Type:
Educational Exhibit
Keywords:
Image verification, Education and training, Cerebrospinal fluid, Imaging sequences, Education, Diagnostic procedure, CT, CT-High Resolution, MR, Neuroradiology brain, Eyes, CNS
Authors:
M. Marinkic, G. Varga, L. Ljubešić; Zagreb/HR
DOI:
10.1594/ecr2018/C-3097
Findings and procedure details
Brain MR (magnetic resonance) is considered to be the best imaging tool in IIH.
When MR is not available,
a contrast-enhanced CT (computer tomography) scan should be sought.
The preferred imaging is brain MR with T2 coronal images and fat-sat (FS) images of orbit accompanied by MRV (magnetic resonance venography).
It is very important to understand the main roles of neuroimaging:
- to exclude other pathologies causing intracranial hypertension
- if possible,
to detect findings associated with IIH.
The cause of raised ICP in IIH is unknown and,
in contrast to cases where the role of radiologist is to find specific radiologic signs to confirm the proposed diagnosis,
in this case the main radiologic task is to exclude other causes of raised ICP.
The causes for secondary raised intracranial pressure (secondary pseudotumor syndrome) that mustn’t be overlooked on neuroimaging scans are dural venous sinus thrombosis and space-occupying lesions (Table.2).
Recognition of a secondary cause of raised ICP like venous sinus thrombosis or the diagnosis of IIH has crucial therapeutic and prognostic implications.
The differentiation of central venous thrombosis and IIH may be difficult even on venographic studies.
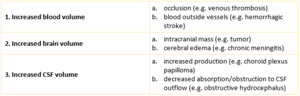

Table 2
Brain MR scan showing no abnormalities is a frequent finding in IIH.
However,
subtle radiologic findings suggestive of IIH have emerged with modern neuroimaging and the radiologist should know them thoroughly in order to perform an accurate reading of the scans.
The possible MR findings in IIH are:
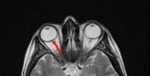
- posterior globe flattening (Fig.1)
- intraocular protrusion of the optic nerve head (Fig.2)
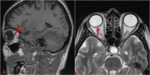
- optic nerve sheath enlargement (Fig.3)
- vertical optic nerve tortuosity (Fig.3)
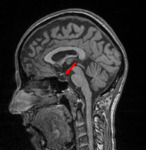
- empty or partially empty sella (Fig.4)
- enhancement (with gadolinium) of the prelaminar optic nerve
- venous sinus stenosis
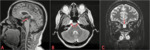
- enlarged Meckel cave (Fig.5)
- meningoceles,
typically within the temporal bone and sphenoid wing (Fig.5)
- slit-like ventricles (uncommon finding)
These findings are not diagnostic of IIH,
and their presence is not obligatory for the diagnosis of definite IIH.
Their discovery on brain imaging should not prompt invasive procedures,
unless clinical signs of IIH,
such as papilledema,
are present.