Keywords:
Interventional non-vascular, Oncology, CT, Ultrasound, Biopsy, Cancer, Metastases
Authors:
M. Goicea1, C.-I. Betianu2; 1Bucharest, ro/RO, 2BUCHAREST/RO
DOI:
10.26044/ecr2019/C-0573
Results
The study group consisted of 91 women (26%) and 259 men (74%).
The mean age of the group was 65,
with ages ranging from 29 to 92 years old.
Our study sample included 317 lung procedures and 47 non-lung procedures.
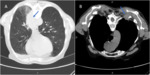
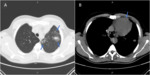
The non-lung procedures included 23 bone (Fig. 1),
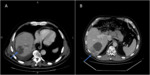
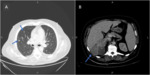
12 hepatic (Fig. 2),
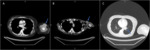
7 small parts (muscle) (Fig. 3),
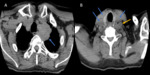
2 lymph nodes (Fig. 4),
2 mediastinal (Fig. 5) and 1 adrenal (Fig. 6) procedures.
One patient had to undergo multiple-site procedures due to uncertainty regarding the origin of synchronous lesions,
namely a pulmonary lesion and a mediastinal lesion.
13 patients had to undergo a second biopsy,
due to insufficient or inadequate tissue for histopathologic characterization of the target lesion.
For 14 lung procedures and 1 non-lung procedure (hepatic) we did not have information about the histopathologic result,
as the patients preferred to have their tissue samples examined in a different medical facility.
Biopsy-related complications were found in 10% of procedures in the lung biopsy group (SD=0.306) and 0% in the non-lung biopsy group (SD=0) (p<0.05).
The complications consisted of 25 pneumothoraces,
3 haemothoraces,
7 alveolar haemorrhages with haemoptysis and 1 infection at the puncture site.
Of them,
10 needed additional medical attendance – 9 drainage tube insertions,
for 8 pneumothoraces and 1 pneumo-haemothorax,
and 1 surgical debridement for infection.
The histopathologic valid result rate did not differ significantly between the two groups,
with a mean of 82% valid results in the lung biopsy group (SD=0.378) and 89% in the non-lung biopsy group (SD=0.315).
An important limitation to our study is that the lung-procedure group was not further separated into procedures in lesions with pleural contact and lesions without pleural contact,
which is the most relevant factor to determine the risk of complications in lung procedures [3,4].
This was caused by an inconsistent system for storage of images used in our department for biopsy procedures between 2015 and 2018.
The protocol is now standardized,
but admitting in the study only patients for which we had intra-procedural images stored would have dramatically decreased the width of our study group.