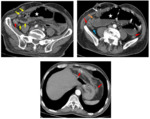
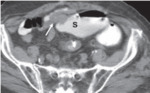
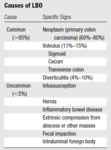
Radiology assumed considerable relevance in assisting the therapeutic decision of surgeonS by addressing these questions:
Is the bowel obstructed?
Obstruction is present when distended bowel loops (diameter >2.5 cm for small bowel (SB) loops and >6 cm for large bowel (LB),
from outer wall to outer wall) are seen proximal to normal-caliber or collapsed loops distally.
What is the severity?
In high-grade obstruction,
there is a 50% difference in caliber between the proximal dilated and the distal collapsed bowel.
Also,
obstruction that has been present for several days leads to complete evacuation of the bowel segments distal to the obstruction point,
highlighting the discrepancy in caliber between the proximal and distal bowel loops.
The “SB feces” sign is a reliable indicator of small bowel obstruction (SBO) but cannot be used for assessing the severity of obstruction: it only identifies the transition point.
It is present when gas bubbles mixed with particulate matter are observed in dilated SB loops proximal to an obstruction.
What is the level?
For SBO,
the approach should begin in a retrograde fashion by starting at the rectum and proceeding proximally toward the cecum,
ileum,
and jejunum.
If the transition point is located proximally (jejunum or duodenum),
the position should be confirmed by using an antegrade approach,
starting at the stomach.
For large bowel obstruction (LBO),
it is more easy to identify the transition zone in retrograde fashion,
following the course of the distal colon proximally until the dilated loops are encountered.
- Spasm at the splenic flexure in a normal colon may mimic a fixed narrowing.
- Dilatation of the ascending and transverse colon with the transitional region near the splenic flexure,
and distal collapse can be seen in both Acute Colonic Pseudo Obstruction (ACPO) and chronic colonic pseudo obstruction.
- “Colon cut-off” sign,
an isolated gaseous distension of the ascending colon and hepatic flexure in the setting of pancreatitis,
can also mimic an LBO.
- When distension of the entire SB is observed without colonic collapse,
the most probable diagnosis is an adynamic ileus,
and a contrast material enema is recommended to rule out colonic obstruction.
What is the cause? Fig. 15 Fig. 16
The answer is almost always in the transition point:
- Extrinsic causes are seen adjacent to the transition point and usually have associated extraintestinal manifestations.
- Intrinsic bowel lesions are seen at the transition point and manifest as localized mural thickening.
- Intraluminal causes manifest as endoluminal “foreign objects” with imaging characteristics different from those of the remaining enteric content.
In our study,
causes were correctly predicted by radiologists in 58 of 80 cases and included obturator hernias,
followed by adhesions,
primary tumors,
volvulus,
intussusceptions,
peritoneal carcinomatosis,
bezoars,
pelvic cancers with intestinal involvement,
Crohn disease,
dysfunction of colostomy and incisional strangulated hernias.
Mean length of stay hospital was 6 days.
Four patients died after surgery.
EXTRINSIC CAUSES
Hernias
- LB hernias
LBO can occur less frequently than SBO,
secondary to inguinal,
femoral,
umbilical,
Spigelian,
incisional,
lumbar,
and diaphragmatic hernias.
The most common internal hernia to produce an LBO is the foramen of Winslow hernia.
On CT,
colon will be found in a hernia with dilated proximal colon and decompressed distal colon.
2. SB hernias
External hernias occur at inguinal (the most common),
femoral,
and umbilical locations.
Internal hernias are less common.
The left-sided paraduodenal hernia is the most commonly reported internal hernia.
Diagnosis of external hernias in most cases is obvious on clinical examination whereas internal hernias diagnosis is almost always radiological.
CT is useful in depicting the site,
the type of hernia,
the size of the hernia defect,
demonstrating the hernial anatomy,
its contents and adverse features.
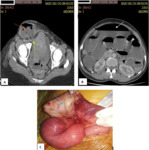
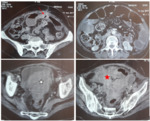
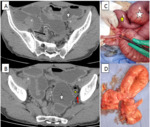
In cases of strangulated hernia,
compromise of the blood supply results in thickening of bowel loops.
