Normal Anatomy
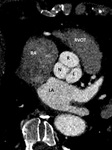
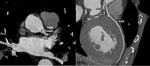
The aortic valve consists of three cusps with curvilinear attachments to the aortic ring. These are known as the left coronary cusp,
right coronary cusp and posterior non-coronary cusp Fig. 1.
On the superior/aortic sides of these cusps are small anatomic dilatations of the aortic root, forming the three sinuses of Valsalva. The coronary arteries arise from these sinuses,
which are named the left,
right and non-coronary (posterior) sinuses.
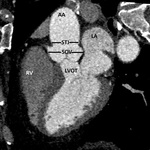
Above the sinuses,
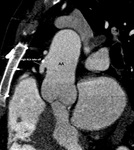
the tubular portion of the ascending aorta begins (sinotubular junction).
The functional unit from the ventriculoaortic junction to the sinotubular junction makes up the aortic root Fig. 2 .
There are four main coronary arteries evaluated on cardiac CT:
1.
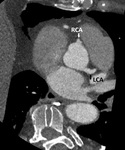
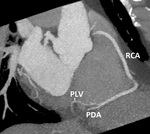
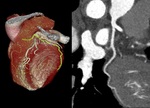
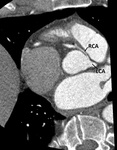
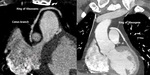
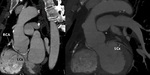
The right coronary artery (RCA) arises from the right (anterior) coronary sinus Fig. 3 Fig. 4 .
It courses through the right atrioventricular (AV) groove between the right atrium and ventricle,
giving rise to the following branches:
- conus artery (in 60%) supplying the right ventricular outflow tract
- sinoatrial node artery (in 60%,
arises from the circumflex artery in remaining 40%)
- diagonal branches run anteriorly to supply the anterior right ventricular wall
- acute marginal artery comes off acutely to supply the anterior wall of the right ventricle
- AV nodal artery
- in 65%,
the RCA continues as the posterior descending artery (PDA),
known as 'right dominant' circulation,
supplying the inferior ventricular walls and inferior one third of the interventricular septum Fig. 5
- the posterior left ventricular artery (PLV),
also known as the posterolateral artery,
is a terminal RCA branch; it is also commonly supplied by the left circumflex,
or rarely by the left anterior descending artery
2.
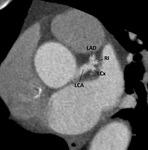
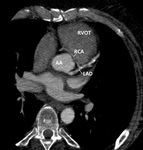
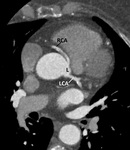
The left main coronary artery (LCA) arises from the left coronary sinus Fig. 3.
It courses between the right ventricular outflow tract anteriorly,
and the left atrium posteriorly, dividing into the circumflex and left anterior descending (LAD) artery.
In 15% of individuals,
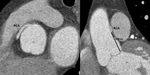
a third branch arises in between the LAD and circumflex, named the ramus intermedius Fig. 6 .
This behaves similarly to the diagonal branches of the circumflex artery.
3.
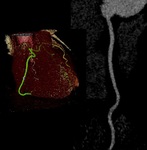
The left anterior descending artery (LAD) courses in the interventricular groove towards the cardiac apex Fig. 7 .
It gives off the following branches:
- diagonal branches,
which run laterally to supply the antero-lateral wall of the left ventricle.
These are variable in number,
and labelled D1,
D2,
etc.
The first diagonal branch serves as an anatomical boundary between the proximal and mid-LAD
- septal branches,
supplying the anterior part of the interventricular septum
4.
The left circumflex (LCx) artery lies in the left AV groove between the left atrium and left ventricle Fig. 8 .
It gives off:
- obtuse marginal branches,
labelled M1,
M2,
etc,
supplying the lateral wall of the left ventricle
- in approximately 10% of individuals,
the LCx supplies the PDA,
known as 'left dominant' circulation
Aberrant Coronary Artery Origins
We present a case series of aberrant coronary artery origins each one demonstrating a different key learning point.
Case 1: Right coronary artery (RCA) origin from left main stem,
inter-arterial course Fig. 9
A 56 year old male was referred from a district hospital,
having had failed cannulation of the RCA at catheter angiography.
The patient had undergone stenting of the LAD 9 months previously.
CT coronary angiogram confirmed the RCA arising from the left main stem,
2.3 mm from the LCA origin,
and passing between the pulmonary artery and aortic root to reach the AV groove.
The RCA was disease free and the two LAD stents were patent.
The patient underwent follow-up in his base-hospital and is currently being treated medically.
Case 2: RCA origin from left anterior descending (LAD),
inter-arterial course Fig. 10 .
A 68 year old male was referred from a district hospital. CT coronary angiogram confirmed a non-dominant RCA with an aberrant origin,
arising from the proximal LAD and running anteriorly between the aorta and pulmonary artery to reach the AV groove.
There was no coronary artery stenosis and a normal origin of the LCA.
The patient returned to his base hospital for optimal medical management.
