Type:
Educational Exhibit
Keywords:
Education and training, Diagnostic procedure, MR, CT, Conventional radiography, Thorax, Paediatric, Lung
Authors:
M. PITARCH DIAGO1, C. Martin Martinez1, V. P. Beltrán Salazar1, C. Duran Feliubadaló1, D. Rodriguez Martinez1, B. Del Rio2, F. Bosch Barragan1, A. Gonzalez Lopez1, A. B. A. B. CASTRO GARCIA2; 1Sabadell/ES, 2Terrassa/ES
DOI:
10.1594/ecr2018/C-3056
Findings and procedure details
We use a literature review and images from our case series to describe and illustrate the different conditions that can present with unilateral hyperlucent hemithorax in pediatric patients.
Causes of pulmonary asymmetry in children can be classified in 5 categories according to whether the abnormality lies in the lung parenchyma,
pleural space,
chest wall,
lung vascularization,
or airway (Table 1).
A. Abnormalities in the lung parenchyma:
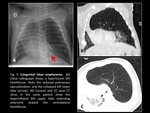
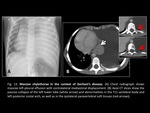
- Congenital lobar emphysema (Fig. 5): typically presents with a large,
hyperlucent hemithorax.
It can affect any lobe,
though the left upper lobe is the most common.
It may be secondary to bronchomalacia,
endobronchial lesions,
or extrinsic bronchial compression,
all of which result in airway luminal narrowing and obstruction.
In the first hours after birth,
congenital lobar emphysema appears on chest radiographs as an area of increased lung opacity due to trapped fetal lung fluid,
which is replaced with air during the following days.
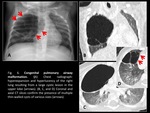
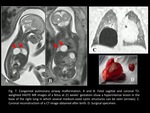
- Congenital pulmonary airway malformation (formerly known as congenital cystic adenomatoid malformation) (Fig. 6,
Fig. 7): characterized by multiple lung cysts of variable size with very thin walls.
They are classified into 5 types (0–4) depending on the number and size of the cysts.
Types 1–4 involve a single lobe in 95% of cases (with no predilection for any particular lobe); type 0 involves the trachea or a main bronchus and these patients typically die in utero.
The radiographic appearance of congenital pulmonary airway malformation varies according to the number and size of the cystic spaces forming the lesion and whether there is superimposed infection.
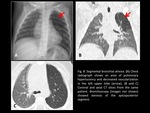
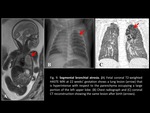
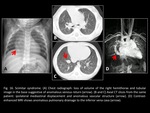
- Segmental bronchial atresia (Fig. 8,
Fig. 9): depending on the level of obstruction (lobar,
segmental,
or subsegmental),
the area of entrapped air can be larger or smaller.
Segmental bronchial atresia typically involves apical-posterior segments of the upper lobe and is usually accompanied by a branching tubular image that corresponds to a “mucocele”.
- Swyer–James syndrome,
Swyer–James–Macleod syndrome,
or constrictive bronchiolitis: a condition that generally develops secondary to infectious processes.
Involvement is usually bilateral but asymmetrical.
It manifests as a small unilateral hyperlucent lung with a decrease in the number and caliber of pulmonary vessels.
This is “acquired pulmonary hypoplasia”.
- Large post-inflammatory pneumatocele.
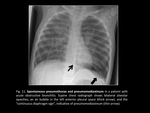
- Pulmonary interstitial emphysema (Fig. 10): in neonates,
it is a type of barotrauma due to positive-pressure ventilation.
It can be segmental or lobar,
unilateral or bilateral.
- Post-pneumonectomy
B. Pleural space abnormalities:
- Anterior pneumothorax (Fig. 11): air accumulated in the anterior pleural space can be seen as a unilateral hyperlucent hemithorax on supine chest radiographs.
- Contralateral pleural effusion: pleural effusion can cause the contralateral hemithorax to appear hyperlucent (false finding).
Parapneumonic pleural effusion is the most common in pediatrics (Fig. 12).
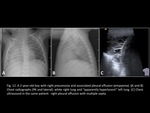
Others: neoplastic disease,
chylothorax (Fig. 13),
etc.
- Left diaphragmatic hernia (congenital or acquired) in which air-filled stomach or small-bowel loops enter the thorax.
C. Chest wall abnormalities:
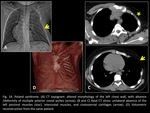
- Poland syndrome (Fig. 14): unilateral congenital aplasia of the pectoral muscles.
It can be associated with agenesis of other muscles in the ipsilateral hemithorax.
It is more common in males and is usually asymptomatic.
D. Abnormalities in pulmonary vascularization:
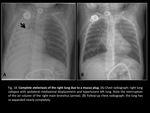
- Lung agenesis: this congenital defect in lung development represents a spectrum of abnormalities ranging from pulmonary hypoplasia to lobar agenesis-aplasia.
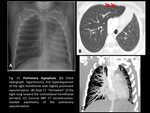
- Pulmonary hypoplasia (Fig. 15): partial agenesis more commonly affects the upper and middle lobes of the right lung; it is usually associated with other abnormalities such as anomalous venous drainage (scimitar syndrome (Fig. 16)).
- Other congenital vascular anomalies: proximal interruption of the pulmonary artery,
unilateral pulmonary vein atresia,
unilateral congenital pulmonary lymphangiectasia.
- Pulmonary embolism: thromboembolism alters lung perfusion,
sometimes manifesting as unilateral lung opacities and pulmonary asymmetry on chest radiographs.
E. Airway abnormalities:
Complete airway obstruction results in pulmonary atelectasis,
which is accompanied by hyperexpansion and hyperaeration of the contralateral lung.
By contrast,
partial obstruction results in air trapping.
The most common causes of airway obstruction in pediatrics are foreign bodies and mucus plugs.
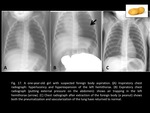
- Aspiration of a foreign body (Fig. 17): most common between the ages of 6 months and 3 years,
any object can be aspirated (typically nuts) and they are not usually radiopaque.
Clinical suspicion is very important.
Foreign body aspiration manifests as a unilateral hyperlucent enlarged hemithorax that does not change with respiration (air trapping).
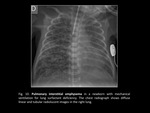
- Mucus plugs: occur in the context of viral infections of the lower respiratory tract or in patients with asthma (Fig. 18).
- Other,
much less common causes of intrinsic airway obstruction: endobronchial tumor or selective intubation.
- Extrinsic bronchial compression: mediastinal cysts (e.g.,
bronchogenic cyst),
mediastinal tumors or adenopathies,
or vascular anomalies such as pulmonary artery sling.