1.1 Male Urethra Anatomy
The male urethra is a narrow fibromuscular tube that conducts urine and semen from the bladder and ejaculatory ducts,
respectively,
to the exterior of the body.
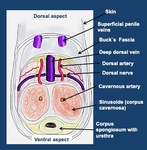
It commences at the internal urethral orifice in the trigone of the bladder and opens in the navicular fossa of the glans penis at the external urethral meatus (Fig. 1).
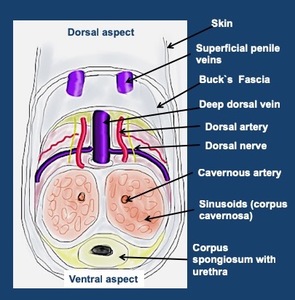
Fig. 1: Urethra Anatomy
The male urethra can be divided into anterior and posterior portions.
The anterior urethra is composed of the penile and bulbar urethra to the level of the urogenital diaphragm.
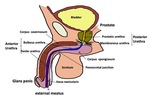
The posterior urethra is composed of the membranous and prostatic urethra (Fig. 2).
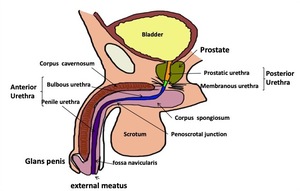
Fig. 2: Urethra Anatomy
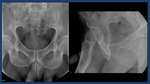
Radiologic anatomy:
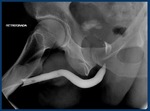
-Normal retrograde urethrography:
The anterior urethra,
is formed by the penile urethra (yellow arrow) and the bulbar urethra (blue arrow).
The posterior urethra,
including membranous (red arrow) and prostatic urethra (green arrow) is better evaluated with voiding studies.
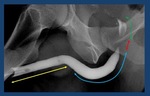
(Fig. 3).
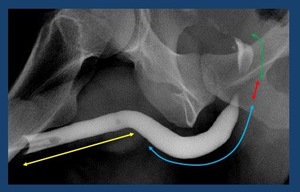
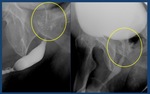
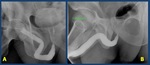
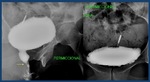
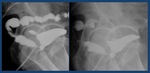
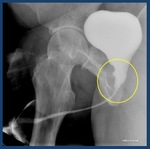
Fig. 3: Normal retrograde urethrography. The anterior urethra, is formed by the penile urethra (yellow arrow) and the bulbar urethra (blue arrow). The posterior urethra: membranous (red arrow) and prostatic urethra (green arrow) is best evaluated with voiding studies.
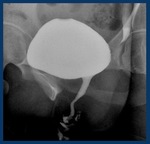
-Normal voiding urethrography:
Useful for posterior urethra (membranous and prostatic regions).
The Anterior urethra is better evaluated in retrograde studies in which a better repletion is achieved.
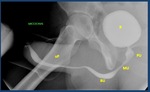
B: bladder ( Fig. 4 )
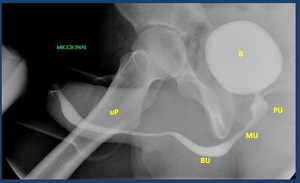
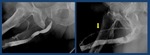
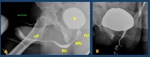
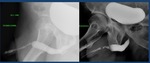
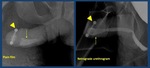
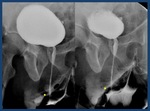
Fig. 4: Normal voiding urethrography. It depicts the posterior urethra. PU. Prostatic urethra with a normal central repletion defect ( veru montanum) . MU: membranous urethra. The bulbar urethra (BU) and especially the penile urethra(uP) are better evaluated in retrograde studies in which a better repletion is achieved. B: bladder
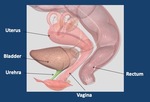
1.2 Female Urethra Anatomy ( Fig. 5 )
The female urethra is 2,5-4 cm long.
It forms an anterior concavity arch and extends from the bladder neck at the urethrovesical junction to the vestibule,
where it forms the external meatus between the labia minora and makes a relief called the urethral carina.
It is located between the symphysis and the anterior aspect of the vagina.
The paraurethral or Skene glands are located around the external meatus.
