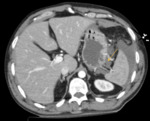
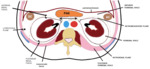
1. PERITONEAL CAVITY
1.1.
The peritoneal cavity is divided into interconnecting spaces,
the supramesocolic and inframesocolic spaces and the pelvic cavity.
1.1.1.
Supramesocolic compartment
(intraperitoneal spaces above the transverse colon)
- contains -
stomach
liver
spleen
Further,
the supramesocolic space is arbitrarily subdivided into right and left supramesocolic spaces.
Spaces
The right supramesocolic space includes:
Right subphrenic space (Fig.1)
Hepatorenal space (Morison's pouch) (Fig.2)
Lesser sac (Fig.3)
The left supramesocolic space has two subspaces:
Left perihepatic space
anterior left perihepatic space (Fig.4)
posterior left perihepatic space (or gastrohepatic recess) (Fig.4)
Left subphrenic space
posterior left subphrenic space / perisplenic space (Fig.4)
anterior left subphrenic space (Fig.5)
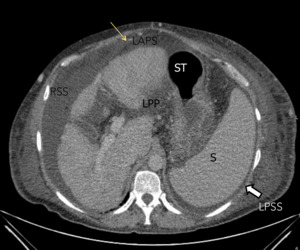
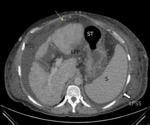
Fig. 1: Axial CT image, obtained in a 55-year-old man shows the falciform ligament (yellow arrow) which is outlined by ascites in this patient with chronic hepatopathy. There is fluid in the left anterior perihepatic space (LAPS) and in the right subphrenic space (RSS), which are separated by the falciform ligament.
The left posterior perihepatic space (LPP) lies parallel to the lesser curvature of the stomach (ST), and it is limited posteriorly and on the right by the gastrohepatic ligament (not showed).
L, Liver; RSP, right subphrenic space; LPSS, left posterior subphrenic space; ST, stomach; .S, Spleen; LPP, Left posterior perihepatic space.
References: Hospital de Braga, Portugal

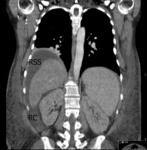
Fig. 2: Coronal CT image in a 66-years-old man shows the right subhepatic space or Morrison space, between the liver and the right kidney (arrow).
The right subphrenic space (RSS) communicates with the right percolic space (RC) and the right subhepatic space (arrow).
References: Hospital de Braga, Portugal
The right subphrenic space (RSS) communicates with the right pericolic space (RC) and the right subhepatic space (arrow).

Fig. 3: Coronal (A) and axial (B) CT image shows the superior (LSs) and inferior (LSi) recesses of the lesser sac in the supramesocolic space.
References: Hospital de Braga, Portugal

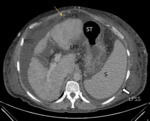
Fig. 4: The left anterior perihepatic space (LAPS). Axial CT image, obtained in a 55-year-old man shows the falciform ligament (yellow arrow) which is outlined by ascites in this patient with chronic hepatopathy. The left posterior perihepatic space (LPP) lies parallel to the lesser curvature of the stomach (ST), and it is limited posteriorly and on the right by the gastrohepatic ligament (not showed).
The left posterior subphrenic (or perisplenic) (LPSS) space surrounds the spleen.
L, Liver; RSP, right subphrenic space; LPSS, left posterior subphrenic space; ST, stomach; S, Spleen.
References: Hospital de Braga, Portugal
Ligaments
Right and left coronary ligaments - the right and left coronary ligaments defines the margins of the bare area of the liver.
Gastrosplenic ligament (Fig.
6) - extends from the greater curvature of the stomach to the spleen.
Gastrohepatic ligament (Fig 7) - the gastrohepatic ligament attaches the lesser curve of the stomach to the liver and contains the coronary vein and left gastric artery.
Hepatoduodenal ligament – the hepatoduodenal ligaments and the gastrohepatic,
together compose the lesser omentum.
The hepatoduodenal ligament contains the portal vein,
hepatic artery,
common hepatic and central cystic ducts,
and nodes of the porta hepatis.
Phrenicocolic ligament (Fig.
8) – the phrenicocolic ligament extends from the splenic flexure to the diaphragm.
This ligament is a relative barrier to fluid spread from the left paracolic gutter to the left subphrenic space.
Splenorenal ligament – extends from the tip of the pancreas to the splenic hilum.
Falciform ligament (Fig.
8) - the falciform ligament,
which is the remnant of the ventral part of the ventral mesentery,
contains the obliterated umbilical vein.

