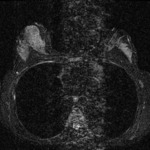
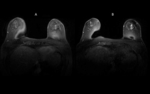
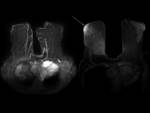
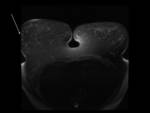
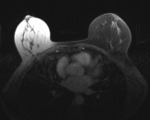
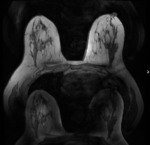
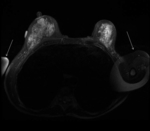
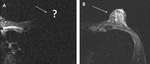
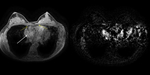
(Figure 1)
Brief description of MRI indications and contraindications
Indications:
High risk screening – Begin at age 25 years old
-
Greater than or equal to 20% lifetime risk of breast cancer
-
BRCA 1,
BRCA 2,
CHEK2,
p53 mutations [2]
-
Other genes and syndromes (Li-Fraumeni,
Cowden syndrome,
etc.)
-
Strong family history of breast and ovarian cancer (more than one first degree relative with breast or ovarian cancer)
-
Chest mantle radiation in childhood
Intermediate risk screening
-
Moderately elevated risk of breast cancer (15%-20%)
-
Personal history of breast cancer diagnosed under the age of 50
-
One first degree relative with breast and/or ovarian cancer
-
Dense breast tissue as a supplemental modality
Newly diagnosed breast cancer [3]
-
To assess the extent of disease in the ipsilateral breast [4]
-
To identify potential breast cancer in contralateral breast
-
To identify the potential presence of multifocal and multicentric disease
-
To assess tumor invasion to pectoralis muscle or chest wall
Assessment of silicone gel filled breast implant integrity (without contrast)
Evaluation of post-lumpectomy changes with positive margins
Response to neoadjuvant chemotherapy [5]
Suspected breast cancer recurrence and post operative tissue reconstruction [6] [7]
Axillary lymph node metastasis primary unknown
MRI-guided biopsy
Other considerations in performing breast MRI
-
Preferably scan between day 3-21 of menstrual cycle in screening patients,
but should not delay imaging in pre-menopausal patients with new diagnosis of breast cancer to time with menstrual cycle
-
Lactational changes can limit evaluation but is no longer considered a relative contraindication for breast MR
-
In patients with positive margins MR can be performed when patient is comfortable enough to be positioned for the study
-
Comparison mammograms and other relevant breast imaging studies should be available at the time of image interpretation
Contraindications:
-
Allergy to gadolinium based contrast agents
-
Moderate to end-stage renal disease
-
Claustrophobia
-
Presence of metallic objects such as pacemakers,
clips,
neurostimulators,
implants and other ferromagnetic objects which are not MR compatible
-
Pregnancy
Overview Of Breast MRI Protocol And Technique
General technical considerations [8]
-
Dedicated bilateral breast MRI coil is required
-
Minimum field strength of 1.5 T
-
Slice thickness less than 3 mm
-
In-plane pixel resolution 1 mm or less to minimize volume-averaging effects
-
Chemical fat suppression is helpful however is not required: use of fat suppression is recommended on sequences used to assess contrast enhancement
-
Post processing motion correction may be helpful in reducing artifacts
-
Simultaneous bilateral high-resolution imaging
-
Gadolinium based contrast enhancement is required for the evaluation of breast parenchyma but not breast implants
-
Pre-contrast imaging followed by dynamic sequences
-
Kinetic assessment based on enhancement data at intervals no longer than 4 minutes
- Short temporal resolution for accurate capture of lesion kinetics
-
MR imaging biopsy technology highly recommended to be available
Our institution standard MR protocol includes:
-
Bilateral breast imaging in a dedicated breast coil
-
Localizer sequence
-
Coronal T2-weighed sequence
-
Axial T2-weighted fat-saturated fast spin echo (SE)
-
Axial non-fat-saturated T1-weighted sequence
-
Axial fat saturated pre- followed by five dynamic post-contrast T1-weighted spoiled gradient echo
- High resolution delayed T1-weighed sequence for better assessment of lesion morphology and internal mammary lymph nodes
-
Post processing:
-
We use both fat suppression and subtraction dynamic pre and post-contrast sequences
-
Computer-assisted detection system used for generating subtraction and MIP images,
kinetic assessment,
and three-dimensional reformatting
MR Artifacts
Patient-related MR artifacts
Motion
-
Reduced signal intensity of a moving structure and blurring of the image can obscure lesions
-
Physiologic: can be caused by fluid,
including pleural fluid,
bowel movement,
or cardiac or arterial pulsation
-
Non- physiologic: due to patient motion (Figure 2)
What to do?