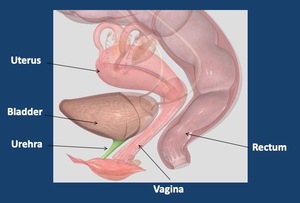
Fig. 5: Female urethral anatomy
Two parts are distinguished: the intramural and the intramembranous.
It is only explored by urinary voiding urethrography (Fig. 6).
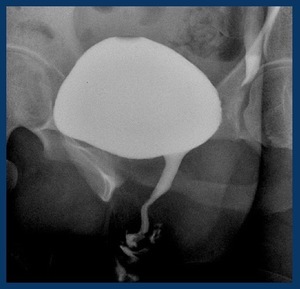
Fig. 6: 48 yo female: Voiding urethrogram
|
2.
Retrograde and voiding urethrocystography.
|
The objective of this technique is the study of the urethra and the bladder.
It begins with the retrograde study of the anterior urethra,
followed by the study of the bladder (cystography) and finally a voiding or anterograde urethrography (Fig. 7) is usually performed.
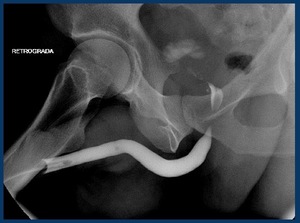
Fig. 7: Retrograde urethrogram
2.1 Indications:
| •Strictures |
| •Urethral injury |
| •Congenital abnormalities |
| •Fistulae or false passages |
| •Infections: periurethral/ prostatic abscess |
| •Diverticula |
2.2 Contraindications:
| •Acute Urinary Tract Infection |
| •Recent instrumentation |
| •Complete urethral obstruction |
2.3 Complications:
| •Due to contrast media: rare |
| •Due to technique: Acute UTI,
urethral trauma,
intravasation of contrast medium,
hematuria…. |
2.4 Preparation:
•No previous preparation is necessary.
•Occasionally,
a prophylactic antibiotic treatment is administered before the examination.
•Before going to the patient,
review clinical history to know the cause and circumstances that may condition the study.
•Verify the patient's identity.
•Explaining to the patient what the test consists of,
what will be done and the importance of his/her collaboration is essential to achieve good results.
• The informed consent of the test must be signed by the patient.
•The patient must undress by removing the underwear.
•Patient is asked to micturate prior to the examination.
2.5 After care.
•Patients should be advised of the possibility of dysuria or urine retention.
•In case of reflux or difficult catheterization: antibiotis are to be prescribed.
2.6 Equipment:
Tilting radiography table with fluoroscopy unit.
2.7 Contrast media:
•60% Iodinated contrast media 200-300 ml:
•HOCM (high-osmolar contrast media)
•LOCM (low-osmolar contrast media).
If the patient has severe urethral stenosis,
filling of periurethral vascular structures (intravasation) may occur during contrast injection,
so in these cases,
the use of non-ionic contrast may be advisable.
•Pre-warming the contrast media will help to reduce the spasm of the external sphincter.
2.8 Material:
•16 or 18 French Foley catheter or special tweezers for urethrography.
•Saline solution to dilute the contrast and to inflate the Foley’s catheter baloon
•Syringe
•Complete sterile field (cloths,
gauze,
and so on)
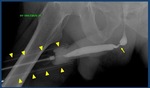
•Urological lubricant/ Some authors do not recommend lubrication because it may prevent the balloon from remaining in place for optimal occlusion ( Fig. 8 Fig. 9 )
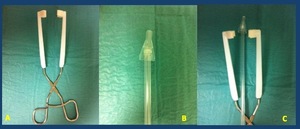
Fig. 8: Special tweezers for urethrography. A Tweezers with special end to pull the glans and stretch the penis. B Detail of the end of the probe that is inserted into the urethral meatus. C System as a whole.
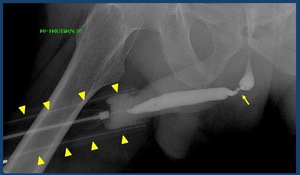
Fig. 9: Retrograde urethrogram performed with forceps (arrowheads) showing a stenosis in the bulbar urethra (arrow).
2.9 Technique
Preliminary film (Fig. 10):
Cone supine anteroposterior view,
with the center focused just below the pubic bone.
