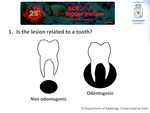
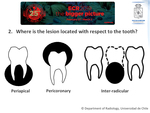
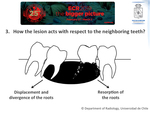
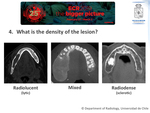
The basic radiological approach to mandibular / maxillary lesions should include 4 questions: 1) Is the lesion related to a tooth? (odontogenic v/s non-odontogenic); 2) Where is the lesion located with respect to the tooth? (periapical v/s pericoronary v/s inter-radicular); 3) How the lesion acts with respect to the neighboring teeth (displacement v/s resorption of the roots); 4) What is the density of the lesion? (radiolucent v/s mixed v/s radiodense).
These questions are outlined in Fig. 2,
Fig. 3,
Fig. 4 and Fig. 5.
To this 4 basic questions other features can be added to help in the differential diagnosis: single v/s multiple,
focal v/s diffuse,
unilocular v/s multilocular,
well v/s ill defined borders,
destruction v/s expansion of the bone cortex,
presence of periosteal reaction,
location (mandibullary v/s maxillary,
anterior v/s posterior).
The main odontogenic lesions may be grouped into the following categories:
- Radiolucent cystic: periapical or radicular cyst,
dentigerous or follicular cyst,
odontogenic keratocystic tumor.
- Radiolucent solid: ameloblastoma,
odontogenic myxoma.
- Radiodense: odontoma,
cementoblastoma or true cementoma,
cemento-osseous dysplasia.
Radiolucent cystic lesions:
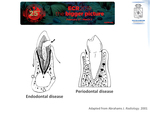
Endodontal disease:
- Infection from caries,
with entrance to the pulp chamber and extension down by the root canal to the apical foramen,
leading to an apical periodontitis with bone resorption.
- Formation of an abscess (acute form) or a granuloma (chronic form).
After that the disease evolves to a periapical or radicular cyst (latent form,
the most frequent odontogenic cyst).
- Imaging ⇒
- Radiolucent lesion surrounding the root apex,
usually <1 cm.
- Small lesions may present just as radiolucent crescent shaped areas surrounding the root apex.
- On axial images periapical cysts usually present a “target” appearance (radiodense root apex in the center of the radiolucent lesion).
- Condensans osteitis surrounding the cyst is a common finding (sclerosis due to bone reaction to the inflammatory process).
- The presence of sclerotic border and the density of the lesion are not useful criteria to differentiate between periapical granuloma and cyst.
Periodontal disease:
- Initial infection as gingivitis,
with extension through the periodontal ligament,
forming a periodontal sac.
- Imaging ⇒
- Radiolucent area extending down by the side of the root (periodontal pocket),
variable in extent (it may reach the root apex).
- It may present condensans osteitis surrounding the cyst (sclerosis due to bone reaction to the inflammatory process).
Both diseases – endodontal and periodontal – may coexist in the same dental element ⇒ endo-periodontal lesions.
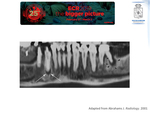
Endodontal and periodontal disease are schematized in Fig. 6 and presented on a CT exam in Fig. 7.
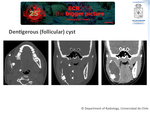
Dentigerous (follicular) cyst:
- The second most frequent odontogenic cyst.
- Pericoronary location (usually in relation to a third molar).
- Corresponds to fluid accumulated between the two sheets of enamel epithelium (developmental cyst).
- Imaging ⇒
- Pericoronary radiolucent lesion with walls that converge at an acute angle in the cemento-enamel junction.
- Variable size,
it can expand the bone and displace teeth.
A dentigerous cyst presented on a CT exam is shown in Fig. 8.
Keratocystic odontogenic tumor (odontogenic keratocyst):
- 5-15% of mandibular / maxillary cysts,
with peak incidence between the 2nd and 3rd decade.
- It develops from the dental lamina (odontogenic epithelium),
so it grows in the support areas of the teeth.
- Twice frequent in the mandible than in the maxillary bone.
- Locally aggressive lesion,
it can present recurrence.
- The presence of multiple odontogenic keratocysts is characteristic of the Basal Cell Nevus Syndrome (Gorlin-Goltz).
- Imaging ⇒
- Radiolucent lesion that can be loculated,
smooth or lobed.
- Usually located in the mandibular ramus or body.
- It can expand and even erode the cortical bone.
- It can displace the dental roots,
but it does not erode them.
- In CT the density is higher than that of water,
due to the presence of keratinized material.
- In MRI the signal is high on T1 (by proteinaceous content) and high on T2.
