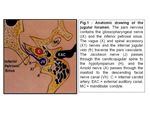
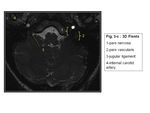
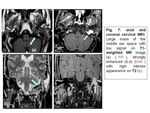
I- Normal anatomy:
The jugular foramen,
sometimes referred to as the posterior foramen lacerum, is a depression on the medial and inferior surface of the petrous pyramid,
formed by the temporal and occipital bones.
The jugular foramen courses anteriorly and laterally as it exits the skull base and consists of a smaller anteromedial portion (pars nervosa) and a larger posterolateral portion (pars vascularis) that are separated by a complete or incomplete fibrous or bony septum.
The pars nervosa contains the glossopharyngeal nerve (cranial nerve IX) and the inferior petrosal sinus as it courses between the cavernous sinus and jugular bulb.
The pars vascularis contains the internal jugular vein,
the vagus nerve (cranial nerve X),
and the spinal accessory nerve (cranial nerve Xl).
The cranial nerves are medial to the jugular vein.
Small dehiscences within the jugular fossa wall allow the passage of the tympanic branch of the glossopharyngeal nerve (Jacobson nerve) and the auricular branch of the vagus nerve (Arnold nerve).
This nomenclature can be somewhat misleading,
because both structures contain neural as well as vascular structures (Fig.
1,2-a,2-b,2-c,3-a,3-b,3-c).
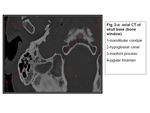
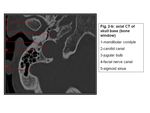
The jugular foramen is separated from the hypotympanum by a bony plate and is medial to the descending facial canal and inferomedial to the posterior semicircular canal (1,2) . The jugular foramen is separated from the anteromedial carotid canal by the caroticojugular spine and from the inferomedial hypoglossal canal by the jugular tubercle. The sigmoid sinus courses anteriorly into the jugular bulb (2).
The jugular foramen varies greatly in size but averages 1.5 cm in length and 1 cm in width (1).
In two-thirds of cases,
the right jugular foramen is larger than the left jugular foramen (2).
II- Pathologic entities:
A variety of lesions may occur in the jugular foramen.
These lesions may arise primarily in the jugular foramen or extend into the jugular foramen from adjacent structures such as the hypoglossal canal,
petro-occipital fissure,
clivus,
mastoid,
and endolymphatic sac; in other words,
either intrinsically or extrinsically.
Furthermore,
these lesions may have typical clinical manifestations and imaging characteristics that allow differentiation.
1- Tumoral lesions:
- Paraganglioma:
The most common tumor to develop in the JF is a paraganglioma.
Paragangliomas are tumors of the chemoreceptor system and account for approximately 60-80% of primary tumors of the jugular foramen (3).
These neoplasms are also called chemodectomas and glomus jugular tumors (4).
Glomus jugular tumors of the temporal bone originate from paraganglionic tissue in the adventitia of the jugular vein or along the Arnold and Jacobson nerves (4,5,6,7).
The majority of paragangliornas proves benign at histologic examination but is locally aggressive.
Malignant degeneration with metastasis occurs in approximately 4% of cases (4).
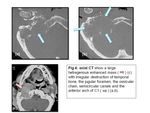
At contrast-enhanced CT,
paragangliomas manifest as areas of irregular,
lytic bone destruction of the jugular foramen with significant enhancement (4,7) (Fig.
4).
These tumors tend to extend in predictable patterns along pathways of least resistance,
frequently below the skull base,
into the mastoid air cells,
and into the hypotympanum,
eroding the jugular plate.
Erosion of the caroticojugular spine and encroachment on the carotid artery may be seen (6).
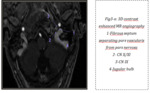
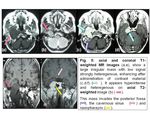
Paragangliomas have low signal intensity on T1-weighted MR images and enhance strongly after administration of contrast material,
which is indicative of hypervascularity.
They appear hyperintense on T2-weighted MR images.
Glomus jugular tumors give an MR appearance known as the “salt-and-pepper” pattern on long TR–long TE images.
The “pepper” component is caused by multiple areas of signal void,
interspersed with the “salt” component,
which is caused by hyperintense foci produced by slow flow or subacute hemorrhage on both long TR and short TR images (Fig.
5).
