AGE RANGE
The age variable was categorized as qualitative and 5 groups were obtained according to the age range: (≤15,
16-35,
36-55.56-75,
≥76.) The largest number of patients belonged to the age range (56-75) and none was younger than 15 years.
Figure 1.
Distribution by age range of the patients included in the study.
SEX DISTRIBUTION
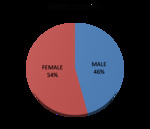
38 of the patients studied were men (46%) and 45 were women (54%)
Figure 2. Percentage representation of the distribution of salivary gland nodules according to sex.
When the statistical analysis was performed,
no significant relationship was found between age and sex with the ultrasound pattern of the studied nodule or with the definitive diagnosis.
PREVIOUS ONCOLOGICAL DISEASE AND PREVIOUS PET-TC
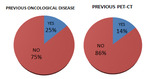
Up to 21 of the total of 83 patients (25%) studied presenting a cancer history,
the most frequent being lung adenocarcinoma. 14% of the patients studied (12),
all of them with a study performed by oncological antecedent,
had a previous PET-CT that showed the presence of some nodule in the parotid or submandibular gland.
Figure 3.
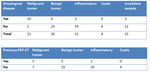
Figure 4. Table of contingency between oncological history and definitive diagnosis and table of contingency between previous PET-TC and definitive diagnosis.
Once the statistical analysis was carried out,
it was obtained that the oncological antecedent significantly increased the probability that the nodule studied was due to secondary involvement (P <0.05).
In our study,
the presence of an intraglandular hypercaptant nodule in the PET-CT study was related to a tumor nature,
predominantly malignant.
The results were not significant P = 0.08
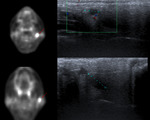
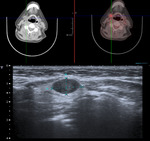
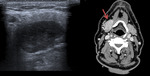
55-year-old woman with history of lung adenocarcinoma who is cited for obtaining cytological material guided by ultrasound of two parotid nodules visualized in a PET-CT study.
Figure 5. Axial cuts PET / CT fusion: two nodular hypercaptant images are observed in the left parotid (red arrows).
Ultrasound was visualized as two homogeneous hypoechoic solid nodules.
Citology: metastases of lung adenocarcinoma.
We also observed cases with hypercapitating nodular lesions in a follow-up PET-CT study in patients with a cancer history that resulted in benign glandular neoplasms.
Patient 69-year-old woman with stage IV breast cancer.
Figure 6. Full body 18F-FDG PET-CT study.
Axial images of CT and PET-CT fusion in which a hypercapitating nodule is seen in the right submaxillary gland.
Ultrasonography identifies a homogenous hypoechoic solid lesion.
Cytology: Pleomorphic adenoma.
SALIVARY GLAND AND ECOGRAPHIC PATTERN:
23 nodules (28%) studied were in the submandibular glands and 60 in the parotid glands (72%). There was no significant relationship between the type of gland where the nodular lesion was located and the rest of the variables studied.
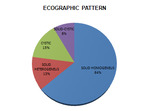
Figure 7. Percentage representation of the type of ultrasound pattern of the nodular lesion.
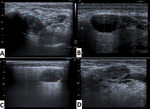
Four echographic patterns were described.
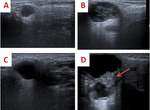
Figure 8. A) HOMOGENEOUS SOLID.
A 67-year-old male with a nodule of solid appearance and echogenicity decreased in the superficial lobe of the right parotid.
Citology: metastases of lung adenocarcinoma.
B) HETEROGENEOUS SOLID.
A 58-year-old woman with a nodule located in the right parotid with a solid appearance and heterogeneous echogenicity,
observing hyperechoic central areas and peripheral areas of lower echogenicity.
Citology: Warthin's tumor.
C) CYSTIC. A 37-year-old male with a palpable lesion.
Anechogenic nodule located in left parotid and with presence of posterior reinforcement in relation to lesion of probable cystic nature.
Citology: No material was obtained.
D) SOLID-CYSTIC (Mixed). An 82-year-old male with a rapidly growing mass in the right parotid region.
Mixed echogenicity lesion with cystic surface area and solid component in its deepest slope (red arrow).
Citology : Mucoepidermoid carcinoma.
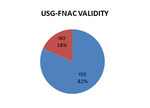
USG-FNAC VALIDITY
In 82% of cases,
material was obtained for cytological study.
Only in 15 patients (18%) the sample was not valid (Figure 9),
in 9 patients by insufficient sample and in 6 cases by obtaining hemorrhagic smear.
In practically all of the nodules with a solid aspect,
material was obtained.
Cystic and mixed nodules are those that showed the lowest diagnostic yield in the USG-FNAC study; however these results were not significant (p> 0.05).
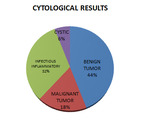
CYTOLOGICAL DIAGNOSIS:
Four large groups of glandular pathology were defined: Benign tumor (44%),
being the pleomorphic adenoma and the Warthin tumor the only representatives of our study; Malignant tumor (18%),
with predominance of metastases; Inflammatory / infectious pathology (32%), that included abscesses,
reactive pattern,
chronic inflammatory pathology and Cystic pathology (6%) (Figure 9) and (Figure 10).
86% of nodules of a tumoral nature were presented as ultrasound homogenous solid,
predominantly hypoechogenic p <0.05.
The inflammatory affectation presented greater heterogeneity of ultrasound presentation,
although up to 45% appeared in the form of a homogeneous solid nodule.
(Figure 11).
Figure 12. Axial contrast-enhanced CT-scan in venous phase: Increase in volume of the right submaxillary gland with respect to the contralateral gland that presents a homogeneous enhancement after contrast administration (red arrow).
The ultrasound show like an homogenous solid nodule.
Cytology: suggestive of acinic cell carcinoma that was confirmed with surgical piece study.
Figure 13. Different lesions of an inflammatory / infectious nature.
A) Solid hypoechoic lesion with study suggestive of abscess.
B and C ) Solid homogeneous intraparotid lesion compatible with reactive adenopathy.
D) Submaxillary lesion of pseudonodular morphology with heterogeneous echogenicity compatible with chronic inflammatory affectation.