Keywords:
Genital / Reproductive system female, Interventional vascular, Pelvis, Catheter arteriography, Percutaneous, Embolisation, Catheters, Efficacy studies, Outcomes
Authors:
T. D'hoore, A. Laenen, K. Op de beeck, D. Timmerman, G. Maleux; Leuven/BE
DOI:
10.26044/ecr2019/C-0844
Results
Treatment failure and symptom control
Time between intervention and follow-up ranges from 1.2 to 15.2 years with a mean follow-up period of 6.1 years.
Improvement of clinical symptoms was achieved in 72 out of 95 patients (75.79%),
based on the non-validated questionnaire.
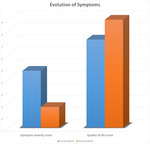
The mean pre-procedural symptom severity score was 47.15 [QR; 35.00-62.50] and 17,06 [QR; 7.5-22.5] after embolization.
This is a reduction in symptoms of 63,83% (p <0.0001).
The mean quality of life score before intervention was 73.05 [QR; 58.33-92.71] and 89.54 [QR; 83.33-100] after embolization,
which is an improvement of 23.29% (p <0.0001) (fig 3).
From 190 patients who underwent UAE,
18 (18.95%) patients had a second intervention,
defined as treatment failure,
at a median of 2,3 years (QR; 1.0 – 3.5 y) after initial UAE.
Kaplan-Meier analysis of freedom from TF showed a cumulative rate of 72.88% after 10 years and stable until the end of follow-up (fig4).
This is in accordance with the rates described in literature.
S.
Duvnjak et al reported 28% TF after 10 years [10].
C.
Scheurig-Muenkler et al reported in 2013 a TF of 23.3% after 7.7 year [11].
These findings support UAE as a good and cost-effective uterine sparing alternative for myomectomy [12].
Although the recurrence rate of myomectomy is lower than UAE,
it has more major complications [13,
14].
Better patient selection might improve outcome and reduce reinterventions
Outcome predictors
Cox regression models were used for univariate analyses of the association between patient characteristics and reintervention.
There was no relevant effect of age,
uterine location,
number of fibromas or preprocedural symptoms.
A pairwise test was only performed with significant global p-value,
which was found in evaluation of uterine volume (p < 0.0001) and volume of the dominant fibroma (p = 0.0003).
An increasing uterine volume is related to a higher risk for treatment failure.
The risk of TF is five times higher in women with a large uterus (>500ml) compared to women with a uterus < 200ml and 3 times higher compared to women with a uterine volume between 200 and 500ml (fig 5).
A fibroma volume of >200ml has a significant higher risk of TF,
as demonstrated in Kaplan-Meier analysis (fig 6).
Women with a large fibroma (>500ml) have 8.8 times higher risk compared to women with smaller fibroids (<200ml).
Our population includes a broad range of uterine volume [44.9ml – 3402ml] and dominant fibroid volume [2-1283.3ml] with accurate volume data because of the use of parallel planimetric measurements,
instead of the ellipsoid formula [7].
Volume calculations of fibroids in literature are almost always done by use of the ellipsoid formula and are therefore subjected to interobserver variability and possible poor correlation with gold standard volume measurements
Pregnancy after treatment
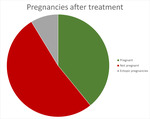
23 patients in our cohort expressed their desire to become pregnant after the procedure with a mean age of 32.61 years (ranging from 22 to 41y).
Nine patients (39.13%) became pregnant and had one or more children after the uterine embolization.
Two patients had an ectopic pregnancy and twelve patients did not get pregnant anymore (fig 7).
Five patients underwent the intervention primarily because of fertility dysfunction.
Four of them mentioned this as their only complaint.
One patient also had bleeding related symptoms.
Three (60%) women had successful pregnancies after the embolization in this group.