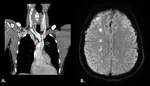
1. Classification Of Border Zone Infarcts
Border zone infarcts can be divided into two main types: external (cortical) and internal (subcortical); however,
mixed types also have been described.
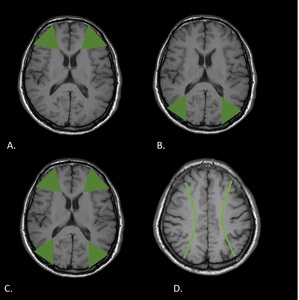
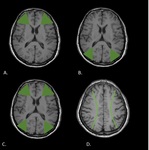
Fig. 2: T1WI shows external border zones. A. Anterior. B. Posterior. C. Both types. D. Paramedian white matter.
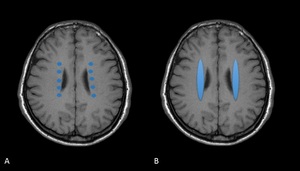
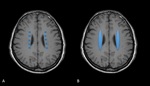
Fig. 3: T1WI shows Internal border zones. A. Partial B. Confluent
1.1.
External border zone infarcts (cortical) Fig. 2
These infarcts are located between major arterial territories and can be subdivided into:
- Anterior : between ACA and MCA. Fig. 4
- Posterior: between MCA and PCA. Fig. 5
- Paramedian white matter: between ACA and MCA. Fig. 5, Fig. 6
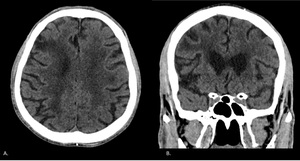
Fig. 4: Axial (A) and Coronal (B) CT plain images of a 77-year-old male show a right anterior external border zone infarct (at the junction of the right anterior and middle cerebral arteries).
References: Department of Radiology, McGill University Health Center, Montreal / Canada 2017
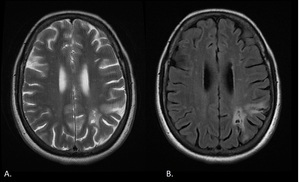
Fig. 5: Axial T2 (A) and FLAIR (B) images obtained in a 52-year-old woman show chronic infarct in the left posterior external border zone.
References: Department of Radiology, McGill University Health Center, Montreal / Canada 2017
1.2.
Internal border zone infarcts (subcortical) Fig. 3, Fig. 8
These infarcts are located between perforating arteries,
such as:
- Between the lenticulostriate and MCA,
which are the most commonly seen.
- Between the lenticulostriate and ACA.
- Between the Heubner and ACA.
- Between the anterior choroidal and MCA.
- Between the anterior choroidal and PCA.
From the imaging perspective they can be divided into:
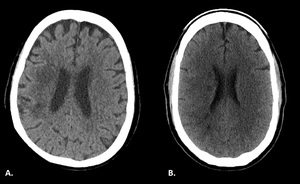
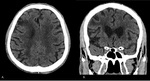
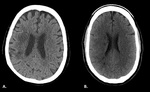
Fig. 8: Internal border zones. A. CT plain of a 71 year-old female shows right internal border zone infarcts (confluent type). B. CT plain of a 43-year-old male shows multiple right internal border zone infarcts (partial type).
References: Department of Radiology, McGill University Health Center, Montreal / Canada 2017
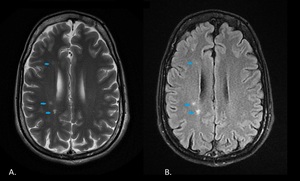
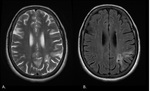
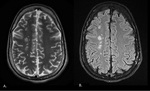
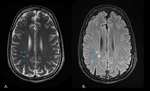
Fig. 9: Axial T2 (A) and FLAIR (B) images obtained in a 35-year-old man show multifocal hyperintensities along the right internal border zone (blue arrows).
