The authors performed a literature review on the topic of eponyms in gastroenterology,
chose a number of them and executed a search through their case archive to find illustrative examples.
The authors present in alphabetical order each eponym and discuss its imaging manifestations and the historical background of the individual for whom it was named.
Balthazar score
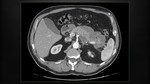
The CT severity index for grading the severity of acute pancreatitis (10-point scale) consists of two scores - Balthazar score (Fig. 3) (grading pancreatic inflammation (Fig. 4) from A to E – 0 to 4 points) and grading the extent of pancreatic necrosis (Fig. 5) (0-6 points).
The Balthazar score has been used alone for some time,
but the addition of a score for pancreatic necrosis has improved the correlation with clinical outcome [2,5].
The Balthazar score was first proposed by E.
J.
Balthazar and al.
in the article titled “Acute pancreatitis: value of CT in establishing prognosis”,
published in 1990.
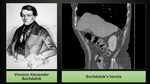
Bochdalek hernia
A Bochdalek hernia is a congenital diaphragmatic hernia,
occurring posteriorly.
It’s more commonly left-sided and may lead to prolapse of retroperitoneal structures into the chest cavity including retroperitoneal fat,
kidneys,
etc.
When large,
these hernias present in infancy with the most common complication being pulmonary hypoplasia.
In adults,
they are rare,
usually small,
and asymptomatic.
They were first described by the Czech Anatomist and Pathologist,
Vincenz Alexander Bochdalek (Fig. 6),
who was born in 1801 in Litoměřice and spent most of his life working in Prague.
Other eponyms associated with him include the Bochdalek's cyst at the root of the tongue and Bochdalek's ganglion of the dental nerve in the maxilla.
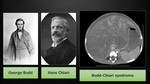
Budd-Chiari syndrome
Budd-Chiari syndrome is a rare disorder characterized by obstruction of the hepatic venous outflow.
At least two of the hepatic veins must be affected to have a clinically significant disease with thrombosis being the leading cause.
Liver congestion and hypoxic damage to the hepatocytes lead to fibrosis,
portal hypertension and eventually liver failure.
It may present acutely with abdominal pain,
ascites, and hepatomegaly or chronically with symptoms related to portal hypertension.
It is named after Budd and Chiari (Fig. 7).
George Budd (1808 –1882) was an English physician,
whose research topics included cholera,
scurvy,
and diseases of the stomach and liver.
In 1845,
in his monograph “Diseases of the Liver”,
he described many disorders including what later became known as Budd-Chiari syndrome.
Hans Chiari (1851 − 1916) was an Austrian pathologist,
whose research dealt largely with postmortem examinations.
Besides the Budd-Chiari syndrome,
his name is also part of another medical eponym – the Arnold-Chiari malformation.
Caroli disease
Caroli disease is a rare autosomal recessive disorder which consists of cystic dilatation of intrahepatic bile ducts.
It has no gender predilection and usually presents in childhood or young adulthood.
It could be associated with renal disorders including autosomal polycystic kidney disease,
medullary sponge kidney,
and medullary cystic disease.
It may be diffuse,
lobar or segmental.
Dilatation is usually segmental and saccular and not fusiform,
which could help in the differential diagnosis.
Clinical symptoms may include right upper quadrant abdominal pain,
jaundice,
cholangitis and in severe forms - portal hypertension and liver failure.
The disease was named after Jacques Caroli (Fig. 8) (born 1902 near Versailles),
a gastroenterologist,
who first described it in 1958.
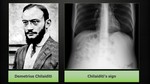
Chilaiditi sign
The term Chilaiditi sign is used to describe the interposition of bowel loops between the right hemidiaphragm and the liver on X-ray.
It’s important not to mistake it for a pneumoperitoneum as it may result in unnecessary further investigations or operations.
When associated with pain it is called Chilaiditi syndrome.
It can be described on a radiograph when gas is seen between the liver and the diaphragm with visible haustra suggesting that it is located within a bowel.
In some cases,
CT examination may be necessary to confirm the diagnosis.
It was named after the radiologist of Greek origin Demetrius Chilaiditi (Fig. 9) (born 1883 in Vienna) who described it in 1910 [3].
Child-Pugh criteria
The Child-Pugh score (Fig. 10) is a scoring system used to measure the severity of chronic liver disease (mainly liver cirrhosis).
