Type:
Educational Exhibit
Keywords:
Multidisciplinary cancer care, Education and training, Cancer, Technical aspects, Localisation, Ultrasound, Mammography, Oncology, Interventional non-vascular, Breast
Authors:
D. Suleimenova1, M. Eghtedari2, H. Ojeda-Fournier2; 1San Diego/US, 2La Jolla, CA/US
DOI:
10.26044/ecr2019/C-0365
Findings and procedure details
Historical perspective
-
There is no difference in disease free survival in patients undergoing mastectomy v.
BCS with radiation [2]
-
Non-palpable lesions detected by mammography required preoperative localization to guide the surgeon in performing a cosmetically acceptable lumpectomy
-
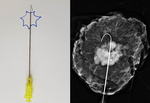
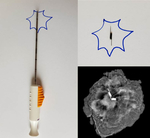
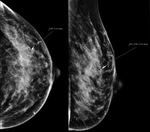
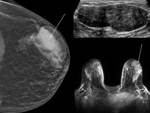
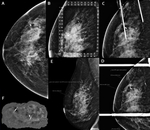
Wire localizations were introduced in the 1970s and for many years had served as the only method for preoperative breast localization (Figure 1)[3]
-
Disadvantages of wire localization include:
- Scheduling challenges,
as wire must be placed on the same day as the surgical procedure
-
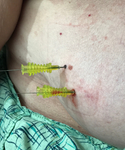
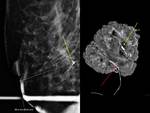
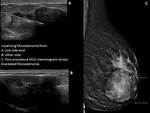
Uncomfortable for the patient because the wire protrudes from the skin until surgery (Figure 3)
-
Risk of wire migration as patient is transferred from breast imaging suite to the operating room [4]
-
Limits surgical approach,
the placement route of the wire chosen by the radiologist often dictates incision location
-
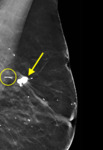
Wire transection can result in a retained wire fragment (Figure 4) [5]
-
Possible injury to neighboring organs (rare case reports of wire causing delayed cardiac injury by penetrating pericardium and wire migration into thoracic cavity) and implants rupture
-
Radioactive seeds (radiolabeling a titanium seed with Iodine-125)
-
Radar reflectors (RF) (Figure 5)
-
Magnetic seed system (labelling lesion with magnetic marker)
Overview of RF localization technique
-
Approved in the United States by FDA in 2014
-
This system uses a radar reflector activated by infrared light
-
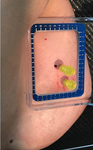
Radar system has 3 components: single use sterilized device preloaded into a needle introducer (Figure 6),
reusable small localizing console which provides audible and visual feedback and dedicated handheld intraoperative probe (Figure 7)
-
Radiologist injects the reflector under image guidance in the center of the targeted lesion at any time before surgery
-
Currently FDA approved for permanent implantation
-
Mammographic,
tomosynthesis,
or ultrasound guidance can be used
-
The reflector is 12 mm in length,
with a 4-mm body and 2 antennas each 4 mm in length,
and can be inserted through a preloaded 16-gauge introducer needle (Figure 8)
-
During surgery,
the surgeon activates the reflector with the hand piece and follows the signal to guide the excision (Figure 9)
-
There are 7 studies (5 retrospective and 2 prospective) identified in the literature [7-13] and summarized in table 1:
|
|
Study by Falcon S et al.
(2018)
|
Study by Mango et al.
(2016)
|
Study by Patel S.
(2018)
|
Study by Cox C (2016)
|
Study by Mango et al.
(2017)
|
Study by Cox et al.(2016)
|
Study by Jadeja et al.
