We retrospectively reviewed our radiologic archives and literature to illustrate the radiological features of myositis ossificans,
helping distinguish it from more aggressive pathological processes,
such as parosteal osteosarcoma and synovial sarcoma according to different imaging techniques.
CT/Plain radiograph
MYOSITIS OSSIFICANS
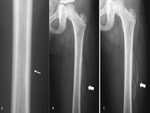
Myositis ossificans at plain radiographs in the first 2 weeks is typically normal, occasionally only with the evidence of periosteal reaction,
possibly because of associated subperiosteal hematoma; soft-tissue calcifications begin to become apparent radiographically at approximately 3 to 4 weeks.
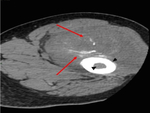
In the early phase the calcifications may appear as amorphous and flocculent and may simulate osteoid matrix and can have an appearance similar to that of extraskeletal osteosarcoma,
which also may be juxtacortical in location ( Fig. 1 ).
In the initial stages of myositis ossificans,
CT demonstrates soft-tissue swelling or a low-attenuation soft-tissue mass without associated calcifications.
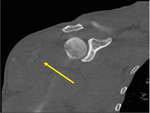
Typically the peripheral rim becomes increasingly calcified as it matures (Fig. 2).
The central noncalcified zone is typically isodense to adjacent muscle.However,
if the peripheral zonal pattern is not evident,
it may be difficult to diagnose myositis ossificans,
necessitating additional imaging evaluation or follow-up.
The calcifications typically mature during the next several weeks becoming more peripherally oriented and coarse in appearance,
around 6 to 8 weeks.
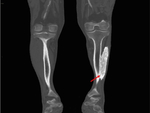
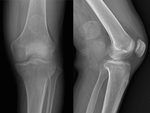
Mature lesions typically run in parallel with the long axis of the muscle and are sometimes adherent to the adjacent bone,
and differentiation from parosteal osteosarcoma may thus require CT or MRI,
for example to identify the cleft between the mass and adjacent bone.
( Fig. 3 )
PAROSTEAL OSTEOSARCOMA
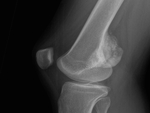
The radiographic aspect of parosteal osteosarcoma is of a large lobulated exophytic,
'cauliflower-like' mass with central dense ossification adjacent to the bone. In the first stage a thin radiolucent line,
corresponding histologically to the periosteum interposed between the cortex and the tumor mass,
separates the tumour from cortex ; as the tumour grows,
this cleavage plane will be gradually obliterated.
As it is generally a low-grade tumour,
there is a reactive cortical thickening of the ajacent bone without an aggressive periosteal reaction.
The tumour extension into medullary cavity is frequently seen ( Fig. 4 ).
At CT scan,
radiographic features of paraosteal osteosarcoma become more evident,
allowing the identification of parosteal origin of calcifications,
the soft-tissue involvement and,
mostly important,
the non aggressive behaviour of the lesion ( Fig. 5 ).
SYNOVIAL SARCOMA
Synovial sarcomas detected at radiography typically appear as nonspecific,
round to oval juxtaarticular soft-tissue masses. Calcification is identified in up to 30% of synovial sarcomas at radiography.
These calcifications are often eccentric or peripheral within the soft-tissue mass and nonspecific in appearance ( Fig. 6 ).
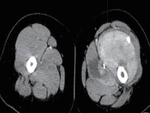
The most common CT appearance of synovial sarcoma is that of a heterogeneous deep-seated soft-tissue mass with attenuation similar to or slightly lower than that of muscle. Areas of lower attenuation representing necrosis or hemorrhage are also common although smaller lesions may be more homogeneous.
CT scans obtained after administration of intravenous contrast material show heterogeneous enhancement in 89%–100% of cases. This feature is quite helpful for distinguishing those synovial sarcomas that initially appear as a cystic lesion or hematoma on precontrast images,
as the heterogeneous enhancement pattern excludes these diagnoses ( Fig. 7 ).
MRI
MYOSITIS OSSIFICANS
MRI is the best single modality for imaging soft-tissue masses but it should be evaluated in conjunction with radiographs because calcifications may not be well demonstrated on MRI.
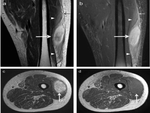
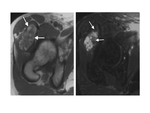
In the acute phase myositis demonstrates a heterogeneous signal intensity on T1-weighted images,
with areas of high signal intensity that are representative of blood products.
T2-weighted hyperintensity suggests regions of granulation tissue,
blood products,
and edema while T2-weighted hypointensity may correspond to hemosiderin deposition or calcifications ( Fig. 8 ).
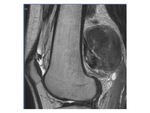
The MRI appearance that follows the acute phase classically demonstrates a lesion that is isointense to slightly hypointense to skeletal muscle on T1-weighted sequences.
Fluidweighted sequences will appear hyperintense to surrounding muscle.
At this stage,
surrounding edema may or may not be present. As lesions progress,
a pattern of mature,
lamellar bone becomes better defined and demonstrates low signal intensity on all sequences,
and the surrounding edema has resolved.
Mature lesions may have areas of internal fat,
which correspond to marrow production in the heterotopic bone ( Fig. 9 )
PAROSTEAL OSTEOSARCOMA
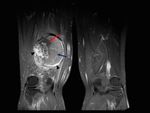
On MRI,
parosteal osteosarcomas are hypointense on both T1- and T2- weighted images due to their dense osteoid components ( Fig. 10 ).
High signal intensity on T2-weighted images could indicate a high grade component,
especially associated with irregularity on cortex and high signal intensity of the marrow ( Fig. 11 ).
SYNOVIAL SARCOMA
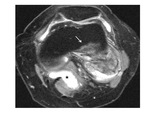
On MR images,
synovial sarcoma typically appears as a prominently heterogeneous multilobulated soft tissue mass with signal intensity similar to or slightly higher than that of muscle on T1-weighted images.
Prominent heterogeneity with predominant high signal intensity is also a feature of these lesions on T2-weighted MR images.
This signal heterogeneity has been described as the triple sign,
represented by intermixed areas of low,
intermediate,
and high signal intensity on long repetition time images ( Fig. 12 ).