1.
Breast cancer recurrence statistics and risk factors
Both radical surgery (mastectomy) and breast conserving surgery are used in breast cancer treatment.
Local recurrence can occur after both radical and breast conserving treatment.
Recurrence occurs in approximately 5% of patients at 5 years with a local failure rate of approximately 1%-2.5% per year. After 5 years,
the risk of recurrence then diminishes,
but patients remain at risk even 10 years after treatment.
[5] E.
Divjak et al.
[1] reported total recurrence rate of 3.85%,
similar to earlier studies. Studies show that breast cancer recurrence rates for patients who undergo these newer procedures(skin or nipple sparing mastectomy) are comparable to those for patients who undergo MRM,
at about 1%–2% per year [7,
8]. The local breast cancer recurrence rate for patients who undergo breast conservation therapy is similar,
at 1%–2.5% per year [3,
6].
Risk factors [10]
- Young age
- Premenopausal status
- Metastatic axillary lymph nodes
- Multifocality
- Lymphovascular invasion
- Absence of estrogen receptors
2.
Description of various surgical treatments of breast cancer
Modified radical mastectomy involves complete removal of the breast tissue,
skin envelope,
NAC,
and level I and II axillary lymph nodes.
[4] MRM is standard choice for locally advanced invasive and inflammatory breast cancer.
[4]
Skin-sparing mastectomy also involves complete removal of breast tissue,
but preserves skin and natural inframammary fold with/without nipple-areloar complex.
After skin-sparing mastectomy,
reconstruction surgery is followed.
[4]
Breast-conserving surgery,
or lumpectomy involves partial removal of breast tissue.
Patients with early-stage disease are usually eligible for either BCS or mastectomy.
Postoperative radiation therapy is required to eradicate any microscopic residual disease.
[14]
There are various methods of post-operative reconstruction methods,
including autologous tissue transfer (FLAPs),
autologous fat grafting,
and synthetic implants.
[4]
Autologous tissue transfer (FLAPs) have advantages including durability or naturalness over synthetic implants insertion.
Most commonly,
pedicled TRAM flap is used for breast reconstruction after mastectomy.
Contralateral rectus abdominis muscle will tunneled through the inflamammary fold to the mastectomy area.
Fig. 1 Pedicled LD flap is another widely used pedicled flap using ipsilateral latissimus dorsi muscle.
Fig. 2 Free flaps can be also considered to match the defect from mastectomy.
Free flap is autologous tissue-transfer methods by complete seperation of the donor tissue from its vascular supply.
Donor vessel will be typically attached to the internal mammary artery.
[4]
3.
Multimodality imaging of benign post-operative change such as hematoma,
seroma,
fat necrosis,
additional post radiation change.
Seroma is collection of fluid under the skin at the site of a surgical incision,
sometimes inflammatory.
Most seromas slowly diminish in size and evolve into scars by 1 year after surgery.
Fig. 3
- Mammography : a seroma manifests as a mass or increased density
- US : anechoic fluid collections. As maturation occurs,
thickened nodular margins may develop
- MR imaging : well-defined lesions of low or intermediate signal intensity relative to adjacent breast tissue on T1-weighted images and of high signal intensity (fluid signal) on T2-weighted images
- Smooth,
thin (≤5 mm) rim enhancement around a seroma should be considered benign
Hematoma results from preceding surgery,
biopsy (rare) and can be easily misinterpreted as other lesions such has breast malignancy if the correct clinical context is not taken into account. Aspiration is usually not needed.
- Mammography : single nodule,
diffusely increased glandular density (the most common appearance),
nodules with calcification
- US : variable - fluid collection,
solid nodule,
cystic nodule,
diffuse parenchymal abnormalities,
calcified nodule
- MR : variable SI on stage of hematoma
- Resolved after 2-3 year
Organizing hematoma is chronic state of fibrotic tissue surrounding a hemorrhage. Fig. 4
- US : a well-defined hypoechoic heterogeneous mass with surrounding increased echogenicity
- MR : intermediate T1 signal intensity and high T2 signal intensity with a thin hypointense peripheral rim and diffuse nodular enhancement
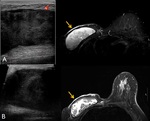
Fat necrosis is non-infectious fat degeneration by inflammatory changes or such as postsurgical disturbance of blood flow.
They usually shows gradual decrease in size on follow-up.
- Mammography : depicts a radiolucent well-defined cyst.
Fig. 5
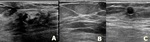
- US : typically hyperechoic intracystic lesion is seen and there is no blood flow. But,
it is difficult to completely distinguish it from solid mass or solid and cystic lesion by ultrasound only.
Fig. 6
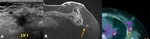
- MRI : high signal intensity on non-enhanced T1 weighted image and the disappearance of the high signal on fat suppressed image. Edge of the fat necrosis can show contrast enhancement by physiological reaction and inflammation,
and they mimic solid masses. Fig. 7
- FDG-PET/CT : fat also can easily be detected on CT, but FDG uptake is often be seen on the edge of the lesion by physiological reaction and inflammation Fig. 8
Post radiation change can be detectes as skin thickening and skin edema.
On FDG-PET, abnormal uptake can be seen up to 3 to 6 months after radiotherapy. Fig. 9
Dystrophic calcification could be occurred in degenerated or necrotic tissue,
and often seen after long-term course.