Adjacent inflammatory changes can be associated Fig. 1.
Adhesions
80% of adhesions occur after surgery,
15% are due to inflammation,
and the remaining few are due to congenital or unexplained causes.
It is a very rare cause of LBO.
It have been reported in the right,
transverse,
and sigmoid colon.
However,
it is the main cause of SBO.
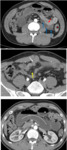
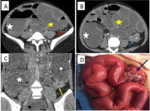
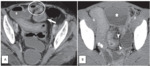
The diagnosis is primarily one of exclusion because adhesive bands are not seen at CT; only an abrupt change in the caliber of the bowel is seen without any associated mass lesion,
significant inflammation,
or bowel wall thickening at the transition point Fig. 2 Fig. 3 .
A volvulus may also demonstrate a transition point without any associated cause; however,
the clinical history,
anatomical location and associated twisting of mesenteric vessels around the transition point can help to distinguish between a volvulus and adhesion Fig. 5 .
Occasionally an associated operative scar on the under surface of the abdominal wall may be seen with adhesive bands.
Extrinsic masses
1. LBO
Caused by adjacent masses such as endometriosis,
lymphadenopathy,
pancreatitis,
intra-abdominal abscesses,
mesenteric or colonic surface involvement of peritoneal carcinomatosis,
and direct invasion from gynecologic or prostatic malignancies.
The CT findings include LB dilatation from a soft-tissue mass.
2. SBO
Carcinoid tumors: seen as nodular calcified masses with surrounding retraction of mesentery and thickening of surrounding bowel loops.
Peritoneal carcinomatosis: SB involvement by metastatic cancer is more frequent in the form of peritoneal carcinomatosis,
which is suggested on CT when extrinsic (omental or serosal) mass is involving the SB wall in the transition zone causing obstruction,
otherwise,
adhesions may need to be considered as a possible cause Fig. 11 .
Ovarian carcinoma is the most frequent cause of metastatic disease of the omentum.
Other tumors that frequently spread to the omentum include carcinoma of the colon,
stomach,
pancreas,
breast,
and endometrium.
Infection due to appendicitis or diverticulitis: obstruction is usually due to a segment of SB becoming involved with an adjacent phlegmon,
abscess,
or inflammatory process.
Lymphoma
INTRINSIC CAUSES
Tumors
1. LB tumors
Usually developed on the sigmoid colon or the splenic flexure.
Left-sided malignancies cause diffuse distension of the colon proximal to obstruction.
Right-sided tumors with an incompetent ileocecal valve can mimic SBO.
The most common site of perforation in LBO is not at the site of the tumor but at the cecum.
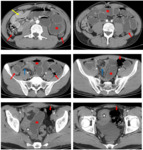
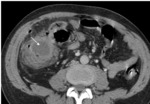
CT show asymmetric and short-segment (<10cm) colonic wall thickening or an enhancing soft-tissue mass centered in the colon that narrows the colonic lumen with or without findings of ischemia and perforation Fig. 4.
Obstructing colon cancers often produce a shouldering appearance and may be large enough to have central necrosis or rarely air within the mass,
the latter appearance may resemble an abscess Fig. 12 .
Also,
the presence of lymph nodes raise the suggestion of a colonic malignancy. Recognition of proximal colonic dilatation aids in identification of the transition point at the site of tumor.
Colonic malignancy may mimic diverticulitis if there is infiltration of the pericolonic fat.
Diverticulitis is usually located on the sigmoid and is characterized by segmental, symmetric bowel wall thickening with hyperemia,
which is typically in a long segment (>10 cm).
Pericolonic inflammation and fat stranding are hallmarks of diverticulitis.
If the inflammation is extreme,
intramural and extramural abscesses,
as well as perforation with pneumoperitoneum,
may be seen.
Fluid in the root of the mesentery and vascular engorgement favor the diagnosis of diverticulitis.
2. SB tumors
Primary SB tumors are rare.
