Patients present with symptoms of odontogenic abscess,
jaw and neck swelling,
elevation of the tongue,
and stridor.The most common presenting symptoms include neck swelling,
fever,
neck pain,
odynophagia,
and dysphagia.
People often describe the appearance as a "bull neck" and they may have "hot potato" voice-dysphonia what is suggestive to severe airway compromise.
At physical examination,
the submandibular tissues are firm and hard,
and crepitation may be present.
As soft-tissue swelling displaces the tongue into the pharyngeal airway,
the patient may experience difficulty breathing or stridor.
There is little clinical evidence of fluctuance and generally no drainable abscess.
If pus forms,
it is usually in deep,
localized pockets.
When untreated,
the infection may track along fascial
planes to involve the parapharyngeal and retropharyngeal spaces,
carotid sheath,
and rarely the mediastinum and subphrenic areas
Patients contrast-enhanced CT scan is used to evaluate the severity of the infection and airway obstruction.
Imaging is most helpful in demonstrating anatomic planes and defining a drainable abscess.
CT is performed also to evaluate mass effect on the airway,
gas-forming organisms and underlying dental disease.
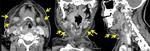
In the presence of Ludwig angina,
CT images show local skin thickening,
increased attenuation of subcutaneous fat,
muscle enlargement,
and loss of fat planes within the submandibular space.
CT images also may depict soft tissue emphysema and focal fluid collections within the fascial spaces of the neck.
(Fig.1,Fig.3,Fig.4.)
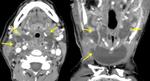
Complications of Ludwig's angina include mandibular osteomyelitis,
the spread of infection to the deep fascial spaces of the neck (Fig.3,Fig.4) and thrombophlebitis of the internal jugular vein (Lemierre syndrome) The most important complication is severe,
potentially fatal,
airway obstruction (Fig.3) since the tongue can rapidly become posteriorly displaced in this condition. Ludwig angina may be complicated by necrotizing fasciitis,
a rare soft tissue infection resulting in the death of subcutaneous and fascial tissue,
or it can expand inferiorly through the fascial planes to the superior mediastinum,
causing descending necrotizing mediastinitis.
Other complications include carotid sheath infection and arterial rupture,
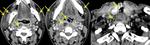
mediastinitis (Fig.2,Fig.3),
pericardial or pleural effusion (Fig.2),
empyema,
subphrenic abscess,
aspiration pneumonia,
cavernous sinus thrombosis and brain abscess.