enhanced sequences is a valuable tool.
MRI FINDING
Acute Change
- Haematomas & Seromas have variable signal intensity in T1 (low in acute to high in chronic) a smoother & thinner capsule.
- Recurrance is nodular & irregular.Enhancement can be early intense or both.
- Granulation tissue has moderate delayed enhancement is delayed;
Chronic and later changes
- 9-18 months,
enhancement may or may not be present at a lumpectomy site.Absence of enhancement excludes residual or recurrent disease.
- Scar tissue should not be enhancing after 18 months.
Therefore,
tissue that enhances must be considered suspicious,
and biopsy should be considered.
Fat necrosis is a sterile inflammation of the fat due to an inadequate blood in the autologous flap & at the site of BCS.
It is due to lipolysis,
inflammatory cell infiltration,
& haemorrhage which evolves in to fibrous scar & calcified cystic mass.
Fat necrosis though benign,
can mimic malignancy.
It typically occurs at the treated site and results in a wide spectrum of findings at MR imaging.
They may appear as rim enhancing,
homogeneous or heterogeneous enhancing mass,
associated with oil cyst,
a focal area or diffuse enhancement,
architectural distortion,
or irregular masses.
Fibrosis with varying appearances on T1-weighted images and associated architectural distortion can be seen with fat necrosis.
Fat necrosis is nearly isointense to fat elsewhere in the breast has varying pattern of enhancement kinetics.
Overlap exists between benign and malignant disease.
Suspicious findings may warrant tissue sampling.
A false-positive diagnosis may be made if enhancement is seen.
MR imaging is the appropriate modality for short-interval imaging surveillance of the post-BCT breast to identify lesions that need intervention and diagnose recurrence.
Birads lexicon is used to categorise the various findings.
BI-RADS 1 Category (Negative): BIRADS-I in BCT patients indicate a normal breast,
but this is not appropriate in a setting of BCS as there is a typical lumpectomy site.
BI-RADS 2 Category (Benign): Common findings such as skin thickening,
architectural distortion,
signal voids,
resolving edema,
seroma with or without thin rim enhancement (≤5 mm) or signal flare from surgical clips progressively decrease over time.
These findings can be considered for the BI-RADS 2 category.
(Fig 9 &10).
BI-RADS 3 Category (Probably Benign; Short-Interval Follow-up Suggested): Post BCT breast show a small focal area or thin linear persistent non mass like enhancement at or adjacent to the surgical site.
6-month follow-up is recommended.
(Fig 11).
BI-RADS 4 Category (Suspicious Abnormality; Biopsy Should Be Considered): Enhancing lesions(masses),
segmental or ductal and clumped NMLE,
nodularity larger than 5 mm around a seroma with a type III curve (rapid initial enhancement and washout),
and BIRADS III lesions with increased size or prominence during short-interval follow-up need to be biopsied.
(Fig 12 & 13).
BI-RADS 5 Category (Highly Suggestive of Malignancy; Appropriate Action Should Be Taken): They appear as irregular mass or masses with spiculated margins and type III kinetic curve.
(Fig14 & 15)
Autologous flap:
MRI depicts status and the type of the flap & helps to confirm the post -op fat necrosis.Commonly used are LD flap (Fig16 & 17) & TRAM flap (Fig 18 &19)
Autologous Fat Grafting :
Autologous Fat Grafting or autologous lipoaspirate grafting is done in an augmentation technique used in conjunction with flaps and in filling up lumpectomy or excisional biopsy defects.
It involves reinjection of aspirated fat from the abdomen or upper thigh.
On imaging,
there is hyperintensity on T1 weighted images and hypointensity on T2 weighted images and fat-saturated images.
Rim enhancement due to peripheral fibrosis and inflammation can be seen.
Calcifications can also be seen at the surgical site.
So the protocol is pre op mammogram and ultrasound,
followed by a new baseline mammogram and ultrasound after 6–12 months of autologous fat grafting.(Fig20)
Silicone implants:
The median life of an implant is 10.8 years.And rupture is silent MR imaging is recommended 3 years after implantation and every 2 years thereafter.
Extracapsular implant rupture,
or leaked silicone gel,
may cause local symptoms such as pain,
capsular contracture,
and breast asymmetry.
At imaging,
silicone signal material extruding from the capsule or silicone granuloma formation can be seen.Intracapsular implant rupture demonstrates the linguini,
keyhole,
and salad-oil signs.
(Fig 21,22 ).
MRI is very sensitive assessing implant integrity (MRI 93%,
US 77%,
Mammogram 68%) & is used for screening patients with silicone implants every 2 years.Water & Silicone supressed sequences are used for imaging.(Fig 23)
There have been anecdotal association between ruptured silicone implant and malignancy & connective tissue disease disorders.
(Fig24)
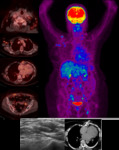
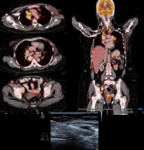
Whole body PETCT
PET CT is a whole-body functional evaluation and is excellent in the picking up distant metastases and in the staging of recurrent breast cancer.It is also useful in response evaluation in the adjuvant & neo-adjuvant setting.
FDG PET scanning is ccurate on or off hormonal therapy,
and may alter management in up to 51% of patients.
Ithelps in identifying the appropriate site for biopsy (Fig 25 ).But there are pit-falls due to artefacts.(Fig 25 & 27).It cannot diffrentiate between tuberculosis & malignancy.(Fig 28).