Type:
Educational Exhibit
Keywords:
Breast, Mammography, Ultrasound, Diagnostic procedure, Education and training, Multidisciplinary cancer care
Authors:
D. Suleimenova1, M. Eghtedari2, H. Ojeda-Fournier2; 1La Jolla/US, 2La Jolla, CA/US
DOI:
10.26044/ecr2019/C-0182
Findings and procedure details
History of BI-RADS
-
First edition of BI-RADS® (Breast Imaging Reporting and Data System) released by ACR in 1993
-
Aims: Standardize and improve mammography interpretation,
simplify monitoring of outcomes,
assess radiologists’ performance, facilitate research and improve patients’ management and treatment
-
BI-RADS® contains: 1) Lexicon of descriptors,
2) Recommended reporting structure including final assessment categories along with management recommendations,
and 3) Framework for data collection and auditing
- BI-RADS Ultrasound and BI-RADS MRI were released in the 4th Edition in 2003 [3]
-
Multiple studies have shown that training in BI-RADS® can decrease variability and improve performance [4]
Overview of BI-RADS 5th edition on mammography [5]
- Indication for study
-
Description of breast composition
-
Description of important findings
-
Comparisons to prior examinations
-
Final assessment
-
Management recommendations
Lexicon for masses
|
Table 1.
Changes to the 5th BI-RADS edition: Masses
|
|
1. Shape
a. oval
b. round
c. irregular
|
-re-ordered oval and round
-Removed lobular (so an not to confuse with microlobulated margins)
|
|
1. Margin
a. circumscribed
b. obscured
c. microlobulated
d. indistinct
e. spiculated
|
-re-order microlobulated and obscured
|
|
2. Density
a. high-density
b. equal density
c. low density
d. fat-containing
|
- Removed “radiolucent” and replaced with fat containing
|
-
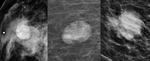
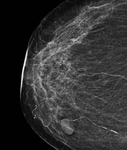
Shape (Figure 1): Round,
oval (with up to 3 slight undulations) or irregular
- “Lobular” was eliminated from the lexicon
- Margin: Circumscribed,
obscured (when >25% of margin is hidden),
microlobulated,
indistinct (without clear demarcation of the margin from surrounding tissue),
or spiculated
-
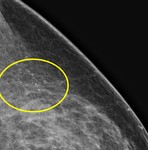
Density: High,
equal,
low,
or fat containing (Figure 2)
Calcifications
|
Table 2: Changes to BI-RADS 5th Edition: Calcifications
|
|
|
1. Typically Benign
a. skin
b. vascular
c. course or “popcorn- like”
d. large rod-like
e. round
f. rim
g. dystrophic
h. milk of calcium
i. suture
|
-Combined “eggshell” and “lucent-centered” into rim and “punctate” and “round” into round
-Re-order dystrophic,
milk of calcium,
and suture.
|
|
|
1. Suspicious Morphology
a.
amorphous
b.
course heterogeneous
c. fine pleomorphic
d. fine linear or fine-linear branching
|
**COMBINE Intermediate Concern,
Suspicious Calcifications and Higher Probability Malignancy **
- Removed “Intermediate Concern” in title
- Removed “indistinct”
-added fine pleomorphic
-added fine linear or fine-linear branching
|
|
| |
|
2. Distribution
a. diffuse
b. regional
c. grouped
d. linear
e. segmental
|
- Removed “scattered’
- Removed “clustered”
|
|
Morphology
- Typically benign: skin,
vascular,
popcorn-like,
large rod-like,
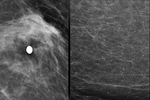
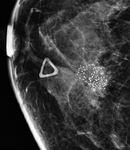
round (Figure 3)(now include round >0.5 mm and punctate < 0.5 mm in size),
rim (Figure 4) (now combines eggshell and lucent-centered),
dystrophic (>1 mm in size as compared to coarse heterogeneous),
milk of calcium,
suture
-
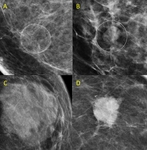
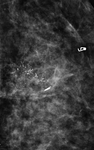
Suspicious: amorphous (Figure 5),
coarse heterogeneous (generally between 0.5 mm and 1 mm) (Figure 6),
fine pleomorphic (usually < 0.5 mm in diameter) (Figure 7),
and fine linear or linear branching (Figure 8) (BI-RADS 4c category) [6]
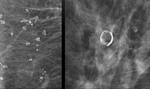
Distribution:
- Diffuse (previously scattered) (Figure 9)
-
Regional (>2 cm,
but do not follow ductal distribution)
-
Grouped (replace previous term clustered; used when more than 5 calcifications are grouped within 2 cm of each other) (Figure 10)
-
Linear
-
Segmental
|
Table 3.