This appearance,
usually seen in tumors larger than 1 cm,
is highly suggestive of a glomus tumor but can also be seen in other hypervascular lesions,
such as metastatic hypernephroma and metastatic thyroid carcinoma.
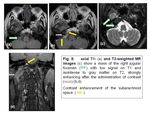
- Schwannoma:
Schwannomas are the second largest group of tumors at the jugular foramen . Ninety percent of jugular foramen schwannomas originate from cranial nerve IX or X. Samii et al.(8) classified these tumors into four subtypes based on location.
Type A tumors are those that primarily occupy the cerebellopontine angle with minimal enlargement of the jugular foramen.
Type B tumors are primarily located in the jugular foramen with intracranial extension.
Type C consists of primarily extracranial tumors with extension into the jugular foramen.
Type D consists of dumbbell-shaped tumors with both intra- and extracranial components.
Schwannomas are smooth,
encapsulated,
lobulated tumors composed of spindle-shaped neoplastic Schwann cells.
Schwannomas cause smooth,
well-demarcated enlargement of the jugular foramen (4).
As the tumor extends out of the foramen,
it may assume a dumbbell shape (7).
Calcification or hemorrhage is uncommon (4),
but cystic or fatty degeneration are frequent (4).
Schwannomas characteristically enhance strongly on contrast-enhanced CT and MR images without flow void.
Most schwannomas appear hypointense or isointense relative to gray matter on T1 weighted MR images and hyperintense relative to gray matter on T2-weighted MR images (Fig.6,7).
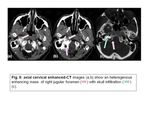
- Meningioma:
Meningiomas develop from the leptomeninges.
They are defined as primary when centered in the JF (intrinsic lesions) and secondary when centered in the posterior fossa with extension into the JF (9,10).
Primary meningiomas of the JF are characterized by an invasive growth pattern with extensive skull base infiltration (9,11).
Meningiomas characteristically appear iso-intense to gray matter on both T1 and T2- weighted MR images,
but this appearance is variable (1) (Fig.
8).
Nearly all meningiomas enhance strongly with contrast material on both CT and MR images (Fig.
9).
The dural component may be prominent (1).
A reliable imaging feature of meningiomas is partial calcification and infiltration of the diploic spaces within the skull base.
This gives rise to characteristic hyperostosis,
which has a distinctive appearance compared with the bone destruction caused by paragangliomas and scalloping of the foramen by neural sheath tumors.
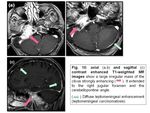
- Metastasis:
Metastasis —usually from primary tumors in the lung,
breast,
and prostate—are aggressive lesions.
Clinical onset of symptoms is often more rapid than with paraganglioma,
schwannoma,
or meningioma (1).
At CT,
metastases manifest as areas of permeative destruction of the temporal bone irrespective of the predictable route of extension of paragangliomas (7).
Vascular metastases such as those from renal and thyroid carcinoma may be indistinguishable from paraganglioma at cross-sectional imaging (Fig.
10) and angiography (4).
-Plasmocytoma:
Plasmacytomas are tumors resulting from neoplastic proliferation of a single clone of plasma cells with monoclonal immunoglobulin production.
A diagnosis of plasmacytoma is made when a single lesion is found and bone marrow examination shows less than 5% plasma cells.
Solitary plasmacytoma most commonly occurs in the spine and pelvis.
Although diffuse skull involvement is common in multiple myeloma,
solitary plasmacytoma of the skull is rare.
Most patients eventually develop multiple myeloma (1).
Plasmacytomas appear as non specific destructive enhancing lesions at radiography. The tumors often have intermediate signal intensity on both T1 and T2 weighted MR images (12).
-Chondrosarcoma:
Chondrosarcomas of the skull base arise from embryonal rests and characteristically arise from the petro-sphenoidal or petro-occipital fissures.
They are usually extradural and have a peak age of presentation between 20 and 40 years.
They may extend posterolaterally to involve the jugular foramen at its medial aspect.
At CT,
chondrosarcoma manifests as a soft-tissue mass with lyric infiltrative bone destruction (4,13).
Matrix calcification in ring- and arc-shaped patterns,
typical of chondroid matrix,
is seen in half of all cases (13).
Chondrosarcomas usually have low to intermediate signal intensity on T1 weighted MR images and heterogeneous hyperintensity on T2 weighted MR images.
On images obtained with contrast material,
mild to moderate inhomogeneous enhancement is typical (4,13).
