In most cases,
the aneurysm ruptures along its posterolateral border into the retroperitoneum,
causing a retroperitoneal hematoma adjacent to the aneurysm [2,
5,
5] (Fig. 1 and Fig. 2).

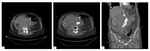
Fig. 1: Axial non-enhanced (A) and contrast-enhanced (B) CT images showing a ruptured abdominal aortic aneurysm. A large retroperitoneal haematoma can be seen in the perirenal and pararenal spaces, especially on the right. In the anterior aortic wall, a disruption of intimal calcifications with tangential calcium sign can be seen (arrow in A and B) indicating the rupture site. Coronal MPR (C) also shows the aneurysm and retroperitoneal haemorrhage.

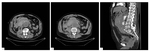
Fig. 2: Axial (A and B) and sagittal MPR (C) non-enhanced CT images showing large retroperitoneal haematoma adjacent to an abdominal aortic aneurysm. The haematoma contains hyperattenuating areas, indicating recent haemorraghe, and extends along the anterior and posterior pararenal spaces on the right. Bulging of the aortic wall and discontinuity of the intimal calcifications are also seen on B.
When the rupture is subtler,
only stranding of the fat adjacent to AAA may be seen.
When large,
the hematoma fills the perirenal and pararenal spaces and displaces the kidneys anteriorly or laterally.
Haemorrhage directly to the peritoneal cavity can also occur as can,
although very rarely,
haemorrhage into the gastrointestinal tract (Fig. 3) or the inferior vena cava [5].
After intravenous administration,
contrast can be seen leaking from the aneurysm [2].
The imaging features of rupture are usually straightforward and should prompt immediate surgical or endovascular treatment.

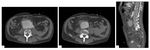
Fig. 3: Axial (A and B) and sagittal MPR (C) contrast-enhanced CT images shows a large aneurysmal dilatation of the distal aorta. Air bubbles can be seen adjacent on the retroperitoneal space, adjacent to the aneurysmal sac, indicating rupture into the gastrointestinal tract. There is also periaortic fat stranding and a large haematoma on the left iliac fossa.
The draped aorta sign (Fig. 4,
Fig. 5 and Fig. 6) is seen in contained aneurysmal ruptures.
In this scenario,
the aneurysmal wall bulges posterior and follows the contour of the psoas muscle or the vertebral bodies.
This sign represents a focal weakness in the posterior wall and,
with time,
can progress to frank rupture [6].

Fig. 4: Axial (A and B) and sagittal MPR (C) non-enhanced CT images shows the draped aorta sign, indicating a contained ruptured aneurysm. The left posterolateral wall of the aneurysm bulges posteriorly and loses its interface with the psoas muscle.

Fig. 5: Axial non-enhanced lumbar spine CT image, performed to evaluate low back pain in a 78 year old patient, shows erosion associated with sclerosis of L3. A bulging of the posterior wall of an aortic aneurysm was also noted.

Fig. 6: Axial (A and B) and sagittal MPR (C) contrast-enhanced CT images of the same patient of fig. 5 shows a contained ruptured aneurysm bulging posteriorly and eroding the lumbar vertebral bodies (draped aorta sign). The vertebral bodies shows some sclerosis, suggesting a chronic process, nevertheless this finding should alert for the impending risk of a frank rupture.
The CT signs of impending rupture could be very subtle and easily missed.
Their identification can have significant implications in the outcome of the patient,
allowing for treatment to be planned in a timely manner.
These include rapid enlargement of the aneurysmal sac,
discontinuity of intimal calcifications and the hyperattenuating crescent sign.
As stated above,
the AAA diameter is associated with the risk of rupture,
with higher risk above 5.5cm [3] (Fig. 7).
Rapid enlargement indicates an unstable aneurysm and is also associated with rupture.
The measurements should ideally be made in a plane perpendicular to the long axis of the aneurysm and increases in diameter of more than 5-7mm in 6 months or ≥ 1cm in one year are an indication for treatment [7].
Of course,
the enlargement can only be assessed if prior examinations are available,
which may not be possible in a symptomatic patient presenting in the emergency.

Fig. 7: Abdominal radiography (A) of a patient presenting with a pulsatile mass on the abdomen shows a large aortic aneurysm. Subsequent contrast-enhanced CT scan (B and C) better depicts the aneurysm. Although there are no signs of rupture, the large diameter of the aneurysm poses a risk of rupture.
The finding of focal discontinuity of the intimal calcifications is unreliable,
especially if there are no previous examinations available for comparison [5].
When rupture is present,
usually the site of haemorrhage can be identified by noting the calcification disruption and displacement (Fig. 1 and Fig. 2).
The hyperattenuating crescent sign is highly specific for complicated aneurysms [8].
It represents recent haemorrhage in the wall thrombus,
which could further damage the aortic wall and lead to rupture.
In CT scans it manifests as an area of high attenuation interposed between the thrombus and the aortic wall.
It should be higher attenuation than the intravascular blood or the psoas muscles in unenhanced and enhanced-CT,
respectively [5] (Fig. 8).
A possible pitfall is the inflammatory aneurysm (Fig. 9).
In this case enhancing fibrotic tissue is seen surrounding the aortic wall [2].

Fig. 8: Axial non-enhanced CT image shows a large aneurysm with a crescentic area of high attenuation seen between the thrombus and the posterior aortic wall (hyperattenuating crescent sign). This area shows a higher attenuation than the blood on the aortic lumen and on enhanced-CT the attenuation should be higher than of the psoas muscle.

Fig. 9: Axial contrast-enhanced CT image shows an aortic aneurysm surrounded by a area of high attenuation. This is seen anteriorly to the aortic wall and the attenuation is similar to that of the psoas muscle. This was caused by fibrotic tissue in an inflammatory aneurysm and, although this aneurysm are more prone to rupture, it does not indicate impending rupture. This patient also presented with right hydronephrosis (not shown), a common complication of this pathology.