Changes to the 5th BI-RADS Edition: Other
|
|
C.
Architectural Distortion
|
-unchanged
|
|
D.
Asymmetries
1. Asymmetry
2. Global Asymmetry
3. Focal Asymmetry
4. Developing Asymmetry
|
-added section for asymmetries alone
-added developing asymmetry
|
|
E.
Intramammary Lymph Node
|
** SEPARATE out findings of intramammary lymph node,
skin lesion,
solitary dilated duct **
- Removed “asymmetric tubular structure”
|
|
F.
Skin Lesion
|
|
G.
Solitary Dilated Duct
|
|
H.
Associated Features
1. Skin Retraction
2. Nipple Retraction
3. Skin Thickening
4. Trabecular Thickening
5. Axillary Adenopathy
6. Architectural Distortion
7. Calcifications
|
- Removed skin lesion (made into separate finding)
|
|
I.
Location of Lesion
1. Laterality
2. Quadrant/Clock-Face
3. Depth
4. Distance from the nipple
|
-added specification of quadrant and clock-face
-added distance from the nipple
|
Architectural distortion
Asymmetries
- Asymmetry (seen on one view only,
often represents superimposition of tissue)
-
Global (involves more than one quadrant of the breast,
assessed as a BI-RADS 2 category if no palpable correlate)
-
Focal: less than one quadrant
-
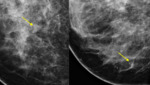
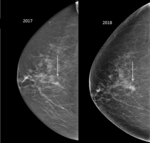
Developing (Figure 13)
-
New term in 5th Edition: asymmetry,
that is new,
larger,
or more conspicuous than on a previous mammogram
-
Note that the term density now applies to either the mammographic breast composition,
or the density within a mass
-
The term density should not be used to describe an asymmetry
Other findings
-
Skin lesion
-
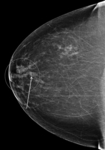
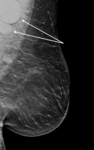
Solitary dilated duct (Figure 14),
note that the probability of malignancy is approximately 10%,
requires additional imaging and a possible tissue diagnosis
-
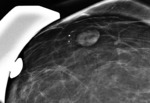
Intramammary lymph node (new category in the 5th Edition) (Figure 15)
Associated features
-
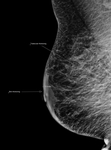
Skin retraction (Figure 16)
-
Nipple retraction
-
Skin thickening (Figure 17)
-
Trabecular thickening
-
Axillary adenopathy (Figure 18)
-
Architectural distortion (which can be a primary finding or an associated finding)
-
Calcifications (which can be a primary finding or an associated finding)
Location of lesions
-
Location of all suspicious findings should be fully described: laterality,
quadrant and clock face,
depth (anterior,
middle and posterior) and distance from the nipple in cm (new in the fifth Edition,
was introduced to parallel the descriptors used in the US and MRI sections)
Assessment categories: There has been no changes in the assessment categories in the 5th edition
- BI-RADS 1 (negative,
benign findings can be present on mammograms,
but not mentioned in the report)
-
BI-RADS 2 (benign,
when at least one of the findings is described in the report)
-
BI-RADS 3 (specified in this Edition,
that this is a separate category with probability of cancer >0% but <2%.
