DIAGNOSIS
In the next image,
you will find the advantages and diasadvantages of the different imaging modalities in acute ischemic stroke.
Fig 1
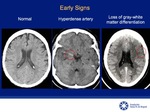
EARLY FINDINGS OF ACUTE ISCHEMIC STROKE
CT Head without contrast (w/o C)
It allows to classify the CVA in hemorrhagic or ischemic.
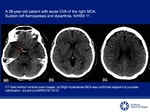
EARLY SIGNS OF ISCHEMIA CVA IN CT HEAD WITHOUT CONTRAST ARE:
Loss of gray-white matter differentiation.
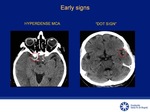
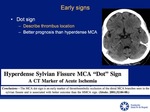
Hyperdense artery (Hyperdense MCA and "Dot" sign) [4,5,8].
Fig 2-4
Important tips
The sign is often present after 90 minutes
30% sensibility
+/- 100% specificity
False (+) includes high hematocrit level,
arterioesclerosis (bilateral)
Hounsfield unit ratio 1,2:1 contralateral or > 43 HU.
Measure of the length (over 8 mm least likely to reperfuse with thrombolysis).
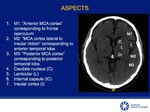
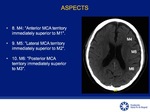
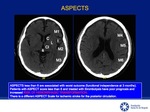
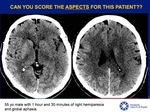
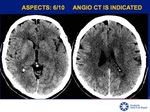
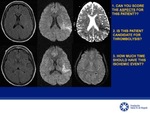
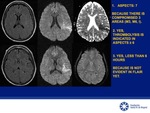
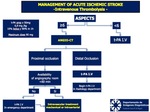
ALBERTA STROKE PROGRAMME EARLY CT SCORE (ASPECTS)
Quantitative score scale of 10 cerebral areas used in patients with ischemic stroke for evaluation of the territory of the middle cerebral artery (MCA) [6].
80% of the acute strokes are in this territory.
Each patient begins with 10 points and for each area of gray-white matter loss of differentiation 1 point is substracted.
Example: If there are 3 territories involved,
the final score on the scale will be 7.
The 10 ASPECTS regions are evaluated in 2 axial sections of the head CT Fig 5-7:
Ganglionic level: (M1 to M3,
caudate nucleus (C),
Lenticular nucleus (L),
internal capsule (IC) and Insular cortex (I).
Supraganglionic level: (M4 to M6 - anterior,
middle and posterior cortex).
The level and a window width of approximately 35-45 HU should be used to evaluate the gray and white matter differentiation.
Using quantitative hemodynamic maps,
it is possible to obtain information of the transit of contrast medium from the arteries to the capillaries to the veins within the brain.
We use perfusion CT mostly in patients with symptoms for more than 6 hours and less than 24 hours to evaluate the penumbra.
[7]
THE PARAMETERS USED TO EVALUATE THE CEREBRAL PERFUSION ARE:
MTT: MEAN TRANSIT TIME
CBF: CEREBRAL BLOOD FLOW
CBV: CEREBRAL BLOOD VOLUME
CORE:
Brain tissue with CBF <10 ml/100gr/min.
Irreversible ischemic tissue.
PENUMBRA:
Brain tissue with CBF <20ml/100gr/min.
Presents decreased neuronal activity.
BENIGN OLIGOHEMIA:
Brain tissue with CBF <50ml/100gr/min.
There is no risk of irreversible ischemia.
Slightly hypoperfused brain tissue.
Allows for the evaluation of the vascular anatomy.
Technical issues are important:
- Antecubital vein with at least 18 g
- 50 to 75 ml of contrast commonly used
- First run should include from the aortic arch to the vertex
- Three phases are obtained,
early arterial,
late arterial and venous phase for the evaluation of collaterals,
with a time delay of 8 seconds between phases.
[9]
It is important for the planning of the endovascular procedure - selection of catheters for carotid and vertebral arteries catetherization.
Critical Findings:
-Rule out aortic arch anatomical variations.
Fig.
