Keywords:
Obstruction / Occlusion, Embolism / Thrombosis, Embolisation, CT-Angiography, Cone beam CT, Catheter arteriography, Pelvis, Interventional vascular, Genital / Reproductive system male
Authors:
J. Vega, J. Cobos, M. Morales Garcia, J. M. Vicente Martín, E. Meilán Hernández, J. Angulo Cuesta; Getafe/ES
DOI:
10.1594/ecr2018/C-3149
Results
The 16 patients met the inclusion criteria.
The mean age was 79.37± 4.88 years.
All patients were high-risk surgical candidates: five of them suffered from ischemic cardiomyopathy,
two suffered from Alzheimer’s disease,
one from Parkinson’s disease and six had chronic obstructive pulmonary disease.
Five patients had refused blood transfusion based on religious beliefs and four were treated with oral anticoagulants.
The procedure was technically successful in 13 patients.
PAE was stopped in one patient due to an episode of agitation and only unilateral embolization was performed.
In the other two patients unilateral embolization was achieved,
but due to severe atherosclerosis selective catheterization of the contralateral prostatic artery was not feasible.
One of these patients showed an early clinical improvement after unilateral embolization so contralateral PAE was not performed.
PAE was successfully repeated in the contralateral side in the other patient one month after the first procedure.
Clinical success (defined as a seven-point improvement in IPSS and removal of the indwelling bladder catheter (IBC) at the follow-up evaluation) was achieved in 15 patients.
Bladder catheters were removed between 10 and 60 days after the procedure.
Only one patient remained on urinary retention with IBC,
despite successful bilateral embolization and mild prostatic volume reduction.
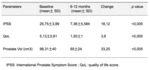
We compared the baseline clinical parameters with those recorded at follow-up evaluation and found a statistically significant improvement in IPSS (mean reduction 18± 6.8,
p<0.005),
Quality of Life Questionnaire score (mean difference 3.5 points± 1.4,
p<0.005) and prostate volume (mean reduction 33.20 ml ± 25.7,
p<0.005).
There was only one important procedure-related complication.
One patient complained of a small wound on the glans penis seven days after the procedure,
with necrotic tissue appearing a few days later.
Conservative management with antibiotics was decided and the wound had completely healed two weeks later.
This patient had undergone a successful bilateral prostatic artery embolization.
However the prostate volume was the greatest in our cohort (166cm3) and the penis wound was probably a consequence of non-target embolization as a result of reflux of microspheres with distal migration and occlusion of small arteries in the penis.
Preprocedural CT angiography role in the evaluation of the of the iliac artery and its branches is very important: knowledge of the anatomy of the pelvis arteries can be useful for avoiding complications such as non-target embolization of surrounding organs.
Evaluation of the atherosclerotic changes in this region can help in selecting suitable candidates for PAE and planning the procedure.
Volume render images were used to find the optimal obliquity for visualizing the origin of the prostatic artery.
Even though our study did not focus on radiation doses or fluoroscopy time,
we found a significant reduction in the procedure duration when we used the obliquities at which those volume rendering images were obtained as guidance during PA catheterization.