PICC are polyurethane catheters whose insertions are in a peripheral vein but the location of its distal end is central in superior vena cava.
The material provides a biocompatible and radiopaque line and has been proved to use for long periods of time with the proper care.
The insertion of PICC guided by an imaging technique (Eco Directed Seldinger method and fluoroscopic control or confirmation of catheter tip by ECG.) has become the method of choice in many centers,
reducing morbidity and mortality,
reducing costs and hospital stays.
The implantation of this catheter is a procedure that can be performed by both the radiologist and the nursing staff,
and does not require preoperative tests.
Therefore there must be training in the choice,
insertion and care of these catheters to handle them with a technical and scientific rigor.
Indications
-
Administration of IV fluids,
medications,
or blood products,
either in large quantities or over a prolonged period of time (>6 days) ;
-
Administration of medications that are harmful to peripheral veins ( pH less than 5,
greater than 9 or osmolarity greater than 600 mOsm / L.
)(eg,
chemotherapy);
-
Long-term access to the central venous system for repeated procedures,
such as blood sampling; and
-
Poor or inaccessible peripheral venous access
In our experience in the recent years,
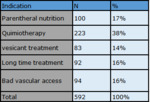
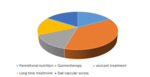
the most frequent indications for the placement of PICC line were the administration of chemotherapy in 38% (N = 223) parenteral nutrition 17% (N = 100) poor venous access or the difficulty of placing a peripheral path 16% (N = 94),
the forecast of a prolonged treatment by the attending physician that was not Qt or NTP 16% (N = 92)
Fig. 1 Fig. 2
Insertion
A vein in the arm is the most common point of insertion (tab.
1) and the distal tip of the catheter must terminate in the superior vena cava,
the inferior vena cava,
or the proximal right atrium.
(4)
Fig. 3
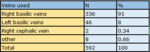
Selection of vein used for insertion of picc in our center in the period from 2013 to 2016
There are 2 methods of bedside PICC insertion: the peel-away cannula technique and the modified-Seldinger technique.
In our institution the most common technique used is the ultrasound located Seldinger technique: by ultrasound a vein is located and accessed with an intravenous needle.
A guide wire is threaded into the needle or cannula several centimeters,
then the needle or cannula is removed,
leaving the guide wire in place.
A nick is made in the skin beside the guide wire,
and an introducer sheath with dilator is inserted over the guide wire.
The guide wire and dilator are removed,
and the catheter is advanced through the introducer sheath,
which is then pulled back and peeled away.
The ultrasound is useful for locating and help access the vein,
increase the insertion success rate ( 65-74% success in the "blind" implant vs 86-95% success in image-guided implant.),
and also facilitates access to larger veins higher in the upper arm associated with a lower incidence of thrombosis,
phlebitis and catheter migration than antecubital fossa insertions.
Advantages.
Can be inserted at bedside by both the radiologist and trained nurses,
which reduces costs and waiting list.
Comfort and safety of the patient both at the time of the insertion procedure and after being able to administer IV home treatments.
The venous structures are preserved by avoiding multiple punctures and manipulations by replacing IV lines.
The insertion of the PICC does not present a risk of pneumothorax and considerably reduces the risk of hemorrhage.
The PICC has multiple lumens (single,
dual and triple lumen catheters) allowing different substances to be administered simultaneously.
Reliable peripheral venous access for long and short term.
Reduces the risk of infection of the patient.
Complications.
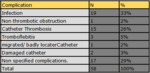
During the years 2013 to 2016 a compilation of PICCs placed under ultrasound guidance has been made in our institution.
We obtained a sample of 592 patients,
of whom 58 had complications,
ie 9.7%,
with catheter infections being the most common complication.
Only 22 of our 552 patients required the removal of the PICC due to complications.
Fig. 5
Care,
Prevention and treatment of complications
Fig. 6
General recommendations :
Always wash hands before manipulation.
When greater than 6 days of therapy are anticipated use of PICC is strongly recommended.
Obstruction prevention:
NSS Should be flush After blood Sampling,
before and after administering medication or fluids.
Thrombosis prevention:
Heparin 6 mL (10 U/ml) each lumen following NSS flush and whenever ordered by the physician,
after blood sampling,
when converting from continuous to intermittent use,
when lumen is not in continuous use,
at discharge If not used daily (2 ml 1000 U/ml each lumen once weekly)
Post implantation care:
To avoid bleeding it's recommended to put an dressing for compression.
Statlock dressing change if it's stained.
Fig. 7
Insertion point care.
A statlock device and a semi-permeable polyurethane sterile transparent dressing in the appropriate size should be used,
labelled and changed every 7 days or when it becomes damp,
loose,
soiled or if patient develops problems at the site that require further inspection.
The use topical antibiotic ointment or cream is not recommended.
When the patient showers the site,
catheter and connecting devices should be covered with dressing.
Arterial catheter should be avoided in the same arm as PICC but can be placed in the same arm if medically indicated.
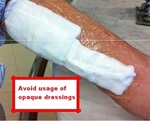
Do not place opaque dressing that does not allow to see the insertion area for complications.
Fig. 8
Intraluminal care.
Treat each connection independently
Aspirate to check permeability and Wash with 10 ml of SF
PowerPicc catheters: Closure system type "clamp".
Sealing with heparin and positive pressure technique
PowerPicc catheter SOLO2: With proximal valve.
There is no precise heparin.
Sealing with SF and positive pressure technique
Cleaning connection with Alcohol 70% or Alcoholic Chlorhexidine 2%
Fig. 9
Obstruction management:
Dilute Urokinase 100000 U in 1 ml,
in a 10 mm syringe and pass the volume that admits the catheter without going to blood.
Economic comparison of PICC line and peripheral and central catheters.
Using as a reference the approximate costs in our hospital in Valencia,
Spain with the approximate costs of the materials and basic salaries of health personnel:
Peripheral catheters are routinely placed by nurses (average salary of 16 euros / hr),
CVC by medical staff together with nurses and PICC by medical team (average salary 26 € / hr) and nursing personal or a specialized nursing team depending on the case,
the approximate cost for the placement of a PICC (€ 170) per se far exceeds the cost of a peripheral route (€ 10) or a CVC (€ 80).
The ultrasound guidance provides a successful implant in the first attempt of the PICC of up to 86-95% against 74 - 88% in peripheral pathways and up to 12% of patients requires 3 or more attempts,
which in many patients multiplies the cost of placement,
on the other hand,
a peripheral route must be changed every 72 hours,
so in patients who prolong the use of a peripheral route for more than 7 days requires at least 3 peripheral catheter implants,
with a higher frequency of complications ( 41% phlebitis,
28% occlusion) and that increase in frequency for each day of placement.
Regarding CVCs,
the generalized use of ultrasound guidance reduces the frequency of complications due to puncture such as arterial punctures,
hematomas and pneumothorax (approximately 11% of complications).
On the other hand,
there is an increased risk of infections compared to the PICC,
although the complications of a CVC they are not much more frequent than those presented with a PICC (10 vs 11%) they are more serious (cervical hematoma,
pneumothorax,
hemothorax,
sepsis) with high treatment costs and when they are present,
they also lengthen the hospital stay,
assuming a greater economic burden.
Fig. 10 Fig. 11
The PICC also under ultrasound guidance is prefered by patients rather than CVC because of its more comfortable and durable for them.