It includes several categories: total bilirubin,
serum albumin,
INR,
ascites and hepatic encephalopathy.
The point scores for each of these categories are added up and the chronic liver disease is classified as class A,
B,
and C.
The Child-Pugh score informs clinicians about the liver function and can be useful when planning interventions including resections and transplantation.
It correlates with the perioperative mortality.
The surgeon and portal hypertension expert Charles Gardner Child (1908–1991) first proposed the scoring system in 1964 in a textbook on liver disease.
It was later modified by Pugh in 1972 with replacing Child's nutritional status with the prothrombin time or INR,
and the assignment of scores of 1–3 to each criterion.
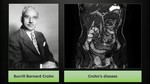
Crohn’s disease
Crohn’s disease is an idiopathic inflammatory bowel disorder defined by diffuse discontinuous gastrointestinal tract inflammation with the terminal ileum and proximal colon being most commonly affected.
It can,
however,
occur anywhere along the digestive tract,
including the mouth and esophagus.
Extraintestinal involvement is also common including skin,
joint,
eye,
kidney,
and liver.
It usually presents in early adulthood with a with both genetic and environmental factors playing a role in its epidemiology.
It was named after Burrill Bernard Crohn (Fig. 11) (born 1884 in New York),
an American gastroenterologist,
who first described the condition as 'regional ileitis' in 1932.
He never named the disease with his name in any of his scientific works and was also against an official resolution during a Conference in Prague,
by means of which regional ileitis was designated as Crohn's Disease.
During his long and prolific career,
he worked also on abdominal hemorrhage and the diseases of the pancreas,
authoring more than 150 articles and four books [1].
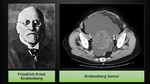
Krukenberg tumor
A Krukenberg tumor refers to a metastatic malignancy in the ovary.
It may originate from different primary sites,
most commonly gastric cancer,
followed by colorectal carcinoma.
They are often bilateral and more common in women who are still in their reproductive years with the median age of presentation being 48 years [8].
Radiologically their features are non-specific and can be indistinguishable from primary ovarian cancer.
Krukenberg tumors are named after Friedrich Ernst Krukenberg (Fig. 12) (1871–1946),
a German physician who in 1896 described five cases of young women with what he thought to be a new type of a primary ovarian tumor.
It was later shown that these cases were of metastatic gastrointestinal origin.
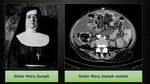
Sister Mary Joseph nodule
Sister Mary Joseph’s nodule refers to a malignant metastatic umbilical nodule - an uncommon finding,
usually associated with advanced primary neoplasm of the gastrointestinal and genitourinary tract.
The mechanism of the spreading to the umbilicus is unclear,
however,
several hypotheses have been formulated including: by contiguity,
lymphatic and hematic spreading.
Patients are usually between 40 and 70 years of age with a slight female predilection.
The term was first used by Sir Hamilton Bailey,
an English surgeon,
in his book “Demonstrations of Physical Signs in Clinical Surgery”,
published in 1949.
It was named after Sister Mary Joseph (Fig. 13),
who was superintendent nurse at the St.
Mary’s Hospital of Rochester.
She was born Julia Dempsey,
in New York,
1856,
and was the first to observe that patients with advanced abdominal-pelvic malignancies,
frequently presented with a periumbilical nodule [6].
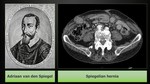
Spigelian hernia
Spigelian hernia is a rare type of an abdominal hernia,
located along the semilunar line.
It is more common in older adults with a slight female predilection and can be both congenital or acquired.
In male infants,
the Spigelian hernia could be associated with ipsilateral cryptorchidism.
The diagnosis of a Spigelian hernia can be a challenge since it lies deep to a muscle and is usually small in size.
Spigelian hernia is named after Adriaan van Spieghel (Fig. 14),
who described the semilunar line.
He was a Flemish anatomist,
born in Brussels in 1578,
who for much of his career practiced medicine in Padua.
His name is given not only to the Spiegelian (semilunar) line and the Spigelian hernia but is also used to describe the caudate lobe of the liver as Spiegel's lobe.
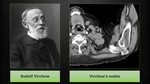
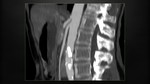
Virchow’s node
An enlarged left supraclavicular lymph node as the first sign of gastric cancer is often called Virchow‘s node.
