The role of imaging in the diagnostic process can be differentiated in these steps:
- Localization
- Characterization
- Staging (if necessary)
LOCALIZATION: the correct definition of the anatomical site of origin represents the first step in the abdominal mass evaluation.
Abdominal compartmentalization in intra-peritoneal,
retro-peritoneal and pelvic space can help in localizing a mass:
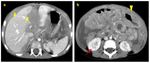
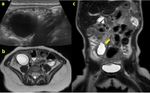
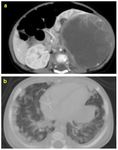
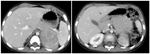
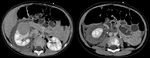
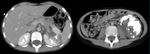
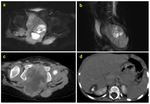
- In case of intra-peritoneal mass distinguishing hepatic mass from other gastrointestinal origin (Fig.
1-6).
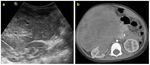
- In retroperitoneal mass differentiating their renal or extra-renal origin (Fig.
7-13).
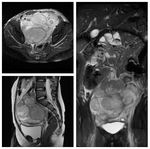
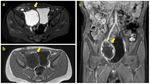
- In case of pelvic mass indicating whether the mass is located in the anterior pelvis,
intermediate compartment,
posterior pelvis (presacral) or lateral compartment (Fig.14-22).
However,
due to its large size,
a mass may present as intra-abdominal even though it may have originated in the retroperitoneum.
CHARACTERIZATION: differential diagnosis depends on the macroscopic tissue characterization of a mass.
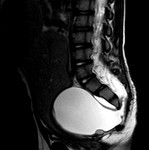
Cystic
- Malformative origin: mesenteric cyst/lymphatic malformation,
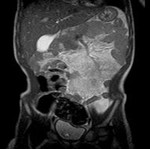
duplication cyst (Fig.
6),
anterior meningocele (Fig.
21)
- Infective/inflammatory origin: hydatid infection,
hepatic abscess
- Neoplastic: cystic Wilms tumor,
cystic neuroblastoma
- Functional: functional ovarian cyst (most regress within 2 cycles),
ureterovesical junction obstruction.
Solid
- Benign mass: ectopic kidney
- Neoplastic: Wilms tumor (Fig.
7,
12,
13),
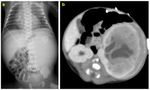
neuroblastoma (Fig.
8),
B-non-Hodgkin lymphoma (Fig.
1,
2)
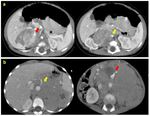
Mixed
- Benign mass: adrenal hemorrhage
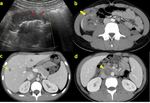
- Malignant mass complicated by a colliquation phenomenon (Fig.
10a)
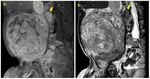
- Teratoma (Fig.
15,
22)
STAGING
- Morphological characteristics
- No.
lesions
- Location
- Extension
- Margins
- Vascular involvement
- Lymph node involvement
- Distant metastasis
IMAGING
First-level examination
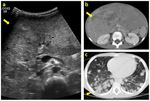
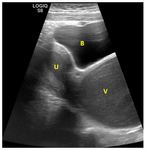
- Ultrasound: in pediatric patients US examination is the first-level imaging modality,
giving the preliminary information of location and size (Fig.
3a,
5a,
6a,
7a,
14).
It provides also an initial mass characterization and evaluates the presence of vascularization (with Doppler-US) (Fig.
5a).
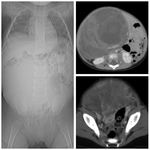
- Abdominal X-ray: it’s not the initial imaging modality of choice, although it may detect the mass effect (dislocation of intestinal loops and opacification) and calcium deposits (teratoma or neuroblastoma) (Fig.
9a).
Other imaging modalities are often required,
due to the US limits in investigating the retroperitoneum,
the presence of intestinal meteorism and inadequate measurement of the lesion.
For complete information,
barium enema,
cystouretherogram,
CT scan or MR can be required.
Second-level examination
CT and MR are the proper imaging modalities in the diagnostic process of an abdominal mass and are mandatory for the staging of neoplastic lesions.
