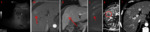
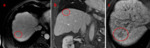
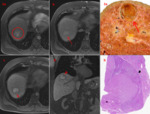
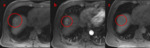
Using LI-RADS 2017
LI-RADS should be used in patients at high risk of HCC,
this includes patients with cirrhosis,
those with chronic hepatitis B infection and finally those with current or previous HCC,
whether or not there is underlying cirrhosis/chronic hepatitis B infection.
LI-RADS should not be used in patients below the age of 18,
those with cirrhosis secondary to an underlying vascular disorder or those with congenital hepatic fibrosis.
In addition,
it should not be used to assess lesions which have a pathological diagnosis of malignancy or a path-proven benign lesion of non-hepatocellular origin such as a haemangioma.
LI-RADS Categories
Using LI-RADS any observation within the liver can be categorised into one of eight different categories,
these are summarised in Table 1 below:
| Category |
Definition |
|
LR-NC
(New to 2017
|
Not categorisable,
either due to image omission or degradation |
| LR-1 |
Definitely benign |
|
LR-2
|
Probably benign |
| LR-3 |
Intermediate probability of malignancy |
| LR-4 |
Probably HCC |
| LR-5 |
Definitely HCC |
|
LR-M
|
Probably or definitely malignant,
not necessarily HCC |
|
LR-TIV
(Previously
LR-5V)
|
Tumour in vein |
Table 1.
LI-RADS Categories.
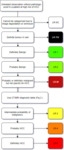
LI-RADS Diagnostic Algorithm
When a finding is made within the liver of a patient at risk of HCC a simple algorithm should be used to make the assessment.
This is outlined in Fig. 1.
Once a LI-RADS category has been chosen this may then be adjusted using ancillary features to up or downgrade by one category (ancillary features described below - Table 3).
If there are one or more ancillary features favouring malignancy,
the category can be upgraded by one,
up to a maximum of LR-4.
Conversely if there are one or more features favouring benignity then the category can be downgraded by one.
If the ancillary features are conflicting then the category should not be adjusted.
The use of these ancillary features is optional,
at the discretion of the reporting radiologist (this is new in the 2017 edition).
If at this point there is any uncertainty then tie breaking rules may be applied.
If the uncertainty is between LR-1 to 5 then the category reflecting lower certainty should be chosen.
If a finding has malignant characteristics but there is uncertainty of hepatocellular origin then LR-M should be chosen and if there is doubt about the presence of tumour in the vein then one should not categorise the finding as LR-TIV.
Finally,
the reporting radiologist should make a common sense judgement to ensure the final category seems appropriate,
if not the finding should be reassessed.
LR-1 and LR-2
The LR-1 and 2 categories should be applied to lesions that have characteristic benign appearances,
this includes but is not limited to:
- Cyst
- Haemangioma
- Transient hepatic attenuation difference (THAD)
- Focal fatty infiltration/sparing
- Confluent fibrosis or focal scarring
Additionally,
lesions that disappear spontaneously should be categorised LR-1. A distinctive solid nodule (ie one with no major features of HCC,
no feature of LR-M and no ancillary features of malignancy) should be categorised as LR-2 if <20mm and LR-3 if ≥20mm.
Findings with appearances suggestive of either focal nodular hyperplasia or adenoma should usually be categorised as LR-3 as in patients at high risk of HCC these are a diagnosis of exclusion.
With caution they may be categorised as LR-2 however LR-1 should not be used for these lesions.
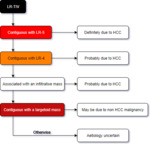
LR-M
If a mass has a targetoid appearance the category LR-M should be used.
This includes rim-enhancement in the arterial phase,
peripheral washout or delayed central enhancement as well as a concentric pattern of diffusion restriction.
These appearances are usually secondary to peripheral hypercellularity with central fibrosis or necrosis/ischaemia.
While atypical HCC can have these appearances,
this is more commonly seen in non-hepatocellular malignancy.
LR-M can also be assigned in a non-targetoid lesion if a finding does not meet the criteria for LR-5 or LR-TIV and does have one of the following features:
- An infiltrative appearance.
- Marked diffusion restriction.
- Necrosis in a non-targetoid pattern.
- Other feature(s) suggestive of a non-HCC malignancy which should be specified in the report.
LR-TIV
If on assessment there is unequivocal soft tissue within a vein that enhances then LR-TIV (Tumour-in-vein) should be assigned.
Once LR-TIV has been assigned an assessment of the most likely aetiology should be made as per Fig. 2
LR-3 to 5
If a finding cannot be assigned to one of the aforementioned categories then it is likely to be a lesion of hepatocellular origin.
An assessment of the likelihood of HCC should be made.
This depends on a number of factors:
- The size of the lesion
- Does the lesion demonstrate arterial phase enhancement?
- The number of "Major features" present
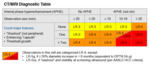
These are then cross-referenced against the CT/MRI diagnostic table,
Fig. 3.
There are strict definitions as to what the major criteria used in this table are as summarised below in Table 2:
| Major Feature |
Definition |
Example |
|
Arterial phase enhancement
(APHE)
|
Enhancement of the lesion in whole or part,
in the arterial phase.
This must be higher than that of the background liver and must be non-rim enhancement (this would be classified as LR-M). |
Fig. 4,
Fig. 5,
Fig. 6,
Fig. 9,
Fig. 11, Fig. 14, Fig. 15, Fig. 16,
Fig. 19 |
|
Size
|
Measure the largest outer-to-outer diameter,
including any "capsule".