Fig. 6: Coronal CT image of the upper abdomen, obtained in a 53-year-old man, shows ascites outlining the gastrosplenic ligament (yellow arrow), which contains the short gastric vessels.
References: Hospital de Braga, Portugal

Fig. 7: Coronal CT image of the upper abdomen, obtained in a 63-year-old man, shows ascites outlining gastrohepatic ligament (yellow arrow).
References: Hospital de Braga, Portugal

Fig. 8: Phrenicocolic ligament (yellow arrow).
References: Hospital de Braga, Portugal

Fig. 9: Axial CT shows fluid in the left anterior perihepatic space (LAPS) and in the right subphrenic space (RSS), which are separated by the falciform ligament (yellow arrow).
References: Hospital de Braga, Portugal
1.1.2.
Inframesocolic compartment
(posterior to the greater omentum,
below the transverse
mesocolon and medial to the ascending and descending colon)
- contains -
small bowel
ascending and descending colon
It is divided into right and left by the oblique small bowel mesentery.
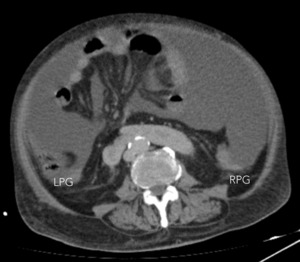
Fig. 10: Lateral to the ascending and descending colon are the right and left paracolic gutters. LPG, left paracolic gutter. RPG, right paracolic gutter.
References: Hospital de Braga, Portugal
The right paracolic gutter is continuous superiorly with the right perihepatic and subphrenic spaces.
The phrenicocolic ligament is a relative barrier to fluid spread from the left paracolic gutter to the left subphrenic space.
1.1.3.
Pelvic peritoneal cavity

Fig. 11: In the pelvis, the peritoneum reflects over the pelvic organs, creating the most gravity-dependent site for fluid accumulation, corresponding to the recto-vesical pouch in males and the recto-uterine pouch (pouch of Douglas) in females (asterisk).
Anteriorly, the medial umbilical fold (yellow arrow), which contain the obliterated umbilical arteries, divide the paravesical space, into lateral (inguinal fossae) and medial (supravesical fossae) compartments. The inguinal spaces are further subdivided into medial and lateral inguinal fossae, by the lateral umbilical folds (blue arrows), which contains the inferior epigastric artery, corresponding to the sites of indirect and direct inguinal hernias, respectively.
References: Hospital de Braga, Portugal
1.2.
A group of abnormalities can arise primarily from mesentery and are referred as Primary Mesenteropathies and includes:
1.2.1.
Malrotation
The presence of an abnormal SMA and SMV relationship,
which have an inverted relationship with the superior mesenteric artery (smaller and more circular) on the right and superior mesenteric vein on the left side,
and the presence of a large bowel predominantly on left and small bowel predominantly on the right suggest the diagnosis of intestinal malrotation.
Intestinal malrotation is a congenital anatomical anomaly that results from an abnormal rotation of the gut as it returns to the abdominal cavity.
This condition may predispose to midgut volvulus and internal hernias.
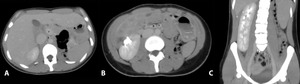
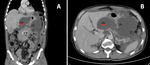
Fig. 12: A) Axial CT of a 7-year-old girl. Axial contrast-enhanced CT scan obtained at the level of the upper abdomen shows an inverted relationship between superior mesenteric artery (a) and superior mesenteric vein (v).
B) Contrast-enhanced CT at a level below.
C) Coronal contrast-enhanced CT shows the presence of a crossed fused renal ectopia referring to an anomaly where the kidneys are fused and located on the same side of the midline (right).
References: Hospital de Braga, Portugal
1.2.2.
Volvulus
Intestinal volvulus is a condition in which the bowel twists around its mesentery.

Fig. 13: The “whirl sign” of cecal volvulus (blue arrow). Contrast-enhanced CT image shows a dilated and stool-filled cecum located in the left upper quadrant. This appearance results from twisted collapsed bowel with enhancing engorged vessels radiating from the twisted bowel.
References: Hospital de Braga, Portugal
1.2.3.
Internal hernias
Internal hernias are protrusions of a viscous through an orifice (congenital or acquired) or a retroperitoneal fossa.
Congenital internal hernias are classified as paraduodenal (left and right),
pericaecal,
foramen of Winslow,
transmesenteric,
transomental,
and sigmoid depending on the involved area.