- CT has the highest spatial resolution and permits to investigate pulmonary parenchyma.
Multidetector scanners allow rapid imaging of the chest,
abdomen,
and pelvis in one setting in order to detect distant metastasis (indispensable in staging phase) (Fig.
3c,
10b).
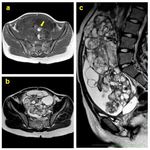
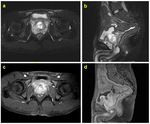
- MR is radiation-free and has the highest contrast resolution with possibility of tissue characterization.
This is the reason why MR is recommended in pelvic mass and it’s the proper imaging modality for loco-regional staging (studying the involvement of vascular and nerve structures) (Fig.
6b-c,
15,
17-22).
Note that for some tumors,
such as rhabdomyosarcoma,
the initial staging evaluation must also include other examination in order to assess possible sites of distant metastases: nuclear medicine modalities (nuclear bone scintigraphy),
hybrid imaging (PET-CT),
bone marrow aspiration and/or biopsy.
DIFFERENTIAL DIAGNOSIS
Two different processes may look morphologically similar,
yet have completely different pathogenesis and significance.
The main example is the differential diagnosis between the most common abdominal neoplastic lesion of the childhood: Neuroblastoma vs Wilms tumor,
both retroperitoneal tumors (Fig.
7,
8,
12,
13).
| |
Neuroblastoma
|
Wilms tumor
|
|
Median age
|
2 y
|
3 y
|
|
Clinical findings
|
pallor,
skin nodules (blueberry muffin syndrome),
hepatomegaly (liver mets- Pepper syndrome ),
periorbital ecchymosis (extensive metastasis at skull base),
paraplegia,
ataxia.
|
unless traumatized,
commonly presents as a large abdominal mass without pain; the patient is apparently in good health.
|
|
Growth
|
Invasive growth,
typical aorta encasement and midline extension (75% of cases)
|
Typically spreads by direct extension and displaces adjacent structures
|
|
Calcifications
|
Frequent
|
Rare
|
|
Pulmonary Mts
|
Rare
|
20% of cases
|
|
Kidney
|
Kidney displaced by the mass
|
the mass origins from kidney
|
|
Invasion of renal vein and inferior vena cava
|
Almost absent
|
More frequent
|
Moreover neuroblastoma matrix varies with age: in infants and children it’s predominantly a solid mass,
instead in neonates it can be a cystic or a complex mass,
simulating an adrenal hemorrage.
Pelvic masses represent another diagnostic challenge.
Rhabdomyosarcoma is the third commonest extracranial solid malignancy (Fig.
16-19).
|
Anterior compartment: bladder,
prostate
|
Lateral
compartment
|
|
Rhabdomyosarcoma
Rare: leiomyosarcoma,
transitional cells carcinoma,
rhabdoid tumor
|
|
Intermediate compartment: the space between bladder and rectum
|
Bone: osteosarcoma, Ewing's sarcoma Lymph Nodes: lymphomas, leukemias,
metastases Soft tissues: RMS,
extrarenal Wilms t.
Vessels
Nervous tissue
|
|
Uterus/vagina:hematocolpo,
rhabdomyosarcoma.
Ovarian origin: functional cysts,
germ cell t., stromal t.,
ephithelial tumors.
Metastasis
|
|
Posterior compartment: presacral space
|
|
Meningocele,
sacrococcygeal teratoma,
germ cell t.,
neuroblastoma,
ganglioneuroblastoma, schwannoma
|
Cystic abdominal masses VS Pelvic masses in females:
- Ovarian tumors: Cystic Teratoma vs Cystadenoma
- Lymphangioma (mesenteric)
- Enteric duplication cyst (Fig.
6)
The most common ovarian neoplasm is mature cystic teratoma (90% benign).
Benign teratomas comprise 67% of pediatric ovarian neoplasms and are bilateral in up to 25% of cases.
The second category of neoplasms is epithelial tumors (cystadenomas and cystadenocarcinomas),
extremely rare in the 1st two decades [10].
In presacral malignancies:
- spinal canal invasion: neuroblastoma
- normal spine: malignant teratoma (predominantly solid) (Fig.
22).