This should be measured on the sequence which the lesion is clearest.
However,
the arterial phase should not be used as any corona enhancement can lead to size over estimation while DWI should not be used as it is susceptible to anatomical distortion. |
N/A |
| Washout |
The observation demonstrates a temporal reduction in enhancement,
in whole or part,
relative to an earlier phase of enhancement.
This does not include the transitional or hepatobiliary phase if a hepatocyte specific contrast agent has been used. |
Fig. 7,
Fig. 9,
Fig. 11,
Fig. 12, Fig. 14, Fig. 15, Fig. 16 |
| Enhancing "Capsule" |
A border around an observation that is thicker than that of background nodules.
This is smooth,
sharp and enhances in the portal venous,
delayed or transitional phases. |
Fig. 14 |
| Threshold growth |
Lesion has increased in size by at least 5mm and one of:
- ≥50% increase in size in less than or equal to 6 months
- ≥100% increase in size in greater than 6 months
- Previously unseen on CT/MRI within the last 2 years,
now at least 10mm.
Measurements must be consistent between serial examinations
|
Fig. 9, Fig. 14 |
Table 2. Major imaging features of HCC and their definitions.
Ancillary Features
Ancillary features can be used at the discretion of the radiologist to improve detection,
increase confidence in an observation or to adjust the category as described above.
Some features favour malignancy in general while others favour HCC specifically (this is a new distinction in the 2017 edition).
It is important to note that the inverse of these features cannot be used to imply the opposite.
The ancillary features are defined in Table 3 below:
| Features which favour malignancy but not HCC in particular |
| Feature |
Definition |
Example |
|
US visibility as a discrete nodule
(New in 2017)
|
Corresponding nodule is visible on unenhanced US |
Fig. 9 |
| Subthreshold growth |
Increased size of mass which is unequivocal but does not meet the definition of threshold growth (Table 2) |
|
| Corona enhancement |
Enhancement around the observation which is visible in the late arterial/portal venous phase |
|
| Fat sparing in a solid mass |
Paucity of fat either within a lesion relative to a background fatty liver or within a nodule inside a fatty nodule |
Fig. 16 |
| Restricted diffusion |
DWI intensity higher than liver,
not attributable to T2 shine through |
Fig. 9, Fig. 16, Fig. 17, Fig. 18 |
| Mild-moderate T2 hyperintensity |
Lesion is mildly to moderately higher than the background liver on T2W imaging.
Similar to a non-iron overloaded spleen |
Fig. 7, Fig. 15 |
| Iron sparing in a solid mass |
Paucity of iron in a mass relative to either an iron-overloaded liver or a siderotic external nodule |
Fig. 4 |
| Transitional phase hypointensity |
Intensity in the transitional phase unequivocally less than the liver |
Fig. 13 |
| Hepatobiliary phase hypointensity |
Intensity in the hepatobiliary phase unequivocally less than the liver |
Fig. 4,
Fig. 6,
Fig. 10,
Fig. 11, Fig. 14, Fig. 16, Fig. 17, Fig. 18 |
|
| Features favouring HCC in particular |
| Feature |
Definition |
Example |
|
Non-enhancing "Capsule"
(Previously "distinctive rim")
|
As for enhancing "capsule" (See table 2) but demonstrating no enhancement |
Fig. 10 |
| Nodule-in-nodule architecture |
A smaller inner nodule within an outer nodule which has different imaging characteristics |
Fig. 11 |
| Mosaic architecture |
Randomly distributed internal nodules within a lesion with different imaging characteristics |
Fig. 12 |
| Fat in mass,
more than adjacent liver |
Greater concentration of fat within a lesion,
or part of a lesion, than in the adjacent liver |
Fig. 13 |
| Blood products in mass |
Intra or perilesional haemorrhage in the absence of intervention,
biopsy or trauma |
Fig. 15 |
|
| Features favouring benignity |
| Feature |
Definition |
Example |
| Size stability > 2 years |
No significant change in size of a lesion over at least two years |
|
| Size reduction |
Unequivocal and spontaneous decrease in size of an observation.
This should not be due to resorption of blood products or treatment.
It must not be attributable to artefact or difference in imaging techniques or measurements |
Fig. 6 |
| Parallels blood pool |
The pattern of enhancement follows that of the blood pool over time |
Fig. 8 |
| Undistorted vessels |
If vessels cross an observation they are not displaced or deformed |
Fig. 20 |
| Iron in mass,
more than liver |
Higher concentration of iron within a lesion compared to the background liver |
Fig. 19 |
| Marked T2 hyperintensity |
Intensity on T2W imaging is similar to that of the bile ducts or other fluid filled structures |
Fig. 8 |
| Hepatobiliary phase isointensity |
Intensity in the hepatobiliary phase identical to that of the liver |
Fig. 5, Fig. 19, Fig. 21 |
|
Table 3.
Ancillary imaging features for use in the assessment of observations.
Self Test
The diagnosis/LI-RADS classification has intentionally been omitted from the provided cases.
This provides a means of self-assessment.
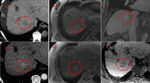
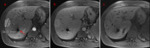
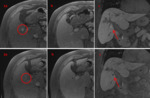
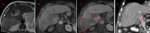
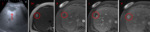
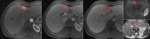
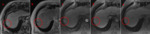
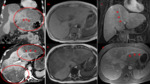
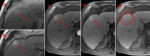
Please review the 17 cases, Fig 4-20 in the sidebar on the right.
Use the information on this page to assign a LI-RADS score to the target lesion.
The answers are provided in the next section (Conclusion).