- Lymphoma:
Involvement of the head and neck by lymphoma may be either primary or metastatic.
The radiographic appearance of lymphoma is nonspecific,
consisting of areas of ill-defined,
permeative destruction.
Lymphorna often has relatively low signal intensity on T2 weighted MR images due to its high cellularity (5).
- Langerbans Cell Histiocytosis:
Langerhans cell histiocytosis is characterized by idiopathic proliferation of the Langerhans cell,
a specific type of histiocyte that specializes in antigen presentation to T lymphocytes.
Langerhans cell histiocytosis of bones characteristically manifests as a well-defined lytic lesion with nonsclerotic margins.
However,
its appearance may be more aggressive,
with areas of permeative irregular destruction simulating infection or a malignant tumor (14).
Langerhans cell histiocytosis typically appears hyperintense on T2-weighted MR images and enhances strongly after administration of contrast material (14).
2- Vascular lesions:
Vascular variants,
such as asymmetric jugular bulbs or a high jugular bulb,
may cause enlargement of the jugular foramen and an apparent mass (pseudo-mass).
In all of these lesions,
the margins of the jugular foramen are smooth and intact.
CT findings include smooth,
rounded enlargement of the pars vascularis,
large ipsilateral and small controlateral transverse and sigmoid sinuses (1,7).
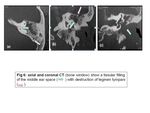
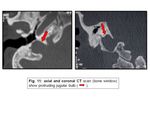
- Protruding jugular bulb:
At CT,
a protruding jugular bulb appears as a middle ear soft-tissue mass contiguous with the jugular vein through a dehiscent jugular plate (Fig.
11).
Turbulent or slow flow in a high or protruding bulb can result in loss of the flow void and contrast enhancement at MR imaging,
thereby mimicking real disease.
Use of flow-sensitive techniques or MR angiography will help clarify confusing cases.
It is imperative that vascular variants be recognized leading to unnecessary complications (1).
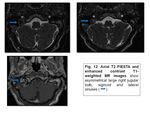
- Asymmetrically enlarged jugular foramen:
The size of the jugular bulbs is variable,
with the right side being significantly larger than the left in two thirds of people.
Its only significance is to distinguish it from pathology,
as it is entirely normal and asymptomatic.
A normal but large bulb will have an intact jugular spine,
normal bony margins and have proportionately large ipsilateral internal jugular vein and sigmoid sinus.
Its dome will not extend above the floor of the internal acoustic meatus (IAM),
thus distinguishing it from a high riding jugular bulb (Fig.
12).
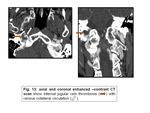
- Jugular thrombosis:
Cerebral venous thrombosis has many predisposing causes,
and the symptoms and signs are often nonspecific (13,15).
Non enhanced CT may show high-attenuation clot ("cord sign"),
and contrast-enhanced CT may show non-enhancing thrombus with marginal enhancement from meningeal collateral vessels ("empty delta sign") (Fig.
13).
Conventional MR imaging shows replacement of the flow void by thrombus (13,15,16).
The appearance of the thrombus varies with the age of the clot.
Acute clot appears isointense and sub-acute clot appears hyperintense relative to gray matter on T1- weighted MR images.
Flow-related enhancement and in plane,
turbulent,
or slow flow can cause loss of the flow void and thus mimic thrombosis (13,16).
Gradient-refocused images will show loss of the normal high signal intensity in the dural sinus with cerebral venous thrombosis (13).
Cerebral venous thrombosis can easily be diagnosed with MR venography.
Both twodimensional time-of-flight and phase contrast MR venography are frequently used.
When maximum intensity projection is used to produce the images from data obtained with time-of-flight MR venography,
hyperintense subacute clot may be mistaken for flow.
Furthermore,
this technique is less sensitive for slow-flowing venous blood.
Consequently,
phase-contrast MR venography is the preferred imaging modality in the assessment of cerebral venous thrombosis.
Angiography shows absence of filling or a filling defect (13,16).
3- Infectious lesions:
Infection may spread to the jugular foramen from contiguous structures such as the middle ear cavity,
mastoid air cells,
or external auditory canal.
Intracranial complications from otologic infections include meningitis,
epidural abscess,
brain abscess,
and dural sinus thrombosis.
These complications have been reduced significantly with liberal use of antibiotics (16).