Used for non-calcified circumscribed solid mass,
focal asymmetry,
and solitary group of punctate calcifications)
-
BI-RADS 4 (use of subcategories is optional for mammography and US)
-
BI-RADS 5
-
BI-RADS 6
-
BI-RADS 0 (used mainly in screening setting)
Review of ACR mammographic density
-
Important because increased breast density:
1) Can mask lesions and may be associated with increased breast cancer risk
2) Lowers the sensitivity of mammography [8]
-
The fifth edition eliminates quartile ranges of percent dense tissue to define the descriptors of breast composition
-
Assessment of density is subjective and based on a visual estimate
-
Density category should reflect the masking effect of dense fibroglandular tissue on mammographic depiction of noncalcified lesions [9]
-
Density categories are now listed as A,
B,
C,
and D so as not to be confused with the numbered BI-RADS® assessment categories
-
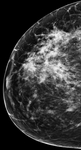
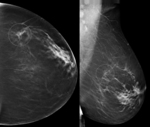
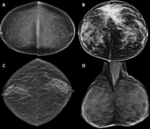
Four mammographic density categories (Figure 19):
A: Almost entire fatty
B: Scattered areas of fibroglandular tissue
C: Heterogeneously dense
D: Extremely dense
Overview of BI-RADS® 5th Edition on US [10]
- Indication for study
-
Scope (whole breast v.
targeted) and technique (automated v.
handheld)
-
Description of breast composition
-
Description of findings
-
Comparisons with previous studies and/or correlations with different modalities
-
Combined reports
-
Final assessment
-
Management recommendations
- General Considerations section discusses broad topics of normal breast anatomy,
image quality related issues,
labelling of images and measuring of findings.
-
Measurements of important findings: longest axis of a lesion,
perpendicular measurement; and a third measurement orthogonal to the first image
-
All measurements in cm or mm consistenly
-
Simple cysts and benign intramammary lymph nodes may be omitted in the report and assigned BI-RADS category 1 Negative
Homogeneous background echotexture- fat
Homogeneous background echotexture- fibroglandular
Heterogeneous background echotexture
An additional new descriptor to be used in males is: Benign male gynecomastia (Figure 21)
|
Table 4.
Changes to the 5th BI-RADS edition: Ultrasound
|
|
A.
Tissue Composition
|
· RENAMED
|
|
1. Homogeneous Background Echotexture – Fat
2. Homogeneous Background Echotexture – Fibroglandular
3. Heterogeneous Background Echotexture
|
|
|
B.
Masses
|
|
1.
Shape
a.
Oval
b. Round
c. Irregular
2.
Orientation
a.
Parallel
b.
Not Parallel
3. Margin
a. Circumscribed
b. Not Circumscribed
i. Indistinct
ii. Angular
iii. Microlobulated
iv. Spiculated
4. Echo Pattern
a. Anechoic
b. Hyperechoic
c. Complex Cystic and Solid
d. Hypoechoic
e. Isoechoic
f. Heterogeneous
5. Posterior Features
a. No Posterior Acoustic Features
b. Enhancement
c. Shadowing
d. Combined Pattern
|
·Removed lesion boundary category
·CHANGE complex echo pattern descriptor to complex cystic and solid
· added Heterogeneous descriptor for echo pattern
· Removed surrounding tissue category (some descriptors added to D.
Associated Features,
below)
|
|
C.
Calcifications
|
|
1. Calcifications in a Mass
2. Calcifications Outside of a Mass
3. Intraductal Calcifications
|
· Removed micro/macro distinction
· added intraductal
|
|
D.