Sometimes an oblique view is also taken.
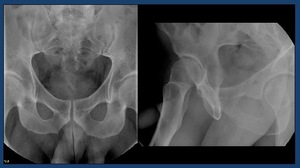
Fig. 10: Preliminary film: AP and oblique view
“Dynamic” urethrocystography represents a synergy of three imaging techniques:
a.
Retrograde urethrography
b.
Cystography
c.
Voiding urethrography

Fig. 11: Study protocol
Retrograde urethrography is the most appropriate way to evaluate the anterior urethra.
Voiding urethrocystography is the most appropriate way to evaluate the posterior urethra

Fig. 12: Retrograde and anterograde urethrography
A.
Retrograde urethrogram: Technique
•The patient is placed in a supine 30-45° right posterior oblique position,
with the right knee flexed and the left leg extended
•The penis should be placed laterally over the right proximal thigh with moderate traction.
•The glans and the external meatus are prepared in a sterile fashion.
•The 16-F or 18-F Foley catheter should be flushed with radiopaque contrast to remove any air bubbles.
•The tip of the Foley’s catheter is then inserted in the fossa navicularis of the penile urethra.
With the Foley in position, the catheter balloon is filled with 1-2 mL of radiopaque contrast or saline solution.
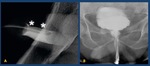
The patient should be reassured about the discomfort that is experienced during balloon inflation ( Fig. 13 ).
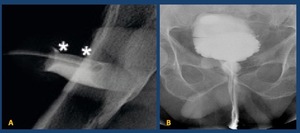
Fig. 13: A.- Retrograde urethrography: tip of the Foley’s catheter in the fossa navicularis (asterisc)
B.-Retrograde urethrography performed through a perineal meatus
•Pressure is applied over the glans penis to avoid expulsion of the catheter and the penis is straightened over the ipsilateral leg to prevent urethral overlap
•The catheter-tipped syringe is then filled with approximately 50 mL of radiopaque contrast,
and 20-30 mL of contrast is injected slowly in a retrograde fashion under fluoroscopic control.
•Static images of the urethra are taken during retrograde injection of radiopaque contrast.
PITFALLS:
•Cowper ducts and glands and Littrè glands may be opacified sometimes (not always) related to inflammation ( Fig. 14 )
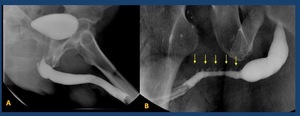
Fig. 14: A.- Opacified Cowper duct (arrow) B.- Opacified Littre Glands (arrows)
•Contrast reflux to seminal vesicles and vas deferens ( Fig. 15 )
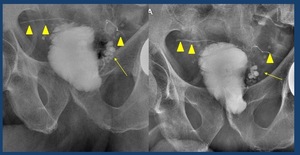
Fig. 15: Contrast reflux to seminal vesicles (arrows) and vas deferens (arrowheads)
•Contrast reflux to prostatic ducts ( Fig. 16 )
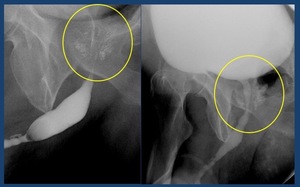
Fig. 16: Contrast reflux to prostatic ducts (circle)
•Intravasation.
Increased pressure causes mucosal disruption and contrast fills the corpora and veins ( Fig. 17 Fig. 18 )
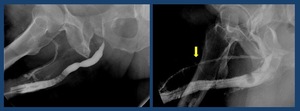
Fig. 17: Retrograde urethrography: Contrast intravasation. Contrast fills the dorsal vein of the penis (arrow)
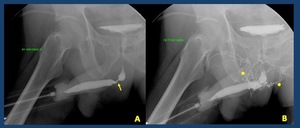
Fig. 18: Retrograde urethrography: Contrast intravasation. A. Patient with stenosis in the bulbar urethra (arrow). B. When the pressure to fill the bladder is increased against the stenosis there is a contrast intravasation (asterisks)
• Bad technique:
Filling defects: The probe has not been well purged and a bubble has been introduced causing a filling defect in the urethra ( Fig. 19 ).
