EPIDEMIOLOGY
JNA is a vascular non-capsulated neoplasm, histologically benign but locally aggressive.
It represents 0,05% of all head and neck tumors and is the most common benign nasopharyngeal neoplasm,
tipically occurring in young males between 9 and 19 years of age [1].
ANATOMY
The exact site of origin of the lesion is controversial,
because this mass usually presents when it has reached considerable size. JNA is thought to originate in the pterygopalatine fossa in the area of the sphenopalatine foramen; some authors consider the site of origine at the level of vidian canal aperture [2].
The pattern of growth is highly predictable: asymmetric (one side is always the primary site of involvement) with the tendency to follow a submucosal plane and invade the basisphenoid’s bone [3,
4].
The tumor can extend:
- medially into nasopharynx,
nasal fossa and the controlateral side;
- laterally into the infratemporal fossa;
- posteriorly can reach critical structures such as internal carotid artery (ICA),
cavernous sinus and orbital apex passing trough several points of minor resistance (such as vidian canal,
foramen rotondum,
inferior orbital fissure).
Intracranial invasion is a late event (ranges from 4.3% to 11%) [5],
occurring at the level of the middle cranial fossa,
but the tumor usually remains extrameningeal.
Pterygopalatine fossa can be considered as a 3-dimensional box with:
- Anterior wall: posterior wall of maxillary sinus
- Posterior wall: pterygoid plates,
lesser wing of sphenoid bone
- Superior wall: inferior orbital fissure
- Inferior wall: narrowing to palatine canals
- Medial wall: perpendicular plate of palatine bone and sphenopalatine foramen
- Lateral wall: pterygomaxillary fissure
CLINICAL FINDINGS
The typical symptoms are progressive unilateral nasal obstruction (80-90%) with rhinorrhea and recurrent unilateral epistaxis (45-60%); headache (25%) and facial pain may arise secondarily to the obstruction of paranasal sinus,
unilateral secretory otitis media secondarily to impairment of Eustachian tube function.
Other symptoms are proptosis,
facial deformity,
nasal voice,
sinusitis,
nasal discharge and anosmia [1].
HISTOPATHOLOGICAL ASPECTS
Histologically JNA consists in a thick vascular network composed of irregular blood vessels within a connective fibro-cellular tissue,
rich in collagen and fibroblasts.
Vessels are extremely variable in size and shape,
without elastic fibers in their walls and with a frequently incomplete muscolar layer. Due to these histological features,
JNA is prone to bleeding.
The pathogenesis of JNA is unclear,
and many theories regarding its pathogenesis have been proposed.
Given the high prevalence among young males, the role of hormonal influence has been debated.
Moreover,
because of its marked vascularization,
many authors consider JNA as a vasoproliferative malformation that might be due to incomplete regression of the first branchial artery (temporary embryological connection between ventral and dorsal aorta); this theory is supported by the expression of laminin alpha-2 (marker for early embryological angiogenesis) and of collagen-type VI (extracellular matrix component that is attractive for neural crest cells) in JNAs [3].
IMAGING
The diagnosis is based on three main imaging features [4,
6]:
- site of origin: as previosly reminded,
JNA arises close to the sphenopalatine foramen and it usually appears as a mass that expands medially into the nasal cavity,
eroding the root of the pterygoid process.
- hypervascularization after contrast administration
- patterns of growth
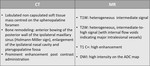
CT and MRI are the two preferred modalities used to determine the extent of the tumor and may be also be used to detect the feeding vessels (Table 1).
Due to the intense tumor vascular supply,
diagnostic biopsy has to be avoided.
JNAs appear as highly enhancing masses after contrast administration with epicenter in the pterygopalatine fossa, involving the nasopharynx and nasal cavity,
sphenoid sinus and infratemporal fossa [2,
7].

Table 1: Key facts in CT and MR imaging features of JNA
CT is useful to demonstrate bony changes in detail: bone is not typically destroyed,
but remodelled or resorbed,
and this feature may be helpful to differentiate JNA from other more aggressive lesions.
On MRI,
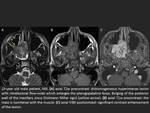
JNA demonstrates low signal-intensity on precontrast T1w images (isointense to muscle) and medium-hyperintense signal on T2w images (Fig. 1).
Intratumor multiple signal voids and significant enhancement after intravenous contrast injection are characteristic MRI features.
Diffusion weighted images (DWI) show no diffusion restriction; the lesion has high intensity on the ADC map,
as expected in benign hypocellular lesion.