8
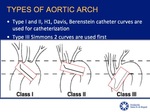
- type of aortic arch: type I and II (H1,
Davis and Berenstein curves) and type III Simmons 2 catether curves should be used.
Fig.
9
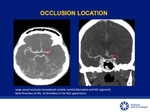
- evaluate carotid bifurcation and vertebral artery origin.
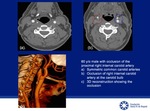
- determine occlusion site.
Fig.
10-11
- Determine thrombus extension.
- Document possible causes of arterial occlusion (cardiac or large vessel embolism,
dissection,
intracranial stenosis,
etc...).
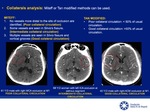
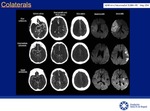
- Evaluate collateral circulation which are useful for the penumbra and final infarct volume evaluation and patient outcome.
Many classifications are available,
choose one and attach to it.
[10] Fig.
12-13
It is an excellent diagnostic modality for ischemic stroke.
Fig.
14
The stroke protocol sequences include diffusion,
SWI and T2 FLAIR,
each one with particular objective:
DWI: To determine the presence and extent of the infarct core,
better than CT.
Core infarcts greater than 72 ml have worst outcome.
Our threshold for contraindication of thrombectomy are 100 ml for anterior circulation.
SWI: To rule out intraaxial or subarachnoid hemorrhage,
hemorrhagic transformation of the infarcted tissue and exact thrombus location and extent.
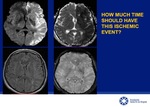
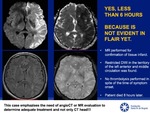
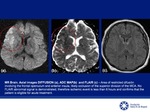
T2 FLAIR: If areas of restricted diffusion are seen in FLAIR,
the time of ischemia is likely greater than 4,5 hours with contraindication for IV thrombolysis.
Perfusion is used mostly after 6 hours otherwise we do clinical,
occlusion site and DWI mismatch.
[11]
The mismatch between DWI and perfusion that we use for penumbra significant tissue is a difference of 20%,
however it has been shown that an infarct with a volume greater than 70 ml in DWI is a better predictor of mRs <2 at 90 days.
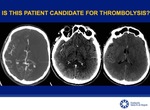
CASE 1.
Fig.
15 - 21
CASE 2.
Fig.
22-23
TREATMENT
CURRENT ACUTE TREATMENT IS:
Intravenous thrombolysis with rt-PA up to 4.5 hours.
Intraarterial mechanical thrombectomy is commonly performed up to 6 hours of symptoms onset to arterial puncture,
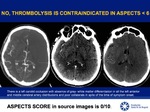
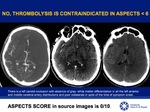
with ASPECTS >5,
in patients older than 18 years,
NIHSS > 6,
in patientes with anterior circulation large vessel occlusion,
posterior circulation stroke,
no response to intravenous thrombolysis or with contraindications for intravenous thrombolysis.
[12]
Patients must be evaluated quickly,
CT or MR should be done in less than 25 minutes after triage evaluation!!! The report to stroke code team should be in less than 45 minutes and IV TPA administered in less than 60 minutes in more than 80% of the patients.
Fig 24.
If there is a recanalization before 150 minutes,
the probability of independence is 91%.
The next hour of delay reduces this probability of functional independece at 90 days in 10% and then decreases this possibility decreases 20% per each hour.
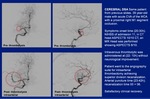
CEREBRAL ANGIOGRAPHY
Modality to perform intraarterial thrombectomy procedure.
Diagnostic initial angiography confirms the site of occlusion and if there is no recanalization after intravenous thrombolysis.
Thrombus aspiration is initially performed and if there is no recanalization stent retrievers are used.
The reperfusion is evaluated with the mTICI score.
Times from triage and imaging to arterial puncture,
first recanalization time and best recanalization times are measured.
CASE 3.
Fig 25-27
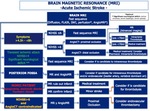
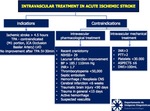
ALGORITHMS AND THROMBOLYSIS CONTRAINDICATIONS Fig.
28-31