Since the left supraclavicular nodes receive lymphatic drainage via the thoracic duct,
from the thorax,
abdomen, and pelvis and are the place where the lymph is returned to the venous circulation through the subclavian vein,
various malignancies (including lymphoma,
cancer of the lung,
breast,
esophagus,
testes and ovary) could be the cause of their enlargement.
Even though left supraclavicular lymphadenopathy is highly suspicious of malignancy,
the differential diagnosis should also include causes like tuberculosis,
sarcoidosis etc.
This association between gastric cancer and left supraclavicular lymphadenopathy has been noted first by the German pathologist Rudolf Virchow (Fig. 15).
He worked at the Charite Medical School in Berlin and has been the author of multiple important medical discoveries.
Wilkie syndrome
Superior mesenteric artery syndrome or Wilkie syndrome is a rare cause of small bowel obstruction characterized by proximal duodenum compression due to a narrowing of the space between the upper mesenteric artery and the aorta.
The disease is associated with a reduction in body weight and,
in particular,
reduction of the mesenteric fat tissue,
presenting with acute symptoms of small bowel ileus or with chronic complaints of episodic abdominal pain.
It is rare and usually associated with conditions causing weight loss such as anorexia nervosa,
major surgery,
malignancy etc.
There are also predisposing factors including increased spinal lordosis,
short ligament of Treitz or unusually low origin of the superior mesenteric artery [9].
It can be demonstrated by fluoroscopy showing dilatation of the first and second part of the duodenum and compression of the third part,
or by CT/MRI,
which can both visualize the reduced aortomesenteric angle and aortomesenteric distance (Fig. 16).
Even though it is named after Wilkie,
who published a large series of cases in 1927 and described the clinical symptoms of the condition, it was first reported in 1861 by Carl von Rokitansky (Fig. 17).
He was born in 1804 in Bohemia and spent most of his life working in Vienna.
During his career,
he did thousands of autopsies and contributed immensely to the art of medicine describing many pathologies some of which bear his name to this day,
including Müllerian agenesis (Mayer-Rokitansky-Küster-Hauser syndrome),
Rokitansky's triad (in pulmonary stenosis) and Rokitansky nodule (in teratomas).
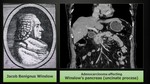
Winslow pancreas
The pancreas is divided into head,
neck,
body,
and tail.
The uncinate process (sometimes called also Winslow pancreas) is considered as an extension to the head and is the only part of the organ located posterior to the superior mesenteric vein.
During the development,
the pancreas arises from two separate parts - dorsal (giving rise to the isthmus,
body,
and tail) and ventral (forming the head and uncinate process).
This embryology also explains the number of variations in the fusion of the two pancreatic parts as well as the multiple variants in the formation of the pancreatic duct.
Jacob Benignus Winslow (1669-1760) was a Danish anatomist,
physicist,
and surgeon who worked in Paris (Fig. 18).
Wirsung,
duct of
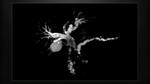
The main pancreatic duct is joining the pancreas to the common bile duct into the ampulla of Vater which later enters the duodenum at the papilla of Vater.
Due to its complex embryologic development,
it can demonstrate multiple variations in its formation,
course and configuration.
The normal pancreatic duct measures 2–3 mm in caliber with its diameter slightly increasing from the tail to the head.
The duct of Wirsung (Fig. 19) is named after the German anatomist Johann Georg Wirsung (born 1589 in Augsburg) who described it during the dissection of a man who had been recently hanged for murder.
In 1643 Wirsung was murdered,
reportedly as the result of an argument as to who was the discoverer of the pancreatic duct.
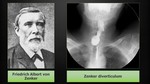
Zenker Diverticulum
A Zenker diverticulum is a pseudodiverticulum since it does not involve all layers of the esophageal wall.
It is a herniation of the mucosa and submucosa through a focal weakness in the hypopharynx muscles.
A sac with a narrow neck is formed,
which can lead to entrapment of liquid and food.
While it may be asymptomatic,
it can present with dysphagia,
regurgitation,
cough,
halitosis [7].
A barium swallow,
an endoscopy or a combination of both can be used to confirm the diagnosis.
It was described in 1877 by Friedrich Albert von Zenker (Fig. 20),
pathologist and physician born in Dresden in 1898.
He is also famous for his discovery of trichinosis.