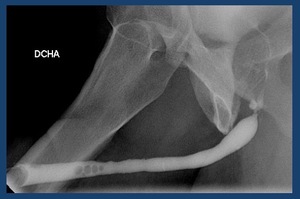
Fig. 19: Retrograde urethrography: bad technique. The probe has not been well purged and a bubble has been introduced causing a filling defect in the urethra (arrow).
Incorrect patient positioning.
Patient in oblique positioning and stretched penis are important to avoid missinterpretation ( Fig. 20 )
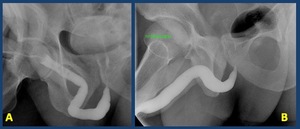
Fig. 20: Incorrect patient positioning . Patient in oblique positioning and stretched penis are important to avoid missinterpretation
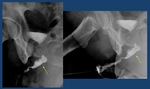
A Retrograde urethrography: bad technique. The penis has not been properly pulled so that the urethra appears angled which can mask a stenosis. B Proper penis positioning.
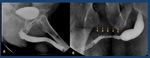
Retrograde urethrography: Pelvic trauma ( Fig. 21 )
•If a urethral injury is suspected in a polytraumatized patient,
it should not be probed.
It is very important when a catheter is in place not to remove it because of the danger of injuring the urethra or making a false path if it is probed again.
•In these cases,
the Urethrogram will be done with a small needle of polyethylene of 16 gauges (type moth) that is placed next to the Foley,
and pressure is made with the fingers on the glans to avoid reflux.
•Nor should complete catheterization be performed in patients with traumatisms and signs of urethral injury,
such as blood in the urethral meatus.
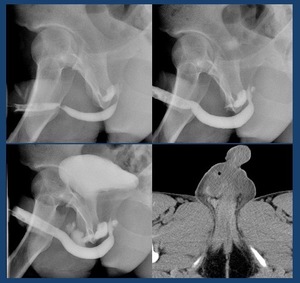
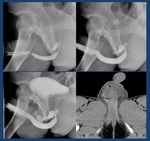
Fig. 21: RUG and CT show extravasation of contrast material from the posterior urethra; note that the extravasated contrast is located superior to the level of the urogenital diaphragm .
B.
Cystography: Technique
•After achieving an adequate filling of the bladder (250-350 mL),
anteroposterior projections,
right and left posterior oblique at 45 ° centered on the sagittal midline 5 cm above the symphysis pubis are performed.
•The Foley Catheter is then removed to continue the third phase of the scan (voiding urethrocystography).
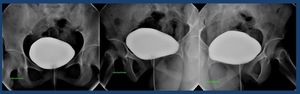
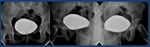
Fig. 22: Cystography
C.
Voiding (anterograde) urethrocystography: Technique (Fig. 23 ).
•It is usually performed after the bladder is filled with contrast material via a transurethral or suprapubic catheter.
•Voiding cystourethrography is the most frequently used imaging method in the evaluation of the female urethra and male posterior urethra.
•The patient voids under fluoroscopic observation and spot radiographs of the bladder and urethra are obtained.
•Voiding cystourethrography may not demonstrate certain abnormalities of the male anterior urethra because the normal anterior urethra is not fully distended to the degree seen at retrograde urethrography.
•When the patient does not get to urinate in the supine position,
it is usually useful to do the study while standing.
•Finally,
a post-void bladder film is done to assess the post-void residue.
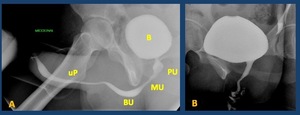
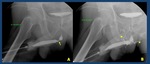
Fig. 23: A. Normal male voiding urethrography. The Anterograde urethrography. PU. Prostatic urethra with a normal central repletion defect ( veru montanum) . MU: membranous urethra. The bulbar urethra (BU) and especially the penile urethra (uP) are better evaluated in retrograde studies in which a better repletion is achieved.
B. Normal female voiding urethrography. .
1.- If during the examination the patient does not achieve urination or has an important post-void residue (urinary retention),
it may be necessary to insert a bladder catheter.
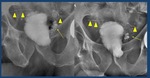
2.- If vesicoureteral reflux is detected at any time during the examination,
an abdominal x-ray will be done that includes the kidneys ( Fig. 24 ).
