Cardiac CT and MR studies were evaluated from 2014 to 2018,
in total 1520 Cardiac CTs and 1756 cardiac MRs were performed.
These cases were then searched with keyword ''aneurysm" in our PACS search engine,
we found 28 cases of different cardiac aneurysm with detailed clinical history,
lab findings, therapeutic procedure performed and clinical outcomes.
These cases were classified as follows- Refer to table 2
CONGENITAL ANEURYSMS
A) LEFT VENTRICLE ANEURYSMS
1.
Left ventricular diverticulum
It is a congenital true aneurysm.
It is a diverticulum like outpouching of the myocardial wall,
which contains myocardium and pericardium and shows normal synchronous contraction with rest of myocardium.
Prevalence of these lesions is 0.4% and may be associated with midline thoraco-abdominal defects.
MRI bSSFP Cine images are useful sequences which demonstrate synchronous contraction of diverticulum with rest of myocardium (2).
Refer to figures (1 and 2) and video (1) for representative cases
2.
Congenital sub mitral aneurysm - Cases with thrombosis and without thrombosis
A sub-mitral aneurysm is a congenital outpouching of the left ventricular wall,
invariably occurring adjacent to the posterior leaflet of mitral valve.
Patients with sub mitral aneurysm can be asymptomatic or present with features of mitral valvular disease,
arrhythmias,
thromboembolism and myocardial ischemia (secondary to compression of LCX) (3).
Du Toit et al.
has classified sub mitral aneurysm into: type I (single localized neck),
type II,
multiple necks (separate distinct openings),
and type III (involvement of the entire mitral annulus) (4).
Refer to figures (3 and 4) and Video 2 for representative cases
B) ATRIAL ANEURYSMS
1.
Congenital anomalous communication between Right Pulmonary artery to Left Atrium:
Pulmonary AV fistula is abnormal communication between a pulmonary artery and pulmonary vein.
Communication between right pulmonary artery (RPA) and left atrium (LA) is an unusual cyanotic congenital malformation which is a form of pulmonary AV fistula.
In this cardiac anomaly,
deoxygenated blood is shunted directly to LA by RPA bypassing lungs,
thus resulting in central cyanosis,
oxygen desaturation,
and dyspnoea.
Associated atrial septal defects are common.
Other cardiac anomalies are rare,
but anomalies of the right lung such as the absence of the lower or middle lobe,
right lung sequestration,
and diverticulum of the right main bronchus,
have been reported.
Communication between the RPA and the LA can be classified into four types,
based upon the anatomy of pulmonary venous drainage pattern (5).
Type I: Normal pulmonary venous drainage pattern.
Type II: Absent right inferior pulmonary vein with a fistulous connection at the normal site of its origin.
Associated are right lung abnormalities such as absent one or more lobes.
Type III: All pulmonary veins connected to the aneurysmal pouch.
Type IV: Right inferior pulmonary vein replaced by three small veins connected to the aneurysmal pouch.
Our case was type I with normal pulmonary venous drainage.
In our case,
9-year female presented with cyanosis and dyspnoea.
ECHO showed aneurysmal dilatation of left atrium,
dilated RPA with dilated RV and RA.
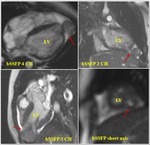
Cardiac MRI was performed which showed anomalous fistulous communication between RPA and LA with features of pulmonary hypertension (Refer figure 5).
Pre-op Cath study confirmed MR findings (refer video 3),
and there were no other cardiac anomalies such as septal defects.
The patient was treated with,
ligation of pulmonary A-V fistula of the right lower lobe through right thoracotomy approach.
Post-procedure patient was stable.
Follow up after 8 months,
there is alleviation of patient’s symptoms.
2.
Congenital aneurysm of Right atrial appendage
Aneurysm of the right atrial appendage is a rare cardiac anomaly that is most commonly diagnosed during adulthood.
These are mostly asymptomatic but when symptomatic patient usually presents with atrial arrhythmias and dyspnoea.
In the literature search,
there are documented cases of RAA aneurysms with septal defects,
LAA aneurysm.
Due to its association with atrial fibrillation,
thrombus formation and its subsequent pulmonary embolism or systemic embolism (septal defects) are of concern (6).
Refer figure 6 for a representative case
3.
Ruptured left sinus of Valsalva into the left atrium
Sinus of Valsalva aneurysms (SVA) are unusual aneurysms,
which can be congenital or acquired.
A deficiency of normal elastic tissue and abnormal development of the bulbus cordis have been associated with the development of congenital SVA.
Other disease processes that involve the aortic root (e.g.,
atherosclerotic aneurysms,
syphilis,
endocarditis,
cystic medial necrosis,
and chest trauma) may also produce SVA,
although these usually involve multiple sinuses Approximately 61% of SVA originate from the right sinus of Valsalva,
while SVAs originating from noncoronary (26%) and left sinuses (12%) are exceedingly rare.
In this actual review,
rupture or fistula from the noncoronary sinus to the left atrium was extremely rare (1.5%) (7).
Clinical presentation depends upon chamber to which SVA has ruptured and its acuteness.
Sudden perforation/rupture to LA or its appendage results in volume overload cardiac failure and sudden cardiac death.
Gradual perforation/rupture to appendages / right atrium usually results in thrombus formation and its complications.
In our case,
26-year female presented with cardiac failure.
