Keywords:
Neuroradiology brain, Oncology, CNS, MR-Diffusion/Perfusion, MR, Diagnostic procedure, Imaging sequences, Observer performance, Cancer, Multidisciplinary cancer care
Authors:
S. Türk1, J. Kim2, R. Lobo3, J. Bapuraj3, T. Ma3, T. Johnson3, S. Camelo Piragua3, L. R. Junck3, A. Srinivasan3; 1Izmir/TR, 2Ann Arbor/US, 3Ann Arbor, MI/US
DOI:
10.26044/ecr2019/C-0958
Aims and objectives
In a proportion of patients,
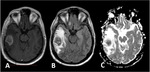
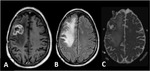
the combination of chemotherapy and radiation provokes increased contrast agent uptake and apparent enlargement of the treated tumor; or the appearance of new lesions mimicking tumor progression.
This phenomenon,
referred to as pseudoprogression,
has become a major challenge in the follow-up of high-grade glioma undergoing treatment,
as only repeat biopsy is conclusive in differentiating pseudoprogression or true recurrence.
Serial imaging studies have been the mainstay in resolving the issue in day-to-day practice and may result in treatment delay for patients with true progressive disease 1.
Up to 30% of patients treated with combined chemoradiation for high-grade glioma may exhibit indistinguishable MRI findings of true tumor progression from pseudoprogression 2.
Perfusion MRI is the most widely used imaging technique to diagnose pseudoprogression and has high reported diagnostic accuracy.
The combination of MRS and diffusion-weighted imaging and/or perfusion MRI seems to be particularly powerful,
with diagnostic accuracy reaching up to or even greater than 90%.
Our aim was to retrospectively evaluate the utility of morphologic and functional MRI characteristics in predicting the diagnosis of true versus pseudoprogression.