When a SB adenocarcinoma manifests as SBO,
it is usually at an advanced state.
It usually appears as a jejunal or duodenal mass-like thickening,
shouldering,
nodular or ulcerating mass with proximal obstructive features.
CT shows tumor extension and local or distant metastases.
SBO caused by isolated metastases to the bowel are extremely rare and poses a significant diagnostic challenge.
Crohn disease or ulcerative colitis
CT findings include wall thickening,
luminal narrowing secondary to the transmural inflammatory process leading to prestenotic dilatation,
fatty infiltration of the mesentery and dilatation of the vasa recta supplying the affected bowel loop Fig. 8 .
During the acute,
inflammatory and noncicatrizing phase of Crohn disease,
bowel shows mural stratification with a targetlike or “double halo” appearance.
Inflamed mucosa and serosa may markedly enhance on postcontrast CT and the intensity of enhancement correlates with the clinical activity of the disease.
During the chronic fibrotic stenosis phase,
mural stratification disappears and the affected bowel wall has homogeneous attenuation.
In addition,
fat deposition in the bowel wall indicates inactive disease.
Distinguishing between these conditions is essential for treatment Fig. 13 .
Lymphadenopathy,
ascites,
abscesses,
and fistulae arising from diseased segments may also be present.
It is also important to exclude malignancy in individuals with Crohn disease as their risk of colon cancer is two to three times higher compared with standard populations.
Stricture formation and obstruction is less common in ulcerative colitis and should raise suspicion of an underlying malignancy.
Tuberculosis
Is the commonest infection to cause SBO.
The most commonly affected site is the ileocaecal region.
When inflammation is mild,
CT demonstrates only slight,
symmetric mural thickening and a few small adjacent mesenteric nodes Fig. 9 .
In advanced and severe cases, we may note marked thickening of the bowel wall,
and the inflammatory mass may have a heterogeneous appearance.
Large regional nodes with hypoattenuating centers are present,
findings that are consistent with caseating necrosis.
Ascites with thickening and enhancement of the peritoneum may also be present.
Benign peritoneal disease such as chronic tuberculous peritonitis can cause retraction and fibrosis of the mesentery leading to mechanical obstruction of the SB.
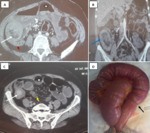
Intussusceptions
Bowel has appearance of a “target” in cross-section or sausage-shaped mass if in the longitudinal plane,
with alternating layers of low and high attenuation.
Also,
the bowel-within-bowel configuration is composed by collapsed,
intussuscepted proximal bowel (intussusceptum) with or without mesenteric fat and vessels lying within the thickened wall of the distended distal bowel (intussuscipiens) Fig. 6 .
A leading mass as the cause of the intussusception can be identified,
but this finding should be carefully interpreted and differentiated from the soft-tissue pseudotumor that represents the intussusception itself.
Colon carcinoma is the most common cause of a colocolonic intussusception,
in addition to benign lesions like adenomatous polyps,
lipomas,
gastrointestinal stromal tumors and appendiceal lesions including the inverted appendiceal stump,
endometriosis involving the appendix,
mucocele.
SB intussusception may be caused by various extrinsic (adhesions,
duplications),
intrinsic (benign or malignant polypoid tumors),
or intraluminal (foreign bodies).
Transient intussusceptions are not associated with this condition and may occur in patients with coeliac disease.
INTRALUMINAL CAUSES
It include gallstones,
foreign bodies,
meconium,
tangles of ascarides or bezoars (intraluminal mass with an ovoid shape,
usually in the jejunum or proximal ileum).
Fluid in the SB outlines the mass located in the transition zone.
It has a mottled appearance owing to air retained in the interstices.
This appearance may be similar to the "feces sign".
MALPOSITIONS
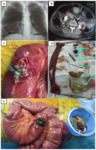
Volvulus
1. LB
It is a twisting of the intestine (usually the sigmoid,
rarely the cecum,
transverse and splenic flexure) upon itself that causes obstruction.
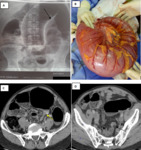
CT findings include single transition point and disproportionate proximal enlargement of the sigmoid.
