Technique:
Patient position: the patient should be lying in supine position,
with his head and shoulders on a pillow.
Four acoustic windows for TDCS:
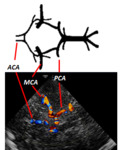
TEMPORAL WINDOW:
The transducer is placed parallel to and just above the zygomatic arch.
At this level the butterfly-shape of the midbrain will be located in the middle of the screen.
We can identify the M1 and M2 segments of the MCA,
A1 segment of the ACA,
P1 and P2 segments of the PCA,
C1 segment of the carotid siphon,
the anterior and posterior communicating arteries and the distal end of the BA.
[Fig.
1]
10–20% of patients have inadequate transtemporal acoustic windows depending on many factors affecting the temporal bone thickness.
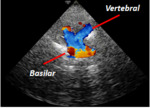
OCCIPITAL WINDOW:
The patient should be lying on the side with the chin lowered toward the shoulder.
The transducer must be positioned on the median suboccipital line.
With US beam passing through the foramen magnum.
We can visualize the intracranial segment of the two vertebral arteries (VA) and the basilar trunk.
[Fig.2]
ORBITAL WINDOW:
The transducer is placed over the closed eyelid,
and looking on the opposite side respect to the probe.
This allows the evaluation of the ophthalmic artery and the C2,
C3,
and C4 segments of the carotid siphon through the foramen of the ocular cavity.
It is recommended to reduce power of the device 10–15% respect to transtemporal scan to avoid possible injuries to the retina.
SUBMANDIBULAR WINDOW:
This approach is utilized in cases of limited evaluation through the other windows.
Most of the ICA flow passes through the MCA.
Therefore,
its assessment represents the blood flow to a hemisphere
MCA is identified at 45–60 mm of depth,
and the blood flows toward the transducer.
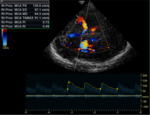
TRANSCRANIAL DOPPLER INDICES:
Other clinically important parameters measured with TCD examination include: Mean CBFV, pulsatility index (PI),
resistivity index (RI) and the Lindegaard ratio (LR) .
Mean CBFV
Mean CBFV is calculated by the formula
(PSV + [EDV × 2])/3
PSV is peak systolic velocity,
and end diastolic velocity (EDV) is end-diastolic blood flow velocity .
It is important to know that the CBFV in an artery is inversely related to the diameter of the same artery.
Hence,
the analysis of blood flow velocity indirectly assess the diameter of intracranial vessels.
In other words,
when mean CBFV is increased,
it suggests stenosis or VSP.
On the other hand,
a lowered value indicates hypotension,
raised ICP,
or brain stem death.
[fig.3]
PI and RI:
They point an estimation of downstream resistance in cerebral circulation.[fig.3]
PI is calculated as:
PI = (PSV − EDV)/mean CBFV
Reference range is between 0.5 and 1.19.
In cases of proximal stenosis or occlusion,
the PI may be lower than 0.5 because of distal arteriolar vasodilation; instead,
a distal occlusion or constriction shall increase the PI above 1.19 due to high distal resistance.
PI is directly related with ICP.
Also,
a significant correlation between the cerebral perfusion pressure (CPP) and PI is present.
The RI is calculated as:
RI = (PSV − EDV)/PSV
A RI value above 0.8 indicates increased distal resistance.
LR:
It allows differentiation between hyperdynamic flow and VSP.
It is calculated as:
LR = MCA mean CBFV/extracranial ICA mean CBFV
Normal reference range is from 1.1 to 2.3.
This ratio directly related to the severity of VSP.
When the CBFV is elevated while the LR ratio is less than 3,
it is considered to be due to hyperemia.
In case of a ratio more than 6,
it indicates severe VSP.
MCA mean CBFV/extracranial ICA mean CBFV >3 mild to moderate VSP
MCA mean CBFV/extracranial ICA mean CBFV >6 severe VSP.
SICKLE-CELL DISEASE AND ISCHEMIC STROKE:
In cases of sickle cell disease semestral TCD is done to calculate the time averaged mean maximum CBFV.
In asymptomatic children,
patients with a time averaged mean maximum CBFV in all arteries of <170 cm/s are considered normal.
CBFV >200 cm/s is related to an increased risk of stroke.
Therefore,
blood transfusion is indicated to lower pathologic sickle hemoglobin to <30% of total hemoglobin to decrease the risk of stroke.