Radiolucent solid lesions:
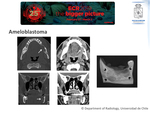
Ameloblastoma:
- Primary odontogenic tumor,
derived from enamel-forming embryonic cells,
whose regression fails during development.
- Peak of incidence in the 3rd and 4th decade.
- Is the second odontogenic tumor in frequency after the odontoma.
- More frequent in the mandible than in the maxillary bone.
- 5% of the cases originate from the epithelium of a dentigerous cyst.
- Is a benign tumor,
but locally aggressive.
- There are multiple subtypes,
most of them indistinguishable on imaging studies.
- There are some ameloblastoma forms with malignant behavior: ameloblastic carcinoma (with a frankly malignant histology) and malignant ameloblastoma (with presence of metastases,
despite a well-differentiated histology).
- Imaging ⇒
- Expansive radiolucent lesion.
- Located more frequently posterior in the mandible.
- Uni or multiloculated,
with a "soap bubbles" appearance.
- The loss of the lamina dura (compact bone that lies adjacent to the periodontal ligament in the tooth socket) and the erosion of the adjacent dental roots are characteristic findings,
which reflect an aggressive local behavior.
- It has tendency to destruct the cortical bone and extent to the soft tissues.
- The presence of a large solid component with enhancement,
intralesional papillary projections and extra bony extension should lead to suspicion of malignant behavior.
- MRI is the better examination for demonstrating intralesional solid component with enhancement and the extra bony soft tissue extension.
An ameloblastoma presented on a CT exam and the radiographic examination of its surgical specimen are shown in Fig. 9.
Odontogenic myxoma:
- Uncommon tumor,
which occurs in the 2nd - 3rd decade.
- Clinically and radiologically indistinguishable from an ameloblastoma.
- It presents as a multiloculated radiolucent lesion,
with internal bony trabeculae.
- Histologically benign,
but locally aggressive.
Radiodense lesions:
Odontoma:
- Most frequent odontogenic tumor.
- Usually occurs in the 2nd - 3rd decade.
- It is a benign tumor,
even considered as an odontogenic hamartoma.
- The presence of enamel inside the lesion can be considered virtually pathognomonic of an odontoma.
- Half of the cases occur in relation to an unerupted tooth.
- It is encapsulated,
and therefore easily enucleable.
- 3 types ⇒
- Simple odontoma: supernumerary teeth or denticles.
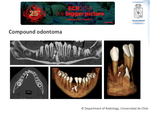
- Compound odontoma: most common type of odontoma,
more frequent in the mandible than in the maxillary bone.
Organized structured tissue,
being able to distinguish the components of a tooth.
Imaging: multiple small and well-defined malformed or rudimentary teeth.
- Complex odontoma: 24% of the odontomas,
more frequent in the posterior mandible.
Disorganized dental tissue,
which does not mimic a normal or rudimentary tooth.
Imaging: circumscribed radiopaque mass,
with amorphous calcifications,
often in relation to the crown of an unerupted tooth.
A compound odontoma presented on a CT exam is shown in Fig. 10.
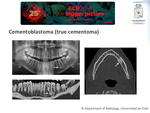
Cementoblastoma (true cementoma):
- It is a rare benign tumor (<1% of odontogenic tumors),
which occurs in the 2nd - 3rd decade.
- Typically located in the molar - premolar region of the mandible.
- Initially it is a radiolucent lesion,
but it become radiopaque as cement is deposited.
- Imaging ⇒
- Radiodense periapical lesion with a fine radiolucent halo.
- Attached to the root of a tooth.
- It can expand the cortical bone.
A cementoblastoma presented on a panoramic dental radiography and CT is shown in Fig. 11.
Cemento-osseous dysplasia:
- Hamartomatous lesion located in relation to the radicular apex,
due to proliferation of connective tissue in the periodontal membrane.
- Also known as cemental or periapical bone dysplasia.
- More frequent in women,
in the 4th - 5th decade.
- 3 types ⇒
- Periapical cemento-osseous dysplasia: more frequent in African descendants.
Localized mostly in the anterior mandible,
affecting one or a few teeth.
- Focal cement-osseous dysplasia: more frequent in Caucasians descendants.
Located in the posterior mandible,
affecting molars.
- Florid cemento-osseous dysplasia: more frequent in African descendants.
Affects two or more dental quadrants.
- Imaging ⇒
- Periapical location.
- Initially it is a radiolucent lesion.
It progressively calcifies,
starting from its central portion.
Subsequently,
it becomes a well-defined sclerotic lesion with a radiolucent halo.
- It does not fuse with the dental root.
The lamina dura and the periodontal ligament are intact.