Patient was surgically treated with aneurysmal neck ligation (refer figure 7)
ANEURYSMS DUE TO MYOCARDIAL INFARCTION
Ventricular aneurysms occur most commonly after MI,
3-5% of patients following MI develop aneurysms,
however,
this population is declining due to early and prompt treatment.
LV aneurysms are common with predominant anterior wall involvement.
When symptomatic,
ventricular aneurysms may present with heart failure symptoms due to systolic bulging with resulting “steal” of stroke volume as well as ventricular arrhythmias.
The most feared complication is a rupture with resulting tamponade.
Pseudoaneurysms are most likely to rupture than a true aneurysm (2).
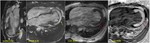
Refer figure (8 to 10) for representative cases
ANEURYSM DUE TO VASCULITIS
Interatrial septal thrombosed aneurysm from Right Coronary Artery (RCA) vasculitis
Coronary artery aneurysm with the involvement of interatrial space is a rare entity.
They usually present with atrial fibrillation which is potential for left atrial thrombus formation.
In the natural course of the disease,
interatrial aneurysm may eventually get thrombosed or may rupture into the right atrium,
which is later complicated by congestive heart failure (8)
In our case 32-year female presented with low-grade fever,
malaise,
dyspnoea,
and palpitations.
Her RFT was deranged,
hence contrast CT/MR was deferred.
ECG showed atrial fibrillation which was reverted to sinus rhythm and sent for cardiac MR.
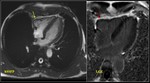
In MR,
there was inter-atrial lesion which was T1/STIR hyperintense,
shows no enhancement on perfusion imaging (refer video 4),
no enhancement on early and delayed contrast.
The same lesion in CT was hyperdense with peripheral calcification.
RCA aneurysmal and extending to interatrial space.
With clinical features and deranged RFT,
vasculitis of RCA with the involvement of renal arteries was considered.
Patient is on dialysis and steroid therapy planned for elective surgery (Refer figure 11).
ANEURYSM DUE TO INFECTIOUS ENDOCARDITIS
1.
Infective endocarditis of mitral valve with sub mitral aneurysm
Sub mitral aneurysm of LV is an unusual condition of varied aetiologies.
In this case,
sub mitral aneurysm of the LV cavity is due to infective endocarditis of the mitral valve.
In infective,
inflammatory cause,
there is focal myocardial involvement which subsequently causes myocardial rupture resulting in pseudoaneurysm which is contained by peripheral thrombus and pericardium (9)
Refer figure (12) for the representative case.
2.
Mycotic aneurysms
These are aneurysms secondary to infection,
which causes destruction,
thinning and eventual rupture of the wall causing mycotic aneurysms.
Since their true wall is destroyed and is walled off by organized hematoma and pericardium,
they are pseudoaneurysms.
Most common causative agents are bacteria specifically staphylococcus and streptococcus.
Risk factors are endocarditis,
IV drug abuse,
and immune-compromised state.
Treated with antibiotics and surgery is necessary in cases with impending rupture (2).
Refer to figures (13 and 14) for representative cases.
ANEURYSMS DUE TO HERITABLE GENETIC DISORDERS
1.
Arrhythmogenic Right Ventricular Cardiomyopathy / Dysplasia (ARVD/C)
It is mostly familial cardiomyopathy characterized by fibrofatty infiltration of RV myocardium.
It presents with ventricular tachycardia and sudden death in 20% of patients.
Diagnosis is according to Task force criteria which is revised in 2010 which includes Echo criteria,
CMR criteria,
RV angiography criteria,
ECG abnormalities,
tissue diagnosis,
and family history into consideration.
Cine images demonstrate RV dilatation,
RV microaneurysms,
and sacculations,
dyssynchronous contraction,
T1 demonstrate fatty infiltration,
LGE imaging shows myocardial scar and RV volumetry by CMR provides RV EDV and RV EF which is necessary for diagnosis according to Task force criteria (10)
Refer figure (15) for a representative case
2.
Brugada Syndrome:
It is a genetic disease with mutations of sodium channel gene resulting in typical ECG changes and sudden cardiac death secondary to ventricular fibrillation.
It is seen in young adults.
ECG changes include right bundle branch block,
ST segment elevation in right precordial leads.
Previously it was thought that there were no structural abnormalities,
but recently RV dilatation/dysfunction,
regional wall motion abnormalities,
aneurysms and even fibro-fatty infiltration similar to ARVD.
These morphological changes are secondary to electrical conduction abnormalities rather than myocardial scar (11).
Refer figure (16) and video (5) for a representative case
MISCELLANEOUS
1.
Takotsubo Cardiomyopathy
Also known as stress-induced cardiomyopathy or apical ballooning syndrome.
More commonly seen in post-menopausal women following a recent stressful event.
These patients present with acute coronary syndrome with ST-segment elevation,
T wave inversion,
and Q waves in ECG,
mild cardiac enzymes elevation.
Coronary angiography will be normal.
MRI shows edema in apical and mid-distal myocardial segments which show akinesia/dyskinesia on cine images.
No myocardial scarring hence normal LGE images.
Recovers after treatment in 95% of cases (11)
Refer figure (17) and video (6) for a representative case
2.
Apical Aneurysm in Hypertrophic Cardiomyopathy.
Apical LV aneurysm is a rare complication of HCM that leads to thrombosis an arrhythmia.
These are a thin wall of LV apex with replaced collagen tissue.
Apical LV thinning is defined as myocardial thickness less than 5mm in end diastole.
MR cine images show thinning and dyskinesia of LV apex and LGE images show enhancement which represents myocardial scarring (12).
Refer figure (18) for a representative case