Keywords:
Interventional non-vascular, Biliary Tract / Gallbladder, Gastrointestinal tract, Ultrasound, Technical aspects, Laboratory tests
Authors:
K. Sabarwal1, T. Pedelty2, T. Osborne1, V. Joshi1, A. Chapman1, S. Prabhudesai1; 1Chertsey/UK, 2Leeds/UK
DOI:
10.26044/ecr2019/C-1010
Results
A total number of 49 patients were identified over the 5-year period.
The mean age was 74.5 years (range 33 to 94).
59.2% were female (n=29).
Based on the individual consultant radiologist’s preference,
the procedure was performed with ultrasound guidance alone in 57.1% of cases (n=28),
ultrasound with fluoroscopic guidance in 32.6%,
(n=16) and CT guidance in 6.1% (n=5).
A transhepatic approach was adopted in 51% of cases (n=25).
The technical success rate was 100%.
An aspirate was obtained in all 49 cases,
however in 2 patients,
no microbiological analysis was found on our electronic pathology system.
Thus 47 aspirates underwent microbiological analysis,
of which 30 (63.8%) were positive for microbes.
Out of the 30 positive aspirates,
24 (80%) were resistant to some class of antibiotics.
A breakdown of the antibiotic resistance noted in our sample size is shown in figure 1.
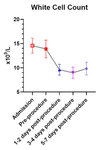
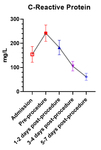
Figures 2 and 3 demonstrate the trend in the white cell count (WCC) and C-reactive protein (CRP) levels respectively.
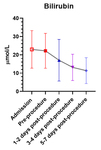
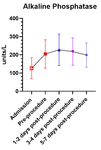
The trend in the liver function tests are illustrated in figure 4 (bilirubin),
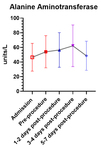
figure 5 (alkaline phosphatase; ALP) and figure 6 (alanine aminotransferase; ALT).
The mean time from admission to the procedure being performed was 3.4 days.
The mean time from procedure to discharge was 9.9 days,
with the average total length of stay being 13.3 days