References: Department of Radiology, McGill University Health Center, Montreal / Canada 2017
2. Pathophysiology Of Border Zone Infarcts
The pathophysiology of border zone infarcts has been studied for a long time and still remains controversial.
They may be preceded by precipitating circumstances that induce hypotension or hypovolemia.
Traditionally,
hemodynamic impairment has been widely accepted as the cause of external border zone infarcts,
but microemboli may also contribute to it.
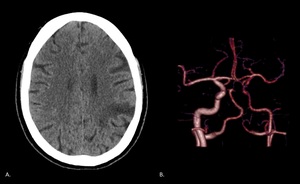
Fig. 11: A. Axial plain CT obtained in a 52 year-old woman shows chronic left posterior external border zone infarct. B. 4D CTA of the same patient shows stenosis of the left internal carotid artery in its extra and intracranial segments.
References: Department of Radiology, McGill University Health Center, Montreal / Canada 2017
External border zone infarcts are induced by a microembolic mechanism associated with hypoperfusion.
Microemboli from the heart or atherosclerotic plaques in major arteries may propagate to cortical border zones which have lower perfusion and therefore,
limited ability to wash out these emboli.
However,
they have a better chance of developing collateral supply through leptomeningeal or dural anastomoses (because they are closer to the cortical surface where penetrating arteries originate); thus,
have better prognosis. Fig. 11, Fig. 12
Studies have shown that unilateral external border zone infarcts are associated with microemboli; In contrast,
bilateral ones are more likely to be caused by underlying hemodynamic impairment.
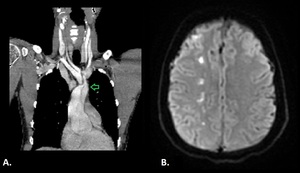
Fig. 14: A. Chest CTA obtained in a 35 year-old man shows a dissection of the aortic arch (type A), that seems to extend into the right brachiocephalic trunk and the origin of the left common carotid artery (arrow). B. DW MRI of the same patient shows restricted diffusion along the right paramedian white matter (External border zone infarct).
References: Department of Radiology, McGill University Health Center, Montreal / Canada 2017
Internal border zone infarcts are mainly caused by arterial stenosis or occlusion,
or hemodynamic compromise because of several characteristics: vulnerability of the vascularization of the centrum semiovale and impaired cerebral vasoreactivity associated with oxygen metabolism failure.
Internal border zones are supplied by deep perforating branches of the anterior and middle cerebral arteries; not only do these branches have lower perfusion pressure,
but also have little collateral supply; as a result,
they are more susceptible to ischemic insults in the setting of hemodynamic compromise.
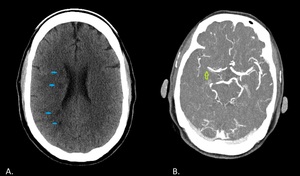
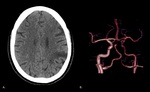
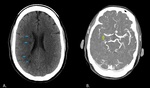
Fig. 13: A. CT plain obtained of a 43-year-old male shows multiple right internal border zone infarcts (blue arrows). B. CTA MIP of the same patient shows occlusion of the distal M1 segment of the right middle cerebral artery (green arrow).
References: Department of Radiology, McGill University Health Center, Montreal / Canada 2017
3. Clinical Features
The most common clinical features of border zone infarcts are altered mental status,
syncope,
hypotension,
weakness of the hands and coma.
4. Imaging Characteristics
External border zone infarcts are generally wedge-shaped,
cortically based,
located at the junction of major arterial territories,
as previously described.
However,
they can also present as pseudolaminar necrosis (curvilinear,
gyriform). Fig. 4, Fig. 5
Internal border zone infarcts are located in the deep white matter,
between the deep and superficial perforating arteries of the MCA,
within the centrum semiovale.