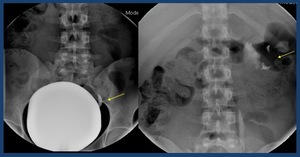
Fig. 24: Vesicoureteral reflux (arrows)
3.- In patients with severe urethral stricture or carriers of a suprapubic bladder catheter sometimes,
after the retrograde urethrography it is necessary to fill the bladder via suprapubic catheter and finally the voiding study is performed.
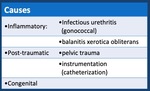
3.1 Urethral Stenosis/Stricture ( Fig. 25 Fig. 26 Fig. 27 )
The term urethral stricture refers to a fibrous scar in the urethra and periurethral tissue (corpus spongiosum).
This scar reduces the width of the urethral lumen.
There are two types of scars: Soft or hard.
Alternatively,
posterior urethral stricture is often an obliterative process that occurs as a result of urethral distraction or disruption caused by either trauma or surgery.
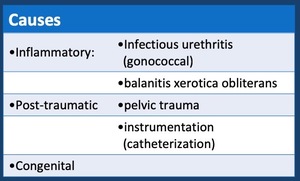
Table 1: Causes of urethral stenoses
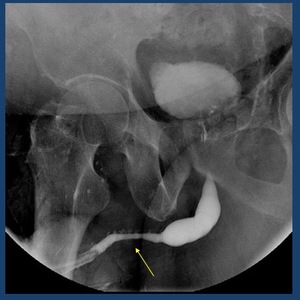
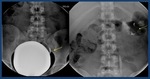
Fig. 25: Retrograde urethrogram depicts a long irregular stricture of the penile urethra with opacification of the Littrè glands
Diagnosis
Retrograde urethrography is the primary method used to image anterior urethral strictures and in posterior urethral strictures,
simultaneous antegrade cystourethrography and retrograde urethrography are often required to determine the length of the urethral defect
Retrograde and voiding urethrocystography define:
•location
•length
•number
•degree of strictures and
•periurethral disease
MR helps in depicting periurethral disease
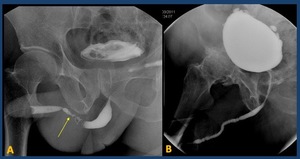
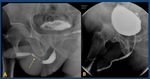
Fig. 26: A.- Retrograde urethrogram: segment of irregular narrowing of the proximal penile urethra. Bladder with irregular wall.
B.- Long irregular stricture of meatus and penile urethra.
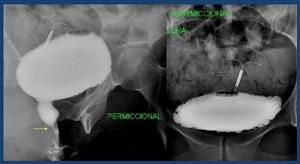
Fig. 27: Female Urethral stricture (arrow)
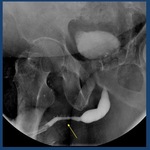
3.2 Infectious urethritis ( Fig. 28 )
Gonococcal urethritis
•First cause of sexual transmission infection in the adult
•Urethral purulent discharge
•Increased number of complications
No gonococcal urethritis
•Chlamydia trachomatis (50% cases)
• Scarce urethral discharge
Complications
•Stenosis
•Periurethral abscess
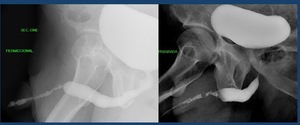
Fig. 28: Gonococcal urethritis. stricture of the penile urethra
3.3 Urethral diverticula ( Fig. 29 Fig. 30 Fig. 31 )
•More frequently in women than in men and are estimated to occur in 1-6% of women,
especially those with stress incontinence
•Usually between the 3rd and 5th decades but can affect all age groups.
•Clinical presentation: the "3Ds": dysuria,
post-void dribbling and dyspareunia.
•Other symptoms are: frequency/urgency,
recurrent urinary tract infection,
hematuria,
stress incontinence.
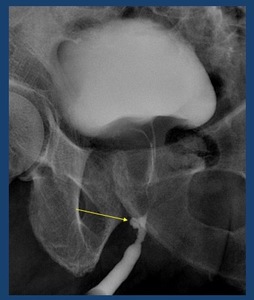
Fig. 29: 64 yo male. Urethral diverticulum (arrow)
Radiographic features:
•Voiding cystourethrography (VCUG) was traditionally considered the investigation of choice but the technique is sometimes equivocal and often additional imaging studies are necessary.