Fig. 1: MR features of JNA.
VASCULAR ANATOMY
Maxillary artery (MA),
the major branch of the external carotid artery (ECA) and particularly its terminal branch,
the sphenopalatine artery, are the most commonly involved vessels in JNA vascularization.
MA arises within parotid gland,
behind mandibular neck,
runs anteriorly in the masticator space,
passes through the lateral pterygoid muscle and reaches the apex of the pterygopalatine fossa where it gives off its terminal branches (Fig. 2).

Fig. 2: Typical angiographic appearance of JNA (tumor blush).
Variably,
14 branches arise from the maxillary artery before its terminal branch,
the sphenopalatine artery.
Sphenopalatine artery supplies the medial and lateral walls of the nasal cavity and the sphenoid,
ethmoid,
and maxillary paranasal sinuses.
Its two terminal branches,
the posterior nasal and posterior septal arteries,
contribute to an extensive collateral network involving small vessels,
including ethmoidal collaterals.
In small and lateral JNA,
ipsilateral MA is the only vascular feeder of the tumor,
but as tumor grows,
vascular supply can also come from other arteries,
particularly the ipsilateral ascending pharyngeal artery and branches of the internal carotid artery (mostly inferolateral trunk) (Fig. 3).

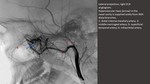
Fig. 3: Juvenile angiofibroma. TSE T2 MR, axial plane(A); intra-arterial DSA (B). DSA demonstrates the several subtle feeders from the
internal carotid artery, not embolized.
ECA and ICA have important anastomoses that have to be kept in mind while doing embolization procedures,
to avoid possible major complications such as embolic stroke or cranial nerve palsies,
and these can be found in three main regions [8]:
1) The orbital region via the ophthalmic artery: there are several potential orbital collateral routes from the ECA to the ophthalmic artery.
In the most frequent case the middle meningeal artery (MMA),
branch of the first segment of MA and remnant of the embyologic stapedial system,
takes over the entire orbital supply (including the central retinal artery and ciliary arteries) from the primitive ophthalmic artery.
This variation is to suspect in case of nonvisualization of the ophthalmic artery from the ICA and presence of a choroidal blush on the ECA injection.
2) The petrous-cavernous region via the inferolateral trunk of ICA (branch of the cavernous segment of ICA) whose branches can have anastomoses with both proximal MA collaterals (cavernous and orbital branches of MMA and accessory meningeal artery (AMA)) and distal MA collaterals (mainly vidian artery and artery of the foramen rotondum). Furthermore,
distal branches of the ascending pharyngeal artery may have connections with inferolateral trunk.
3) The upper cervical region,
mostly via the ascending pharyngeal artery: as a remnant of the embryologic hypoglossal artery,
the ascending pharyngeal artery may keep connections with the vertebral artery.
TREATMENT
The surgical approaches involve either standard open method (external or intraoral incision),
as well as the recent and more advanced endoscopic approach.
Endoscopic surgery has been demonstrated to be a feasible alternative to external techniques for the management of small-intermediate JNA since the 1990s.
Nicolai et al in 2003 [9] reported that endoscopy was a viable technique for JNAs confined in nasopharynx,
nasal cavities,
sphenoid and maxillary sinuses,
pterygomaxillary fossa and ethmoid.
More recently other studies demonstrated that this approach can be performed even in JNAs extending to the infratemporal fossa,
orbit and parasellar region [3,
10,
11]. Open approaches are still recommended in JNAs encasing the ICA or with a massive feeder contribution from it,
or in the rare cases of intradural spread.
The diffusion of endoscopic management and the high degree of vascularization of JNAs make bleeding control during surgery of paramount importance.
It is widely described in literature that preoperative embolization of JNA greatly reduces intraoperative blood loss [12,
13,
14,
15] and is therefore recommended prior to surgery.
At our institution,
embolization is performed preoperatively in all cases of JNA undergoing surgery.