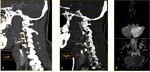
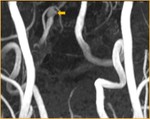
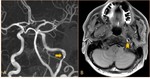
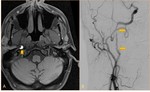
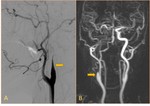
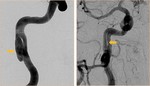
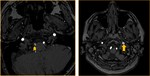
The radiologists should search for CAD findings at the neuroimaging procedures such as lumen-opacifying methods (CTA/ MRA/ DSA) and cross-sectional procedures (CT/MRI) when clinical features are suspicious for dissection.
Dissections can present as stenosis,
occlusion,
or aneurysmal dilatation at the CTA,
DSA,
and MRA. CT and MRI can be helpful to show the intramural hematoma at the vessel wall.
The sensitivity and specificity of MR-MRA and CT-CTA in the diagnosis of CAD are relatively similar to DSA.
It seems logical to start with non-invasive techniques when there is a possibility of CAD.
There is no need for DSA if the diagnosis is clear with CTA or MRA.
Whereas if there is an open-ended result at the cross-sectional methods and high clinical suspicion of CAD in a young patient DSA should be preferred to evaluate.
CT: Unenhanced brain CT may help to demonstrate potential results of dissections such as ischemia and hemorrhage. Also,
in some cases,
an intramural hematoma may be seen as a crescent-shaped hyper-attenuated area at the vessel wall.
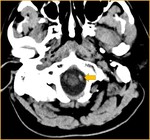
The findings of ICA and VA dissections on CT;
- Subarachnoid hemorrhage
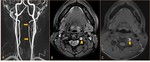
- Infarct at the ICA or VA territory (Fig. 5)
- Crescent-shaped hyper attenuated area at the vessel wall as a result of the intramural hematoma
- Occlusion of the dissected artery (Hyperdense artery sign) (Fig. 9)
-CTA: CTA is an easily accessible method and well-tolerated examination to evaluate CAD.
The time of image acquisition is faster than MRI.
When compared with DSA,
CTA is a minor invasive method and contrast amount is lesser.
Multiplanar reformat images help to show both vessel lumen and wall better.
However,
in some cases,
bony regions may hide the dissection findings because of the artifacts.
In addition,
the radiation exposure is a disadvantage and make the use of CTA unpractical in some groups such as pregnant and pediatric patients.
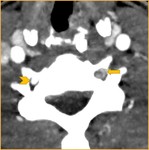
The findings of ICA and VA dissections on CTA;
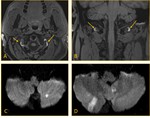
- An eccentric narrowed lumen ( Fig. 6 ,
Fig. 7 ),
- Increasing at the overall diameter of the artery ( Fig. 7 ),
- Crescent-shaped mural thickening ( Fig. 7 ),
- Intimal flap (less common in VA than ICA) ( Fig. 8 ,
Fig. 10 ),
- Dissecting aneurysm,
- Irregular or regular stenosis at the lumen ( Fig. 5 ,
Fig. 6 ),
- Occlusion of the vessel,
- Thin peripheral enhancement of vessel wall.
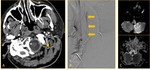
-MRI: There are many useful sequences when assessing dissections.
DWI and FLAIR images are key sequences to look for the proof of cerebral infarction as a consequence of dissection ( Fig. 6 ,
Fig. 8 ,
and Fig. 14 ).
The fat-saturated T1 weighted (fat-sat T1W) MRI is the best sequence to show the subintimal hematoma at the vessel wall.
Also,
T2 weighted (T2W) MRI may be useful to demonstrate intramural hematoma.
The signal of the intramural hematoma varies depending on the stage of hemorrhage.
In the acute and chronic phase,
the intramural hematoma is mostly isointense and can hardly detect on fat-sat T1W images.
However,
in the subacute phase,
the intramural hematoma is typically hyperintense and can be clearly seen on fat-sat T1W sequences.
Besides,
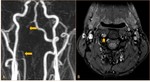
there are some new MRI techniques in the imaging of CAD such as 3D turbo-spin echo sequences called Sampling Perfection with Application optimized Contrasts using different flip angle Evolution (SPACE) ( Fig. 12 ).
3D T1 SPACE sequence is in the use of the diagnosis of CAD with some advantages.
This sequence allows multiplanar reconstructions which are very practical in tortuous regions ( Fig. 13 ,
Fig. 14 ).
Also,
recent studies showed that compared with fat-sat T1W,
3D T1 SPACE sequence has a shorter acquisition time and a larger coverage area that allows showing all arterial portions (cervical and intracranial) in only one acquisition.
The findings of ICA and VA dissections on MRI;
-MRA: Time-of-flight (TOF) MRA or contrast-enhanced (CE) MRA are typically used to utilize the ICA and VA. CE MRA contributes the diagnosis of the dissection by providing information about the vessel lumen though TOF MRA can also demonstrate subacute intramural hematoma.
The findings of ICA and VA dissections on MRA;
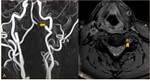
- Irregular stenosis (string sign or rat tail’s sign) ( Fig. 4 ,
Fig. 12 ),
- Focal narrowing with a distal site dilatation (string and pearl sign) ( Fig. 12 ,
Fig. 17 )
- Occlusion of the artery ( Fig. 11 ,
Fig. 15 )
- Tapered occlusion (flame shaped occlusion) ( Fig. 19 )
- Pseudoaneurysm formation ( Fig. 16 )
- An intimal flap ( Fig. 21 )
- Double lumen sign ( Fig. 21 )
DSA: Although considered as the gold standard method for diagnosis and endovascular treatment,
DSA is an invasive modality and cannot display the wall of the artery.
The findings of ICA and VA dissections on DSA;
- Irregular stenosis (string sign or rat tail’s sign) ( Fig. 8 ,
Fig. 18 ),
- Focal narrowing and distal dilatation (string and pearl sign)
- Tapered occlusion (flame shaped occlusion) ( Fig. 19 )
- Pseudoaneurysm formation ( Fig. 20 )
- An intimal flap ( Fig. 20 )
- Double lumen sign ( Fig. 20 )
PITFALS:
Periarterial fat or veins,
turbulent or slow flow in the artery,
hypoplastic artery surrounded by fat may cause false positive results in the MRI-MRA by mimicking intramural hematoma.
Causes of false negative on MRI-MRA are lack of hyperintense signal on T1W images and thinking narrowed vertebral artery such as a normal asymmetric vertebral artery.
Causes of false-positive findings on CTA are atherosclerotic arterial wall thickening,
ulcerated atheromatous plaques,
pulsation artifacts,
dental amalgam artifacts,
motion artifacts,
and slow flow in the artery.