The coffee bean,
kidney bean,
and bent inner tube signs,
all descriptors of the appearance of air-filled closed loop of colon,
can all be seen.
A “beak” can be found at the point of twisting of the sigmoid colon and if necessary,
may be confirmed with colonic contrast material.
The whirl sign,
the appearance of spiraled loops of collapsed bowel with enhancing engorged vessels radiating from the twisted bowel,
is often evident at the point of obstruction Fig. 5.
2. SB
Is rare and may occur secondary to various conditions such as malrotation,
congenital bands,
postoperative adhesions,
and internal hernias.
CT findings include right-sided SB,
left-sided colon,
abnormal relationships between superior mesenteric vessels,
and aplasia of the uncinate process.
Distended and fluid-filled loops have U-shaped configuration or radial distribution,
converging toward the point of torsion,
and mesentery tightly wound around the point of torsion (whirl sign).
Is the obstruction complicated?
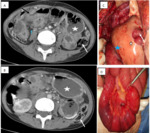
1. Closed-loop obstruction
A closed-loop obstruction (incarcerated) is a form of mechanical obstruction in which a segment of bowel is occluded at two points along its course by a single constrictive lesion occluding both bowel and mesentery.
The closed loop is able to rotate along its axis,
thereby producing a volvulus.
Most commonly this occurs due to an adhesive band or a hernia.
As adhesions and hernias are commoner in the small rather than LB,
closed-loop obstruction are seen more often with SBO.
CT findings depend on the length,
degree of distention,
and orientation of the closed loop in the abdomen.
When a closed SB loop (usually dilated and fluid-filled) is horizontally oriented,
it has a U- or C-shaped configuration at axial imaging.
A radial configuration with stretched mesenteric vessels converging toward the site of torsion may be detected depending on the orientation of different SB loops within the incarcerated bowel segment Fig. 3.
A “beak sign” is seen at the site of the torsion as a fusiform tapering,
and occasionally a “whirl sign” can be seen,
reflecting rotation of the bowel loops around the fixed point of obstruction Fig. 3 .
2. Strangulation
Is most commonly associated with adhesions or herniated bowel.
It is defined as a closed-loop obstruction associated with intestinal ischemia. If present, emergent surgical decompression is advised to avoid transmural necrosis and perforation.
Findings indicative include:
- High-density bowel wall sign on precontrast CT image.(hemorrhagic congestion) usually accompanied by bowel wall thickening (>3 mm).
- Reduced (or delayed enhancement) in the early phase,
or lack of wall enhancement in the late phase.
A pitfall: when strangulated bowel wall show high density on precontrast CT because of hemorrhage,
postcontrast CT will show this high-density bowel wall to seem to be enhanced,
unless precontrast CT is performed.
Therefore,
precontrast CT is essential to compare the degree of enhancement of the bowel wall between pre and postcontrast scans.
- Focal or diffuse increased attenuation of the mesenteric fat because of edema (congestion) or hemorrhage in the mesentery attached to the closed loop.
- Closed-loop mechanism defined by at least two adjacent abrupt transition zones of bowel and/or C- or U-shaped configuration of the bowel loop and the mesenteric vessels converging toward torsion.
- “Target sign” (submucosal layer edema) on loops located upstream of the transition zone.
- Whirl sign: a soft-tissue mass with an internal architecture of swirling mesenteric vessels and fat attenuation reflecting a twist in the mesentery.
- Ascites may be present also in patients with closed-loop obstruction without ischemia or with simple BO.
- In advanced cases: pneumatosis intestinalis (intramural gas),
mesenteric venous gas,
and/or portal venous gas: not specific for strangulation,
rather for inbowel infarct
A combination of the three first signs is sufficient to predict strangulation in adhesive SBO and suggest surgery.
Another difficulty is to differentiate primary strangulated loops from secondary proximal dilated loops.
The main point for differentiation is that strangulated loops are usually filled mostly with intestinal fluid,
and that secondary dilated bowel loops are filled with the admixture of air and fluid.