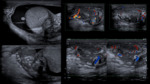
The fundamental causes of acute scrotal syndrome can be divided into the following groups:
VASCULAR:
Torsion of spermatic cord.
Torsion of testicular appendices.
Testicular infarction.
Thrombophlebitis sperm vein.
INFECTIOUS:
Orchitis Epididymitis Gangrena de Fournier.
TRAUMATICS:
Scrotal trauma
SYSTEMIC AND DERMATOLOGICAL
Schonlein-Henoch purple.
Idiopathic scrotal edema.
Familial Mediterranean fever.
Medicated dermatitis.
Erythema multiforme.
Contact eczema.
PATHOLOGY OF NEIGHBORHOOD
Inguinal hernia.
Hydrocele Meconial vaginalitis.
Varicocele Epididymal cyst and spermatocele.
MISCELLANY
Testicular tumors.
Epididymal and paratesticular tumors.
Scrotal fat necrosis.
Idiopathic scrotal necrosis.
Torsion.
More frequent in adolescents.
It is a true surgical emergency.
There are 2 types: extravaginal and intravaginal.
Intravaginal torsion,
more frequent in adolescents,
occurs when the tunica vaginalis completely envelops the testicle and the epididymis presenting an insertion that is too high and allowing the testicle to rotate freely in the hemiscrotum (in the bell clapper).
Extravaginal torsion is more rare and usually appears in neonates.
It is caused by a scarce or lack of insertion of the testicle to the wall of the scrotum,
allowing the testicle,
epididymis and vaginalis to rotate together.
In both cases the veins are blocked before the arteries causing testicular edema.
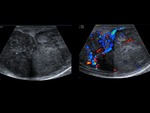
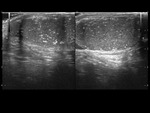
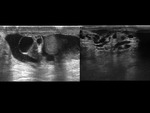
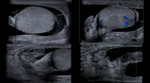
Grayscale findings are not typical and Doppler examination is mandatory.
The affected testicle shows a markedly diminished or absent flow with respect to the contralateral.
It is very important to use wall filters with low repetition frequencies due to the low velocities of the testicular vascular flow.
The diagnosis is difficult in cases of intermittent torsion since in the phase of distortion the flow can be normal or even increased.
However,
an infarct area can be observed as a sequel.
In case of chronic torsion there is no flow in the testicle but the paratesticular tissues may show an increased flow.
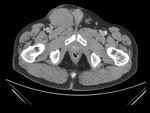
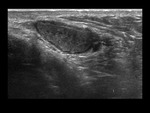
Trauma.
The consequences of trauma can be bruising,
fracture or rupture.
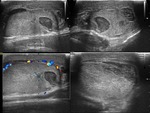
An irregular contour of the testicle can be observed,
bruises,
alterations in echogenicity due to hemorrhage or infarction,
thickening of the testicle or scrotal wall and rupture of the albuginea.
In case of testicular eruption,
the anatomical testicular architecture may not be recognized.
Doppler can differentiate testicular fragments from a complex hematoma and indicate potentially recoverable tissue.
The acute hematoma is echogenic.
In the subacute phase it appears as a collection of hypoechoic fluid with septa formation.
If the testicle appears diffusely hyper or hypoechogenic,
testicular rupture should be suspected.
Infection.
Orchiepididymitis is the most frequent cause of acute scrotal pain in adults.
The infection usually begins in the head or tail of the epididymis and extends from there to the entire epididymis and to the testicle,
diffusely or focally.
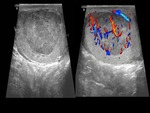
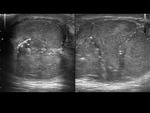
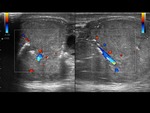
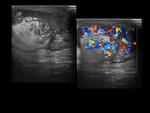
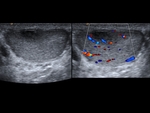
The echogenicity is heterogeneous,
with thickening of the scrotal covers and increased Doppler flow.
An enlarged and hyperechogenic testicle can be observed initially.
Later,
it may have hypoechoic areas due to edema,
and develop venous infarcts and hemorrhages,
reactive hydrocele or pyocele,
and sometimes progress to abscess.
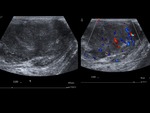
Tumors
Seminomas are the most frequent testicular tumors,
affecting young patients (30-40 years).
Cryptorchidism is a risk factor.
They usually present as homogeneous hypoechoic masses with an oval shape,
with sizes from a small nodule to occupy the entire testicle.
They may also present a more heterogeneous appearance with calcifications,
microlithiasis,
necrosis or increased flows in the Doppler study.
Among the non-seminomatous tumors are carcinomas of embryonic cells with a more aggressive behavior than seminomas and with frequent invasion of the albuginea,
testicular distortion and visceral metastasis.
They are more heterogeneous,
with poorly defined margins and frequent cystic areas of necrosis,
hemorrhage,
calcification or fibrosis.
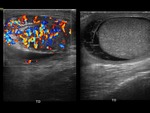
Other pathologies:
Varicocele: dilation of the pampiniform plexus veins greater than 1.5-2 mm.
Their visualization improves when they become more prominent after Valsalva maneuvers or in standing position
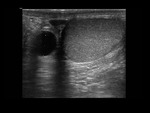
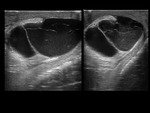
Hydrocele,
hematocele and pyocele: collections of serous fluid,
blood or pus respectively between the two sheets of the tunica vaginalis.
Cysts of epididymis or spermatoceles (more frequent in the head) with anechoic content or with debris by sperm,
lymphocytes,
fat.
Calcifications and microlithiasis,
in the testicle or in adjacent tissues.