Demographics
Between July 2017 and February 2018,
CBCTs were performed on 269 patients.
103 were excluded as they were for evaluation of known fractures,
post-operative imaging or chronic pain assessment.
166 scans were performed patients with suspected radiocarpal fractures after trauma despite no fracture visible on initial radiographs.
49 were excluded as CBCT was performed over 2 weeks after wrist trauma.
117 were performed within the predetermined time limit of 2 weeks for acute fracture.
The median number of days from initial trauma to CBCT was 9.
This patient group was 51.2% male with an average age of 41,
median of 39 and range was 16-81.
Right sided wrist fractures were significantly more common than left sided wrist fractures (P<0.001).
The most commonly suspected fracture on the clinical request was of the scaphoid,
listed as the bone of concern in 76.9%.
Six CBCT studies were suboptimal (3 conducted with the wrist in a cast and 3 with motion artefact) but considered assessable by all reviewers.
Fracture identification
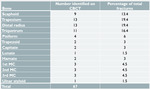
The results for detection of radiocarpal fractures are presented in Table 1. 59 (50.7%) of the 105 patients had an acute fracture identified on CBCT.
6 patients had more than one fracture with a total of 67 fractures identified.
The most commonly fractured bones were the distal radius (13) and trapezium (13),
each accounting for 19.4% of fractures in the cohort.
16.4% were triquetral fractures and 13.4% were scaphoid fractures.
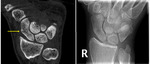
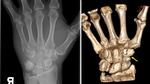
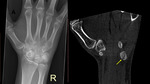
Fig.
2 & 3
18 of the 117 patients had a non-specific cortical abnormality on initial radiographs.
7 of these correlated with acute fractures on CBCT,
while 9 patients had no fracture on CBCT and 2 patients had an acute radiocarpal fracture diagnosed in a bone separate from the bone with the cortical abnormality.
Gold standard for the presence of a fracture was taken as clinical follow up with MRI in cases with persistent clinical concern for fracture in cases with negative CBCT and in cases with no focal pain at the site of reported fracture.
8 patients had follow up MRI which identified 1 scaphoid fracture which was not on CBCT.
One patient also had scaphoid oedema without a fracture line on T1 sequence,
deemed not to represent a fracture for this study.
All fractures identified on CBCT corresponded clinically to fracture on examination.
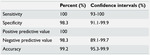
CBCT had a sensitivity of 98.3% (95% CI: 91.1%-100%),
specificity of 100% (95% CI: 93.7% to 100%),
PPV of 100%,
and NPV of 98.3% (95% CI: 89.1% to 100%).
Accuracy was 99.1% (95% CI: 95.3%-100%).
Table 2
 Inter-rater agreement for CBCT
Inter-rater agreement for CBCT
3 of the fractures identified on CBCT by the senior radiologist were not diagnosed by the junior radiologist.
The agreement rate between the two radiologists was K = 0.948 (95% CI 0.89-1).
 Fracture Characterisation
Fracture Characterisation
25 (37.3%) of fractures were characterised as displaced.
44 (65.7%) of fractures extended into the trabeculae of the injured bone while 23 (34.3%) involved only a cortical fragment.
Comminution was identified in 8 (11.9%) fractures,
of which none had identified fracture on radiographs.
 Retrospective radiograph review
Retrospective radiograph review
In cases where CBCT identified a fracture,
the patient’s radiographs were re-assessed to identify if the known fracture was visible in retrospect.
When injured bone,
site and size of fracture was known,
fractures could be confidently identified in 17%,
indeterminate cortical abnormalities were seen in 25.4% and no abnormality was present in 57.6%.
Fig.
4
 Radiation Dose
Radiation Dose
CBCT had a set DLP for the imaging protocol used,
of 35.3mGy/cm.
Median Dose Area Product (DAP) for combined radiographs was 0.36 mGy/cm2.