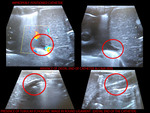
We studied a total of forty-five neonates.
Twenty-three of these were (51.11%) female and 22 (48.89%).
(See Fig. 3,
Graphic 1).
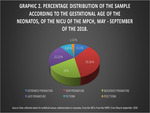
The dominant gestational age group was extreme prematurity with 20 neonates (44.44%).
(See Fig. 4, Graphic 2).
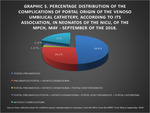
Of the 45 neonates with umbilical vein catheterization,
36 (80.00%) presented complications (See Fig. 5, Graphic 3).
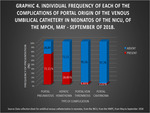
The most frequent complications were portal pneumatosis with a frequency of 71.11%,
followed by liver hematomas with 28.89%,
portal thrombosis with a frequency of 4.4% and portal cavernomatosis with 2.2 %.
(See Fig. 6,
Graphic 4).
Compared to a previous study by Ji HK et al.
(10) ,
the frequency of portal thrombosis in our study is low (43% vs.
4.4%,
respectively).
More than one complication in the portal venous system could arise in the same neonate.
A large part of the complications were associated.
(See Fig. 7, Graphic 5).
Of the 9 patients with moderate prematurity,
all of them developed complications after umbilical vein catheterization.
The single post-term patient studied also developed complications after catheterization.
However,
this frequency did not have a direct relationship with gestational age,
but rather with the correct or incorrect positioning of the umbilical venous catheter.
(See Fig. 8,
Graphic 6).
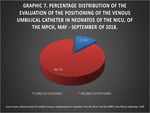
The evaluation of the positioning of the catheter indicated that 39 neonates (86.7%) had catheters that were incorrectly positioned and 6 (13.3%) were properly positioned.
This is a low percentage compared to the results reported in a study by Lloreda et al.
(7). (See Fig. 9,
Graphic 7).
Of the 39 neonates with incorrect positioning of the catheter,
36 (92.31%) presented portal system complications and 3 (9.69%) presented no complications.
We found no complications in the 6 neonates who had an adequately positioned umbilical vein catheter (See Fig. 10,
Graphic 8).
A statistically significant relationship was determined between the incorrect positioning of the umbilical venous catheter and the presence of all types of portal system complications (portal pneumatosis,
portal thrombosis,
portal cavernomatosis and hepatic hematomas),
Fisher's exact test value of 0.001.
There is a statistically significant relationship between the incorrect positioning of the umbilical venous catheter with the presence of portalpneumatosis assessed individually (Fisher's exact test p value of 0.001).
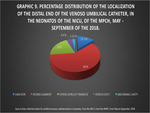
We found that the most frequent position of the distal end of the umbilical vein catheter was at the level of the round ligament,
present in 27 neonates (60%).
(See Fig. 11 and Fig. 12,
Graph 9).
Although some studies report that inadequate positioning of the umbilical venous catheter,
especially when it is positioned in the portal vein (as this conditions the presence of portal thrombosis and subsequently other complications such as portal cavernomatosis and portal hypertension),
it was not possible to demonstrate a statistically significant relationship between the incorrect positioning of the catheter and the presence of the most serious complications such as thrombosis and cavernomatosis of the portal vein evaluated individually,
probably because they are complications whose presentation occurs late.
This,
associated with deaths in the NICU,
discharges,
and some medical limitations limited the follow-up of neonates,
thus reducing the possibility of diagnosing late complications compared to those that occur predominantly early,
such as portal pneumatosis and hepatic hematomas.
Likewise,
the fact of removing the catheter incorrectly positioned early for ethical reasons by identifying the incorrect positioning of the catheter could have conditioned alterations in relation to what would have occurred in a natural environment (not evaluated after its placement by ultrasound).
These changes contributed to some degree of bias during the study.
(2).
We found a higher percentage of females rather than males with portal system complications (85.95% vs 72.2%,
respectively).
However,
gender is not significantly related to the presence of complications (Fisher's exact test p value of 0.96).
(See Fig. 13,
Graph 10).