Associated Features
|
|
1. Architectural Distortion
2. Duct Changes
3. Skin Changes
a. Skin Thickening
b. Skin Retraction
4. Edema
5. Vascularity
a. Absent
b. Internal Vascularity
c. Vessels in Rim
6. Elasticity Assessment
a. Soft
b. Intermediate
c. Hard
|
· added associated features category (includes descriptors from previous lesion boundary and vascularity categories)
· added descriptors for elasticity assessment
|
|
E.
Special Cases
|
|
|
1. Simple Cyst
2. Clustered Microcysts
3. Complicated Cyst
4. Mass In or On Skin
5. Foreign Body Including Implants
6. Lymph Nodes – Intramammary
7. Lymph Nodes – Axillary
8. Vascular Abnormalities
a. AVMs
b. Mondor Disease
9. Postsurgical Fluid Collection
10. Fat Necrosis
|
· This section is expanded
|
|
E.
Vascularity
|
· Removed dedicated vascularity section
|
Masses
-
Shape: Round,
oval and irregular (Figure 22)
- Orientation: parallel and not-parallel (“wider than tall”,
“taller than wide” ,
“vertical”,
“horizontal” were eliminated from the lexicon)
-
Margin: circumscribed or not circumscribed,
that can be further described: indistinct,
angular,
microlobulated,
spiculated
-
Echopattern: anechoic,
isoechoic,
hypoechoic,
hyperechoic,
heterogeneous (Figure 23),
and the new term complex solid and cystic (Figure 24) replaces “complex mass”
-
Posterior features: enhancement,
shadowing,
combined pattern,
no posterior features are also unchanged
Calcifications
-
In a mass,
outside of a mass,
and intraductal calcifications (Figure 25) are new descriptors
-
No division into micro or macrocalcifications
Associated findings
Associated features
-
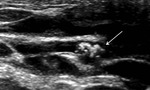
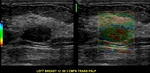
Vascularity: absent,
internal vascularity and rim vascularity
-
Elasticity: soft,
medium and hard,
color descriptor is not accepted (Figure 26)
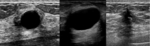
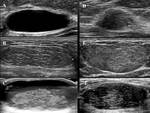
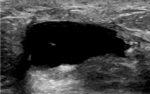
Special cases
-
Clustered microcyst,
complicated cyst,
mass in or on skin,
foreign body including implants
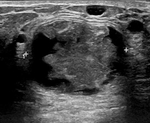
-
Lymph nodes: intramammary and axillary
-
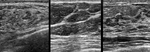
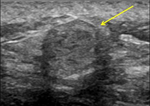
Simple cyst,
postsurgical fluid collection (Figure 27),
fat necrosis (Figure 28),
arteriovenous malformations/pseudoaneurysm,
Mondor disease (Figure 29) have been added to the lexicon
-
Following parameters to describe lymph nodes:
-
Size in longest dimension
-
Shape: oval,
round,
irregular
-
Cortical thickening: uniform v.
focal
-
Margin: circumscribed v.
not circumscribed
-
Hilar compression or displacement
-
Combined modality reporting: Issue a composite report if more than one modality studies are performed on the same day
-
Assessment categories same as in mammography[11]
Aims of changes in BI-RADS® lexicon [12]
-
Harmonization of descriptors across all breast imaging modalities to increase consistency
-
Elimination of descriptors rarely or improperly used
-
Consolidation of descriptors with the same prognosis and management (eg. typically benign egg shell and lucent centered)
-
Stratification of the findings with different level of probability for malignancy (4A,
4B,
4C)
-
Incorporation of new emerging technology (elastography)
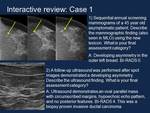
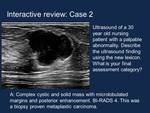
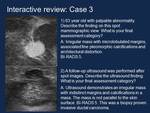
Interactive case review testing the recent changes to BI-RADS 5th edition (Figures 30-32)