Patient Selection:
This is a single-center prospective study.
A total of 16 consecutive patients diagnosed with moderate-to-severe lower urinary tract symptoms (LUTS) secondary to benign prostatic hyperplasia (BPH) were included in the study.
All of the participants were high-risk surgical patients,
did not respond to medical treatment and all but one had an indwelling bladder catheter.
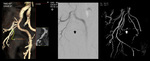
Preprocedural imaging:
All patients underwent pelvic CT angiography before PAE.
The tests were performed with a 64-detector row CT (Aquilion,
Toshiba) or a 8-detector row CT (Brightspeed,
GE Medical Systems).
CT angiography protocol entailed the administration of 120mL of non-ionic iodinated contrast material (Vispaque,
320mg/ml iodine) at a rate of 4-5ml/s through a peripheral vein.
Postprocessing was performed at the workstation (Vitrea,
Vital Images or Advanced Workstation,
GE HEalthcare) obtaining maximun intensitiy projections (MIP) and volume rendering images,
showing the optimal obliquity of the prostatic arteries (PA).
Patient evaluation:
Patients were evaluated at least once before the procedure and between 6 and 12 months after intervention.
Patient clinical evaluation included IPSS (International Prostate Symptom Score) and Quality of Life Questionnaire (QoL),
physical examination,
laboratory tests,
uroflowmetry,
and transrectal ultrasonography (TRUS).
Prostate volumes were measured with transrectal ultrasound,
using the ellipsoid method formula,
before and after the procedure.
Clinical success was defined by removal of the IBC and at least 7 point improvement of the IPP score after PAE.
Data analysis:
Statistical analysis was performed using SPSS version 23 statistical software package (IBM).
Continuous variables were tested for normality and equality of variances with Kolmogorov-Smirnov’s test and the Levene’s Test,
respectively.
For comparisons of baseline and outcome variables the paired t test and Fisher’s exact test was used.
Statistically significant differences were assumed at p<0.05.
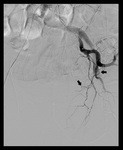
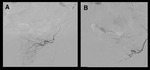
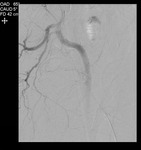
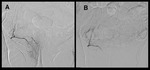
PAE technique:
Catheter angiography was performed under local anesthesia through a percutaneous right femoral artery access.
Angiography of the anterior division of the internal iliac arteries was performed in ipsilateral anterior oblique projection,
using the optimal obliquity determined in the CT angiography.
Selective catheterization of the prostatic artery was then performed.
Embolization was done with 100-300μm (and a combination with 300-500μm in some cases) polyvynil-alcohol based microspheres (Bead Bloc; BTG) until all the arterial branches that supply the prostate were completely occluded.
Technical success was defined by the embolization of all the angiographically visible arterial supply to the prostate.