Case 3: High RCA take-off from ascending aorta Fig. 11
A 50 year old male with a long history of ischaemic heart disease and previous LAD stent presented with ST-elevation myocardial infarction.
Catheter angiography confirmed LAD occlusion. The right coronary artery could not be cannulated,
therefore CT coronary angiogram was requested.
CT coronary angiogram revealed aberrant origin of the RCA,
arising high above the aortic valve cusps,
at a 3 o'clock position above the sinotubular junction. This would be prone to compression due to the aberrant origin between the aorta and main pulmonary artery.
There was moderate mid and distal RCA stenosis.
The patient subsequently underwent triple coronary artery bypass grafting for definitive surgical revascularisation.
Case 4: RCA origin from left coronary sinus Fig. 12
A 73 year old female presented with atypical chest pain.
A CT coronary angiogram was requested which revealed a dominant RCA arising from the left coronary sinus,
adjacent to (but separate from) the left main stem.
The RCA passed anteriorly between the aortic root and pulmonary artery to the AV groove.
There was high grade mid-RCA stenosis and moderate mid-LAD stenosis.
She subsequently underwent catheter angiography with angioplasty and stenting of the RCA.
Case 5: Left coronary artery (LCA) from right coronary sinus,
inter-arterial course Fig. 13
A 73 year old female presented with recurrent episodes of chest pain on exertion.
Blood pressure was high at 170/86.
A CT coronary angiogram showed the LCA arising from the right coronary sinus,
with the left main stem passing between the aorta and pulmonary artery.
There was no coronary artery stenosis.
She has been followed up under the cardiologists and is currently being managed medically,
with surgical intervention unlikely to be required due to age.
Case 6: Separate ostia of the LCA and left circumflex artery (Absent left main stem) Fig. 14
A 65 year old male presented with chest pain and abnormal ECG findings suggestive of coronary artery disease.
CT coronary angiogram revealed absence of the left main stem,
with the LCA and LCx arising separately from the left coronary sinus.
There was apical left ventricular hypertrophy in keeping with hypertrophic obstructive cardiomyopathy,
which was confirmed on cardiac MRI.
Case 7: High RCA origin & Ring of Vieussens as sole supply to LAD territory.
A 62 year old male,
with a history of previous CABG,
was referred for CT coronary angiogram due to inability to cannulate the RCA and LMS at catheter angiography.
CT coronary angiogram revealed aberrant origin of the RCA well above the sino-tubular junction Fig. 15 . The native RCA gives a large conus branch which supplies the LAD territory via a ring of Vieussens (normal variant) Fig. 16 .
Aberrant origin of the circumflex artery off the proximal RCA just distal to the conus branch Fig. 17 .
Occlusion of the LIMA to LAD graft.
Patent SVG to PDA and SVG to OM1 grafts.
He was subsequently reviewed in the cardiothoracic surgery clinic,
and was not deemed a suitable candidate for redo CABG due to multiple comorbidities.
He is therefore being managed with optimal medical therapy.
Clinical Significance
Aberrant origin of a coronary artery is often an incidental finding.
However,
patients with these anomalies can be symptomatic,
with angina,
syncope and arrhythmia.
They are an important cause of sudden death in athletes,
military recruits and other young adults 5,
7,
8,
9.
The mechanisms for this association are unclear and various theories have been proposed. Possible causes include:
- compression between the great vessels (aorta and pulmonary artery) because of increased aortic size and wall tension during periods of systemic hypertension such as exercise
- flow restriction secondary to acute angulation of the origin (also exacerbated by aortic dilation),
and
- ostial stenosis / 'slit-like' ostium
Such patients are generally treated with definitive surgical revascularization,
with either coronary artery bypass grafting or reimplantation of the coronary ostia.
Management
In patients with symptoms arising from ventricular tachyarrhythmia or myocardial infarction,
surgical intervention is indicated,
particularly in cases of the origin of the left coronary artery from the right sinus of Valsalva.
The commonly encountered surgical interventions described in the literature include: 10,
11,
12
- Coronary artery bypass grafting (CABG) with the saphenous vein or internal mammary artery.
- Explantation and re-implantation of the coronary ostia.
This may result in neo-ostial stenosis and is not useful for intramural coronary arteries.
- Unroofing (marsupialization) of the coronary artery to relieve the acute angulation of its origin and eliminate possible compression between the great arteries.
This is only possible if there is a significant intramural course.
- For patients without any intramural course,
the “hinge twist” procedure has been described,
in which the proximal LCA is re-orientated and rotated out of the area of compression between the great vessels 13.
- Pulmonary artery translocation and intracoronary stents to prevent vessel compression are other alternative surgical procedures that have been described in the literature 14.
Benefits of surgical treatment in asymptomatic individuals with AAOCA (anomalous aortic origin of coronary artery) have not been well established.
As our case series demonstrates,
optimising medical management is the preferred strategy in the majority of older patients with an incidental finding of an aberrant coronary artery origin,
including those with 'high-risk' anatomy,
such as a high pressure inter-arterial course.