The partial type can present either as a single lesion or multiple as a “rosary-like”,
“string of pearls” pattern in linear orientation (antero-posterior),
parallel to lateral ventricle and can resemble multiple emboli.
In contrast,
the confluent type is a large,
“cigar-shaped” infarction alongside the lateral ventricle. Fig. 9
On CT,
they tend to be hypodense,
enhacement can be seen in subacute phase on CECT.
On MRI,
on T1WI,
in an acute phase they have low signal intensity while in a subacute phase gyriform cortical hyérintensity can be seen (in external type).
On T2WI and FLAIR they have high signal intensity in involved areas.
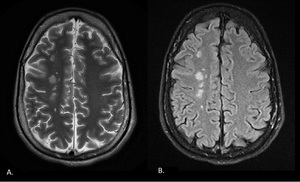
Fig. 6: Axial T2 (A) and FLAIR (B) images obtained in a 35-year-old man show multifocal hyperintensities along the paramedian white matter. (External border zone infarct).
References: Department of Radiology, McGill University Health Center, Montreal / Canada 2017
On DWI,
they have restricted diffusion (hyperintense on DWI and hypointense on ADC).
Fig. 7,
Fig. 10 This sequence not only depicts better the location of border zone infarcts in relation to the vessels,
but also enables differentiation between acute and chronic stroke.
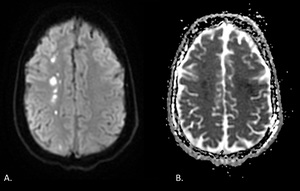
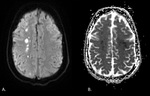
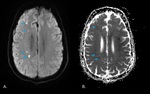
Fig. 7: Diffusion-weighted images and ADC map obtained in a 35-year-old man show multifocal lesions with restricted diffusion along the right centrum semiovale.
References: Department of Radiology, McGill University Health Center, Montreal / Canada 2017
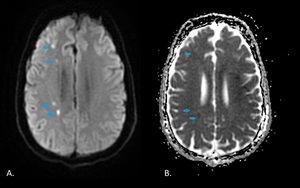
Fig. 10: Diffusion-weighted images and ADC map obtained in a 35-year-old man show multifocal lesions with restricted diffusion along the right internal border zones (blue arrows).
References: Department of Radiology, McGill University Health Center, Montreal / Canada 2017
Perfusion CT and MR can help identify the cause of the border zone infarct,
for instance,
hypotension,
embolism,
or severe stenosis of a proximal vessel.
Fig. 12 Three patterns have been identified:
- Normal perfusion may be seen in patients with a transient perfusion deficit due to hypotension in the absence of large artery disease.
- Localized perfusion deficit may be seen in patients with infarcts due to cardiac or embolic causes.
Note that the area of hypoperfusion matches the area of restricted diffusion.
- Extensive perfusion deficit may be seen in patients with severe stenosis or occlusion of large arteries.
Note that there is a mismatch between the area of hypoperfusion and the area of restricted diffusion.
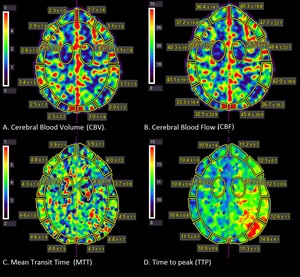
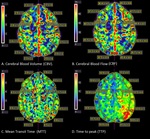
Fig. 12: Perfusion CT maps of the same patient show reduced cerebral blood volume and reduced cerebral blood flow, and increased mean transit time and time to peak in the left posterior border zone.
References: Department of Radiology, McGill University Health Center, Montreal / Canada 2017
5. Treatment and Prognosis
It is important to identify the cause of the border zone infarcts in order to give appropriate treatment to these underlying conditions.
Patients with external border zone infarcts have better prognosis which can be explained by the better chance they have of developing collateral supply.
Patients with internal border zone infarcts are more prone to poor prognosis and have higher risk for future stroke.