Fig. 14: A 64-year-old man with abdominal pain. CT image showed a clustered dilated small-bowel in the right mid abdomen consistent with an acquired internal hernia after an abdominal surgical procedure.
References: Hospital de Braga, Portugal
1.2.4.
Inflammatory

Fig. 15: A 65-year-old man with mesenteric panniculitis. Axial contrast-enhanced CT showed an increase in the density of the fat in the mesentery (misty) and tiny nodes (asterisk).
References: Hospital de Braga, Portugal
1.2.5.
Omental infarction

Fig. 16: A 67-year-old man with omental infarction. Contrast-enhanced CT performed for acute LLQ pain shows a focal area of increased omental fat stranding, vascularity and whorled appearance (circle).
References: Hospital de Braga, Portugal
1.2.1.
Mesenteric neoplasms

Table 1: Mesenteric neoplasms.
References: Hospital de Braga, Portugal
1.3. A group of infectious,
inflammatory,
traumatic and neoplastic mesenteric abnormalities can spread to secondarily involve the mesentery.
Peritoneal carcinomatosis is the most common diffuse peritoneal disease and corresponds to the intraperitoneal dissemination of a tumor.

Fig. 17: Contrast-enhanced abdominal CT scan shows omental thickening (arrows) and ascites caused by metastases from colon cancer.
References: Hospital de Braga, Portugal

Fig. 18: Pseudomyxoma Peritonei. Contrast-enhanced TC showing low attenuation fluid throughout the peritoneum, omentum and mesentery, with scattered (curvilinear or punctate) calcifications consistent with Pseudomyxoma Peritonei.
References: Hospital de Braga, Portugal
2.
RETROPERITONEAL CAVITY
The retroperitoneum extends from the pelvic brim inferiorly to the diaphragm superiorly.
It is bounded ventrally by the posterior parietal peritoneum and dorsally by the transversalis fascia.
It is divided into three distinct compartments:
- the anterior pararenal space,
located between the parietal peritoneum and the anterior renal fascia;
- the perirenal space,
located between the anterior renal fascia and the posterior renal fascia;
- the posterior pararenal space,
bounded by the posterior renal fascia (PRF) and the transversalis fascia (TF).
2.1 Anterior pararenal space
(located between the parietal peritoneum and the anterior renal fascia)
- contains -
ascending and descending colon
2nd to 4th portions of the duodenum
pancreas
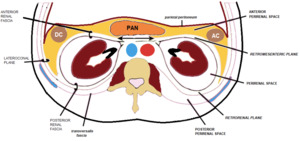
Fig. 20: Representation of the retroperitoneal cavity - anterior pararenal space (yellow).
References: Hospital de Braga, Portugal
2.2 Perirenal space
(located between the anterior and the posterior renal fascia)
- contains -
Kidney
Adrenal gland
Proximal ureter
Renal artery and vein
The perirenal space is surrounded by the perirenal fascia which is incomplete where the renal vessels pass through it; it is thought that there are well-structured pores within the perirenal fat.
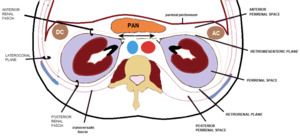
Fig. 21: Representation of the retroperitoneal cavity - perirenal space (purple).
References: Hospital de Braga, Portugal
The retrorenal plane represents an expandable plane located between the perirenal space and posterior pararenal space.
The retromesenteric plane is a potentially expansile plane located between the anterior pararenal space and the perirenal space.
The retrorenal and retromesenteric planes have merged to form a combined plane,
which is situated on the anterolateral surface of the psoas muscle,
lateral to the ureter and medial to the iliac vessels; it allows the spread into the pelvic extraperitoneum.
The retromesenteric plane allows communication across the midline.
2.3 Posterior pararenal space
(The posterior pararenal space is bound by the transversalis fascia posteriorly and the posterior renal fascia.
Anteriorly these space continues as the properitoneal fat line of the flank wall)
- contains -
Fat
lymph nodes
This space contains no viscera and rarely participate in pathologic processes.
Collections in the posterior pararenal space usually result from spontaneous retroperitoneal hemorrhage or from a disease in contiguous musculoskeletal structures.

Fig. 22: Representation of the retroperitoneal cavity - posterior pararenal space (pink).
References: Hospital de Braga, Portugal
2.4 A fourth space surrounds the aorta and inferior vena cava,
which is limited laterally by the perirenal spaces and ureters and extends superiorly into the posterior mediastinum.
Retroperitoneal fibrosis is an example of a disease that affects predominantly this space.
2.5
2.5.1 Paravesical space
(extraperitoneal space)
anterior and lateral to the umbilicovesical fascia
extends posteriorly to communicate with the presacral space
- contains -
Fat
2.5.2.
Prevesical space
(retropubic space or space of Retzius)
(extraperitoneal space)
bounded by umbilicovesical fascia
- contains -
Fat
bladder
urachus
obliterated umbilical arteries

Fig. 23: Typical “molar tooth” configuration of a prevesical fluid collection (red asterisk).
References: Hospital de Braga, Portugal