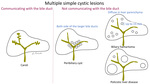
Simple hepatic cystic lesions
appear as round or ovoid fluid-containing lesions with smooth imperceptible well-defined walls and no evidence of complex internal features,
such as septations,
mural irregularity,
nodularity or wall calcification.
No enhancement is seen after intravenous contrast media administration (Fig3).
Imaging features
On ultrasound,
a hepatic cyst appears as a well-circumscribed anechoic lesion with posterior acoustic enhancement.
On CT: homogeneous hypoattenuation (water attenuation around 0-10 HU).
In fatty livers simple cyst can appear iso- or hyperattenuating compared to hepatic parenchyma on precontrast images.
In such cases density measurement can be helpful for making the correct diagnosis.
On MRI,
hepatic cysts are homogeneously hypointense on T1-weighted imaging and homogeneously hyperintense on T2-weighted imaging.
The increase in signal intensity due to fluid content on heavily T2-weighted imaging (long TE,
>80 ms) helps differentiate simple hepatic cysts from solid tumors,
which appear less intense on these sequences.
Shorter TE (40-60 ms) is helpful to differentiate simple cyst from other complex cystic lesions (e.g.
hemangiomas): simple cyst will show intermediate signal intensity similar to cerebrospinal fluid,
while others complex cystic lesions will present higher signal intensity.
Simple,
non-complicated hepatic cysts usually show a low to isointense signal intensity on high b-value DWI performed on 1.5T MR scanners. When 3T scanners are used their signal intensity may be high,
as a result of the contribution of T2 hyper-intensity to the overall signal intensity on DWI scans (T2 shine-through effect).
To confirm true restricted diffusion,
one should always compare the DWI image to the ADC: in cases of true restricted diffusion,
the region of increased DWI signal will demonstrate low signal on ADC.
Differential diagnosis (Fig4,
Fig5 and Fig6).
-
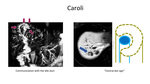
Saccular cysts up to 5 cm in diameter in communication with the major bile ducts are typical for Caroli disease.
Another finding highly suggestive of Caroli disease is the “central dot sign,” in which tiny foci of strong contrast enhancement within dilated intrahepatic bile ducts correspond to intraluminal portal vein radicals (Fig7).
Complex hepatic cystic lesions
Complex cysts are defined by the presence of complex features within a cystic lesion.
In patients with complex hepatic cyst the pretest probability of a diagnosis is highly affected by the patient's comorbidities,
clinical and laboratory data.
Thus,
imaging studies should always be interpreted in the context of the other clinical information of the patient (Fig12).
Otherwise healthy patients (Fig13).
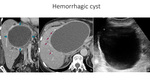
The principal challenge is to differentiate simple hepatic cyst complicated by intracystic hemorrhage from cystic neoplasms – i.e.
biliary cystadenoma or cistadenocarcinoma (Fig14).
Indeed,
multiple septa,
vegetations and thickened cyst wall may be present on both entities.
Hyperintensity on T1-weighted sequences – due to hemorrhagic content – and a liquid-liquid level are more frequently observed on hemorrhagic cysts.
US imaging plays an important role in achieving a correct diagnosis of hemorrhagic cyst when it demonstrates the mobility of the septa.
Besides enhancement of thick septa,
mural nodules or thickened wall are typically found in malignant lesions.
Moreover,
checking previous imaging,
when available,
may facilitate the diagnosis (Fig15).
After intravenous administration of contrast material,
the typical early,
peripheral,
nodular discontinuous enhancement is always observed in hemangiomas and usually allows non-invasive diagnosis.
However,
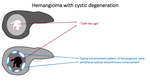
in giant hemangiomas,
the progressive centripetal enhancement of the lesion,
although present,
does not lead to complete filling even on delayed phases.
On MR images giant hemangiomas may show a central cleft-like area of low intensity on T1-weighted images and of higher intensity on heavily T2-weighted images.
This area remains hypointense after contrast administration (Fig16).
The central cleft-like area may be due to cystic degeneration or liquefaction.
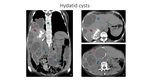
Key imaging features for diagnosis of hepatic hydatid cysts are: mural calcifications (observed in about half of patients),
daughter cysts (round peripheral structures within the mother cyst),
“water lily” sign (detachment of the endocyst membrane which results in floating membranes within the pericyst) (Fig17 and Fig18).
In the absence of daughter cysts,
it may be difficult to differentiate an echinococcal cyst from a cystic metastasis or a pyogenic abscess on imaging.
However,
hydatid cysts almost never show contrast enhancement,
reflecting the poor vascularity of the parasitic lesion.
Ciliated Hepatic Foregut Duplication Cyst
Solitary subcapsular congenital lesion that typically measures less than 3 cm,
and is commonly located in the segment IV.
A ciliated hepatic foregut duplication cyst has many similarities with a bronchogenic cyst (i.e.
it is lined by ciliated pseudostratified columnar epithelium).
Given the reported risk of malignant transformation,
ciliated hepatic foregut duplication cysts should be resected.
Patients with comorbidities
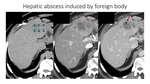
Hepatic abscess
usually appears on imaging as a well-defined,
low attenuation,
round mass with an enhancing peripheral rim after contrast media administration.
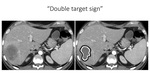
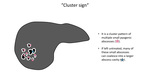
The "double target sign” (Fig19) and the "cluster sign" (Fig20) are characteristic radiologic signs of hepatic abscess seen on contrast-enhanced CT images.
A transient,
early,
wedge-shaped or circumferential segmental region of hepatic hyperenhancement at dynamic CT and MR imaging,
which equilibrates in late phases,
has also been reported to be associated with hepatic abscesses (Fig21).
Gas may be present in up to 20% of liver abscesses,
but it is not a specific sign.
Hepatic extrapancreatic pseudocyst
is an abnormal collection of pancreatic fluid generally due to pancreatitis and is usually symptomatic (i.e.
abdominal pain).
Hepatic pseudocysts occur predominantly in the left lobe of the liver and are secondary to an extension of fluid from the lesser sac into the hepatogastric ligament.
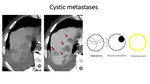
Cystic metastases
Compared with other benign complex cystic lesions,
cystic metastasis has thick,
irregular septa and mural nodules that represent viable tumor.
The attenuation of the cystic component is usually higher than that of pure fluid because of the presence of necrosis,
mucin or hemorrhage (Fig22).
However,
distinguishing solitary cystic metastases from other malignant cystic neoplasms without knowledge of their primary malignancy can be problematic because the imaging findings are usually unspecific.
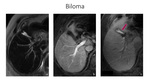
The collection of bile,
lymph,
or blood products after injury to the liver parenchyma will result in the formation of a biloma (Fig23),
seroma,
or hematoma,
respectively.
These lesions may occur after blunt or penetrating trauma or iatrogenic injury to the liver,
such as after cholecystectomy,
liver surgery,
liver transplantation,
or percutaneous liver procedures.
On imaging,
bilomas appear as a simple fluid collection that may or may not show a thin rim of enhancement (i.e.,
a pseudocapsule).
Superinfection results in a complex cystic appearance.
Cystic hepatocellular carcinoma (rare)
Very rarely hepatocellular carcinoma (HCC) can have a cystic component,
due to necrosis and cystic degeneration in rapidly growing tumors or after treatment.