(2017)
|
|
Number of patients (number of reflectors placed)
|
129 (152)
|
13 (15)
|
42
|
50
|
100 (123)
|
154
|
42 (90)
|
|
Nature
|
Retro
|
Retro
|
Retro
|
Pro
|
Retro
|
Pro
|
Retro
|
|
Rate of successful reflector placement
|
97%
|
100%
|
100%
|
100%
|
99.9%
|
99.9%
|
100%
|
|
Rate of successful removal
|
100%
|
100%
|
100%
|
100%
|
100%
|
100%
|
100%
|
|
Complication rate and types
|
0
|
0
|
0
|
0
|
0
|
0
|
0
|
|
Rate of reflector migration
|
0.8%
|
7%
|
0
|
0
|
5.5%
|
0
|
0
|
|
Rate of positive margins
|
Not assessed
|
0%
|
9.5%
|
7%
|
7.4%
|
14.9%
|
10.3%
|
|
Mean distance from clip to target
|
6 mm
|
3 mm
|
4 mm
|
2.8 mm
|
3 mm
|
2.8 mm
|
Not reported
|
All studies reported:
-
Negative margin rate of 85%-100% (comparable or higher than that with wire localization)
- Complication rate of 0%
-
Rate of successful placement of 97-100%
-
Rate of successful removal of 100%
-
Mean distance between reflector and target 2.8- 6 mm
-
Technical issues: inaudible signal from the skin (most common),
majority of reflectors were identified immediately after skin incision,
some reflectors were defective,
others were disabled after contact with electrocautery
Pros:
-
Can be placed any time before surgery as they have no restriction on length of time they can remain in the breast [14]
-
Non-radioactive
-
Allow independent scheduling of image-guided localization from surgery
-
Improved workflow for radiology suite and surgery
-
Comparable or lower re-excision rate for positive margins
-
Does not affect the incision site
-
Surgeons rated RF reflectors better than wires for incision site planning,
tissue localization,
confidence in removing the correct target,
and ease of specimen removal [7]
-
Less likelihood of migration as compared with wire
-
Improved patient’s experience
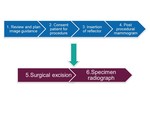
Algorithm (Figure 10)
- Review imaging to plan approach for localization target (lesion or clip)
-
Select modality in which lesion is seen best (mammographic/tomographic or ultrasound)
-
Obtain patient consent
- Prep the skin
-
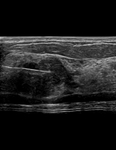
Localize the lesion
-
Administer local anesthetic
-
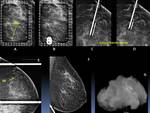
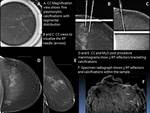
Place the introducer needle tip within the target (Figure 11)
-
Unsheathe the reflector by retracting the release button
-
Test that the reflector can be detected
-
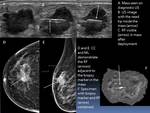
Obtain post procedural mammograms for surgical planning (Figure 12)
-
Annotate images for surgeon to review
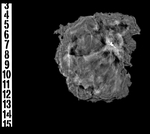
- Obtain specimen radiograph to confirm removal of the target and localization device (Figure 13)
Limitations to wireless localization and strategies to overcome them
Limitations
-
Inability to reposition the reflector once deployed
-
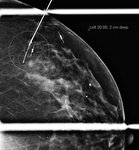
Maximum detection depth of 4.5 to 5 cm (may not produce a detectable signal if lesion is too deep) [8] (Figure 14)
-
Currently RF is not approved in the USA for deployment under MR guidance (however if the device is in place,
the patient can have MRI)
-
Successful case of MRI guided reflector placement was reported by Falcon S.
et al.
in 2018 [13]
-
The reflector is MR conditional due to the presence of nickel and ferromagnetic properties based on non-clinical testing
-
Potential to disable the reflector if direct contact by electrocautery [8]
- The use of halogen lights that emit infrared radiation in surgery room may also interfere with the signal
-
Significantly more expensive compared to wires
-
Require additional equipment in radiology suit and surgery room
Strategies for success
Inaudible signal after deployment [13]
-
Re-position the patient and try to detect signal from different angle
-
Confirm that the reflector was deployed,
i.e.
review post procedure mammogram
-
Remove any covers (gloves/sterile drapes) from the console handpiece placed there for infection control purposes
-
Try to obtain signal with operating room console,
the console in radiology suite is not as powerful as the one for operating room
-
Avoid placing RF within a hematoma
-
If audible signal remains undetectable,
a wire can be placed the day of surgery
-
Wires or large surgical clips may interfere with signal detection
-
Inaudible reflectors may be identified after skin incision [8]
Two targets within the same breast
Localization of an axillary lymph node
Post biopsy hematoma
-
When placed within a hematoma or seroma,
the RF localizers “float” which may lead to migration [10]
-
What to do?
- Place reflector adjacent to hematoma not within
-
Localize target with a wire if hematoma is an issue
Cases
Figures 18,
19,
20 and 21