-
Ensure patient’s comfort and convenient positioning BEFORE the start of the study
-
Communicate with the patient the importance of being still during the examination [9]
-
Consider sedation if patient is claustrophobic
Artifacts due to body habitus [10]
What to do?
Susceptibility artifacts (Figure 5 and 6)
-
Cause: titanium biopsy clips [11],
median sternotomy wires,
infusion ports,
other ferromagnetic foreign bodies or electronic devices
-
Inhomogeneity in the magnetic field results in local signal intensity void in the vicinity of the metal,
often with a surrounding area of high signal intensity and image distortion [12]
What to do?
-
Any non implantable metallic objects need to be removed from the patient prior to entering the magnet
-
Marker clip susceptibility artifact can be used during image interpretation to correlate site of biopsy
Associated with equipment
Inhomogeneous fat saturation (Figure 7)
-
Fat suppression can be achieved by different methods depending on MR manufacturer,
usually automatically by MR unit software
-
Inhomogeneous fat saturation can be due to field inhomogeneity
-
More common in fatty breasts
-
Results in areas of hyperintense fat on fat-suppressed images,
hindering the assessment of enhancing lesions on post-contrast T1 sequences
-
Can affect portions of the breast or the entire breast
-
Fat saturation takes time and this needs to be taken into account when setting high temporal resolution of the study
What to do?
-
The center frequency must be set as accurately as possible to the water peak
-
Shim volumes positioned correctly by technologist [13]
-
An alternative to fat saturated dynamic imaging is subtraction,
but it's essential for the patient to stay still during the examination as misregistration will limit the interpretation of subtraction images
Phase encoding artifact (Figures 8-10)
-
Periodic physiologic motion such as pulsation of heart or big arteries results in ghosting
-
Occurs at regular intervals in the phase-encoding directions (LR v.
AP,
etc.)
-
Appropriate direction is left to right for axial images and superior to inferior for sagittal images
-
Otherwise ghosting artifact may obscure breast parenchyma
What to do?
Misregistration
-
Due to patient movement between sequences to be subtracted
-
A type of motion artifact seen exclusively on subtraction images
-
Can obscure lesions or create pseudo lesions
-
Can lead to nulling in the image (Figure 12)
What to do?
-
Ensure that the patient is still during the entire examination
-
If misregistration artifact is suspected,
unenhanced and contrast- enhanced source images should be closely inspected
Wraparound (Figures 13 and 14)
-
Due to tissue located outside the prescribed imaging field of view [14]
-
Results in appearance of anatomic structures where they do not belong through misregistration during Fourier transform reconstruction
What to do?
RF interference artifact (Figure 15)
-
Due to source of RF signal in the magnet room or leak in the RF shield surrounding the MR unit allowing the RF signals from outside to penetrate the shield [13]
-
Results in appearance of high-signal-intensity bands over the entire image,
not just within the breast,
that propagate in the phase encoding direction
What to do?
-
Make sure the MR imaging room door is completely closed during the examination
-
Make sure there is no source of RF signal inside the imaging room
-
Make sure the room is appropriately shielded
Technologist-related
Positioning (Figure 16 and 17)
-
Improper positioning of the breasts into the breast coils
-
Can appear as an area of high signal intensity where breast tissue is adjacent to coil and loss of symmetry [9]
-
Be aware of large portions of the breast left outside the coil
-
Challenging for patients with big breasts,
patient with back or shoulder problems
What to do?
Incorrect use of breast coil (Figure 18)
-
The breast coil has elements that can be used for either the right or left breast,
or both breasts simultaneously
-
Appropriate coil elements need to be selected by the technologist
Inappropriate contrast administration (Figure 19 and 20)
-
Due to poor intravenous access,
failure of power injectors,
and intravenous tubing malfunction,
or patient’s hemodynamic status
-
Complete absence of contrast administration is identified as no enhancement in the heart,
superficial vessels,
and absence of normal nipple enhancement
-
Poor contrast material bolus is more difficult to notice
- Could result in missing malignant lesions
What to do?
-
Assess each study for contrast enhancement quality
-
In case of complete lack of enhancement study is considered non-diagnostic and needs to be repeated
-
If contrast material bolus is of questionable quality,
either a repeat examination or a short-interval follow-up can be considered,
taking into account the pretest probability of malignancy in each individual case
Early contrast administration (Figure 21)
-
Due to administration of contrast during the pre-contrast phase
-
Identified when enhancement is seen in heart and vessels in pre-contrast images
-
Results in nulling on subtraction images
What to do?