Keywords:
Neoplasia, Cancer, Observer performance, Ultrasound, CT, Urinary Tract / Bladder, Kidney, Abdomen
Authors:
H. M. A. OBrien, N. Burns-Cox, J. Kasznia-Brown, P. Burn; Taunton/UK
DOI:
10.26044/ecr2019/C-1118
Results
A total of 37 patients were included. The tumour sites included: ureter (15 patients),
renal pelvis (12),
renal calyx (4),
renal parenchymal infiltration (6) (See figure 1).
US scans were performed as an initial investigation in 23 patients.
15 of these patients were referred through the one stop macroscopic haematuria clinical pathway.
Tumour was correctly identified in 3 and hydronephrosis identified in 13 cases.
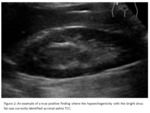
We concluded that US had sensitivity for detecting TCCs of 13% and a sensitivity of 70% for detecting any renal abnormality that could indicate underlying upper tract TCC. Figure 2 demonstrates an example of a true positive US scan demonstrating a central soft-tissue mass in the echogenic renal sinus fat,
a typical appearance of renal pelvis TCCs1.
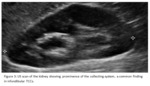
Figure 3 shows another true positive case demonstrating prominence within the collecting system.
Hydronephrosis is a common finding in infundibular TCCs2.
TCC was subsequently confirmed on CT.
A total of 14 patients had a CT scan as their initial investigation.
Indications included follow-up scans for other malignancies,
investigating symptoms of renal colic and looking for renal tract malignancy.
On retrospective review of the CT findings,
all tumours were present on CT.
We therefore said that CT had sensitivity of 100% for detecting upper tract TCCs.
However,
6 tumours were missed on CT by the initial reporting radiologist.
We therefore said that CT had a pick-up rate of 84%.
In looking at the time taken to correctly diagnose upper tract TCCs in our trust,
we found 57% of patients had their diagnosis made in <1 month while 24% of patients waited >100 days for their diagnosis to be made (See figure 4). Some of the causes of delayed time to diagnosis and discrepant cases are discussed below.
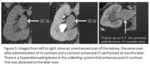
Figure 5 shows an example of a patient who presented with macroscopic haematuria.
They had an unenhanced and delayed phase scan on initial presentation.
An upper pole TCC was missed on these scans.
They then had a CT Angiogram 16 months later as part of their work-up for prostatic embolization to treat ongoing haematuria.
It was on this scan that the TCC was correctly identified.
In reviewing this CT retrospectively the Hounsfield Units of the collecting system on the initial scan was 36 on the unenhanced phase.
TCCs typically are hyperattenuating (5-30HU) on unenhanced scans compared to urine2. In addition,
it demonstrated enhancement post administration of intravenous (IV) contrast (HU 64),
a feature that is highly suspicious of malignancy.
Hydronephrosis is the most frequent CT finding in ureteric TCC and hydroureter can often be seen proximal to the obstructing tumour2.
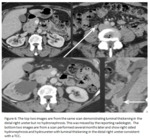
Figure 6 demonstrates an example of a missed ureteric TCC.
The patient had a staging scan for sigmoid cancer.
The kidneys appeared normal but the tumour in the distal right ureter was missed.
The tumour was identified several months later on a follow up scan that demonstrated right sided hydronephrosis and hydroureter to the point of obstruction in the distal ureter.
On retrospective review of this case there was no hydronephrosis on the initial scan.
Ureteric wall thickening (eccentric or circumferential) and luminal narrowing are other features of disease2.