•Double-balloon catheter urethrography (DBU): a double-balloon 14 French Foley catheter is inserted into the urethra and contrast medium is injected at high pressure within the "isolated" urethra.
•US.
Well-marginated anechoic periurethral cystic lesions.
•CT.
NECT Low-attenuation periurethral lesion.
CECT Low-attenuation nonenhancing periurethral lesion.
Enhancing mass suggests associated tumor.
•MR.
Hyperintense periurethral cystic lesion on T2WI,
Hypointense on T1WI .
Although voiding cystourethrography is frequently used to evaluate urethral diverticula in women,
MR imaging is highly sensitive in the demonstration of these entities
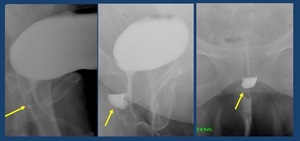
Fig. 30: 63 yo female. Voiding cystourethrogram shows contrast filling urethral diverticulum (arrows)
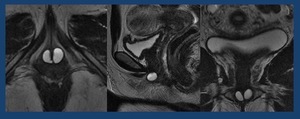
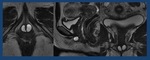
Fig. 31: 68 yo female. Multilocular Urethral diverticulum. Axial, sagittal and coronal T2W images (arrows)
3.4 Urethral fistulas ( Fig. 32 Fig. 33 )
•Rectourethral fistula is a connection between the lower urinary tract and the distal part of the rectum.
• They are rare conditions and can be classified as congenital or acquired.
• Acquired rectourethral fistula resulting from surgery,
radiation,
trauma,
or inflammation often occur in adults
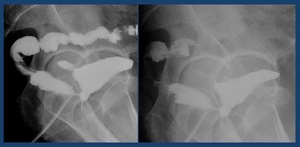
Fig. 32: Urethrorectal fistula in a patient undergoing prostatectomy
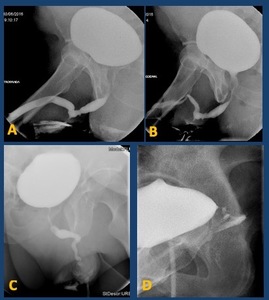
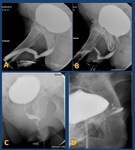
Fig. 33: A and B.- Urethroperineal fistula. C.- Glans fistula. D.- Vesicovaginal fistula
3.5 Urethral Calculi ( Fig. 34 )
•Most urethral calculi consist of small stones expelled from the bladder into the urethra during voiding.
•Rarely,
primary (native) formation of a stone occurs in the urethra when stricture is present,
or it may be associated with a urethral diverticulum.
• Retrograde urethrography will usually depict a round filling defect in the urethra.
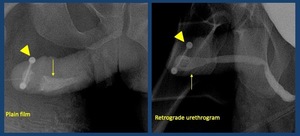
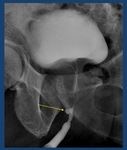
Fig. 34: Urethral Calculi in anterior urethra (arrow). Piercing (arrowhead)
3.6 Postsurgical changes ( Fig. 35 Fig. 36 Fig. 37 )
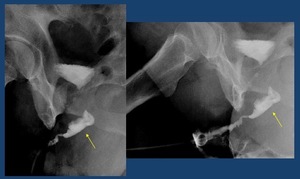
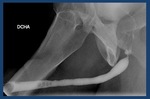
Fig. 35: Urethroplasty with oral mucosa of the bulbar urethra (arrow)
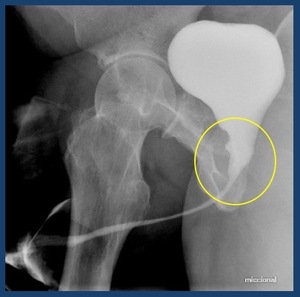
Fig. 36: Radical prostatectomy: cavity post-prostatectomy (circle)
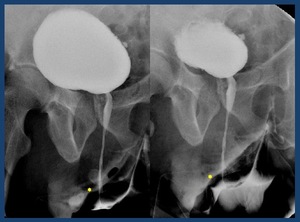
Fig. 37: Perineal Urethroplasty. Perineal meatus (*)