Radiological features indicative of TSC include:
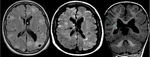
Intracranial manifestations: 1) Cortical tubers are areas of disorganized cortex commonly located at the gray-white juction (approximately 50% in the frontal lobes).
They are considered to be closely related to the neurologic manifestation of TSC,
including epilepsy,
cognitive disability and neurobehavioural abnormalities.
On magnetic resonance imaging (MRI),
cortical tubers tipically appear as well-circumscribed areas of low signal intensity on T1-weigthed images and hypertintense on T2-weighted and FLAIR.
In neonates and infants with a background of unmyelinated white matter,
cortical tubers have high signal on T1-weighted and low signal on T2-weighted images.
Tubers frequently demonstrate central cavitation or calcification (50%) and approximately 10% enhancement following contrast administartion.
2) Subependymal nodules are located around the wall of lateral and third ventricle (usually in close proximity to the foramen of Monro).
On MRI these lesions are iso or hyperintense on T2-weighted and hyperintense on T1-weighted sequences with variable enhancement.
They are more prone to calcification than cortical tubers,
tipically measure less than 1 cm but may grow over time and degenerate into Subependymal giant cell astrocytomas.
Subependymal giant cell astrocytomas can cause obstructive hydrocephalus (they are frequently located at the foramen of Monro),
are heterogeneous on MRI imaging (T1 iso/hypoinyense,
T2/FLAIR iso/hyperintense),
contain calcifications and demonstrate intense inhomogeneous enhancement.
3) White matter lesions include: superficial abnormalities,
radial migration lines and cyst-like white matter lesions.
Superficial white matter abnormalities are associated with almost all cortical tubers and exhibit T2 hyperintensity reflecting gliosis or decreased myelin content.
Radial migration bands are lines of bright T2 and FLAIR signal extending from the periventricular regions into the subcortical white matter and are believed to represent lines of arrested neuronal migration.
Cysts are frequently smaller than 1 cm,
located adjacent to the occipital horn and trigone of the later ventricle and follow CSF signal in all sequences.
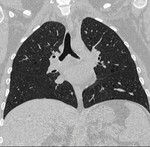
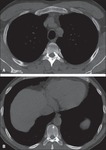
Pulmonary lesions : 1) Lymphangioleiomyomatosis is the most common pulmonary lesion characterized by diffuse interstizial proliferation of smooth muscle cells and cystic change in pulmonary parenchyma.
Computed tomography (CT) tipically shows diffuse,
well-circumscribed,
thin-walled lung cysts of variable size, which may communicate with the airways,
indicated by decrease in size on expiratory imaging.
Dyspnea and recurrent spontaneous pneumothorax are the most common presentations,
with slow and steady progression to respiratory failure.
2) Multifocal micronodular pneumocyte hyperplasia is a rare disorder associated with TSC identified on CT as multiple pulmonary nodules in a random distribution.
3) Clear cell "sugar" tumors of the lung are rare benign lung lesions appearing as rounded,
marginated,
peripheral parenchyma nodule or mass without evidence of cavitation or calcification.
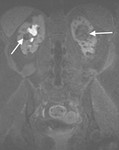
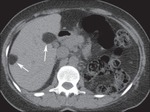
Renal manifestations: 1) Angiomyolipomas (AMLs) are the most common renal lesions in adults and older children with TSC; easly detected on CT as non calcified cortical masses contaning fat attenuation of less than -20 HU;
2) Renal cysts usually multiple and bilateral,
are the second most common kidney lesion.
Although renal cyst may occasionally be present in the fetus and neonate,
typically children with TSC are born with normal kidneys and develop cystic disease and AML as they age.
3) Renal cell carcinoma are rare,
manifest at an earlier age than in general population and their growth is slower than sporadic RCC.
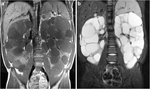
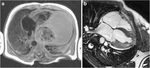
Cardiac rhabdomyoma which may be multiple or single,
are commonly located on the ventricluar septum.
Childhood regression is the rule,
with most of them regressing before birth and 70% by the age of 4 years.
These tumors are usually asymptomatic,
but in a minority of cases may present with cardiac failure or arhythmia when surgical resection may be considered.
Other manifestatons: Dermatological lesions including hypopigmented macules,
facial angiofibromas,
shagreen patches and ungula fibromas.
Involvment of various abdominal organs including epatic angiomyolipomas,
retroperitoneal LAM,
splenic hamartomas,
pancreatic lesions (AML and pancreatic neuroendocrine tumors),
hamartomatous colorectal polyps.
Perivascular epiteloid tumors (PEComas) are a family of mesenchymal tumors consisting of perivascular epitheloid cells.
On MRI,
they are hyperintense compared to the muscles on T2-weighted images.
Skeletal abnormalities such as cyst-like lesions,
hyperostosis of the inner table of the calvaria and osteosclerotic changes.
Retinal hamartomas present in 40-50% of patients with TSC.