The diagnosis of benignity is not so difficult with its characteristic coarse calcification.
But,
during the forming progress of coarse calcification,
amorphous calcification or pleomorphic calcification may be seen,
and the definitive diagnosis is difficult,
thus appropriate follow-up is recommended with these cases.
4.
Multimodality imaging of breast cancer recurrence compared to primary disease
1) Recurred tumor in the breast
With adequate treatment,
it rarely occurs earlier than in the first 2 years.
During that period,
radiologic alterations are more likely to suggest benign process.
It may or may not appear in a similar fashion as the primary malignancy.
Also,
recurred tumors can develop at the contralateral breast.
So,
bilateral breasts should be evaluated.
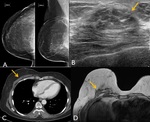
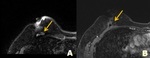
Most recurred lesion after MRM located around op bed.
Mammography is not useful to evaluate tumor recurrence after MRM. MRI sometimes played limited role because operation bed has tendency of underestimation.
(thin structure,
vulnerable artifact) Local recurrence after MRM tend to have palpable symptom.
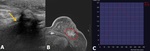
(superficial lesion) US or PET is more useful after MRM. Fig. 10
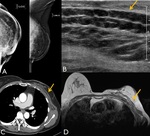
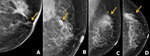
Most recurred lesion after BCS located on ipsilateral breast and especially around op site. Original cancer has tendency of high grade cancer,
more aggressive pathologic type or larger extent. Fig. 11 Fig. 12 Variable imaging modalities are used to detect recurred tumor after breast cancer surgery for follow up study.
[2,
5]
- MG
- It is less sensitive for the detection of recurrence in postconservative breast because of operation and radiation related alteration.
However,
it is more useful to detect suspicious calcifications than US or other imaging modalities.
- Increasing asymmetry,
enlarging mass within the operative bed
- Increasing edema,
overall trabecular pattern,
indicating lymphatic spread
- Pleomorphic,
coarse heterogenous or linear calcifications ; frequently same morphology as those found in the primary cancer
- US
- It is more sensitive and specific for the detection of recurrence than mammography.
However,
it may be difficult to differentiation between diffuse acoustic shadowing caused by scar and tumor,
and its sensitivity is limited for evaluation of small or noninvasive lesion.
- Circumscribed or ill-defined,
spiculated,
irregular,
hypoechoic mass
- Calcifications can be seen as echogenic foci.
- CT
- Its sensitivity and specificity are lower than other modalities,
but sometimes incidental findings can be detected on CT scan at first. Also,
it provides the anatomic information.
- Circumscribed or ill-defined,
spiculated,
irregular,
enhancing mass
- PET-CT
- It can detect unexpected uptake foci with higher sensitivity,
especially patients with heterogenous breast parenchymal background.
However,
small tumors can not be detected.
- Faint or intense hypermetabolic lesion
2) Regional lymph node recurrence
Regional lymph node recurrence occurs in about 1%-16% of breast cancer patients,
with associated with poor prognosis.
Preop nodal staging tend to lymph node recurrence. The axillary,
supraclavicular and internal mammary lymph nodes are the most common sites of regional lymph node recurrence. Patients with SCN or internal mammary lymph nodes tended to have axillary LN metastasis.
Sizes of benign and malignant nodes are similar.
Cortical morphologic feature appears to be of greater importance than size.
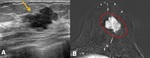
PET-CT is useful for detection of metastatic lymph nodes. Fig. 13
- MG
- The limitation of mammography is that the field of view of mammography does not include this entire area.
- Round shape,
more hyperdense than normal lymph node
- US
- Round or irregular shape,
thick and eccentric hypoechoic cortex (> 3mm in thickness),
loss of echogenic hilum,
less than 1.5 of long to short ratio,
with or without calcifications
- Internal mammary lymph node metastasis : normal lymphatic structures are not discernible with US,
but metastases appear as spherical or ovoid hypoechoic masses of uniform echogenecity,
confined to the intercostal space,
distinguishable from the internal mammary vessels on longitudinal scans.
- PET-CT
- It can show more accurate extent of node metastasis,
so more sensitive than other modalities
- Faint or intense uptake
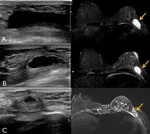
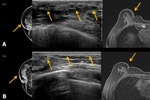
3) Recurrence of chest wall (skin)
It may occur by direct local extension of tumor through the pectoral fascia and into the pectoral muscles or by indirect extension via interpectoral nodes.
Ultrasonography is best modality to evaluate chest wall.
Prior to US scanning,
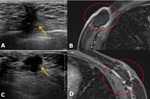
patients usually have palpable mass at the operative site or chest wall. Fig. 14
- MG
-It is often difficult to be detected because of small size and superficial location.
- US
- Circumscribed or ill-defined,
round,
ovoid or irregular,
taller than wide,
hypoechoic mass
- PET-CT
- Faint or intense uptake
5.
Differential diagnostic point of recurrences compared with benign post-operative change
Various benign condition (fat necrosis or benign reactive lymph nodes) sometimes mimic breast cancer recur. Correlation of other multimodality or clinical symptom can help in differentiating of recurrence from benign post op condition. Kinetic curve pattern of MRI and short term F/U imaging can be helpful. However,
when clinically suspected,
not hesitate to performing biopsy. Fig. 15