Methods:
Upon Ethical Committee approval,
the retrospective study was conducted including 24 patients whose chest radiographs showed (SPN) (30 nodules),
including 13 (54%) males,
and 11 (46%) females,
with age ranges from 28 to 79 with the mean age 58.5 years ± 2.31 SD.
No significant age differences in both sexes.
The study took 6 months,
starting from June 2017 to early 2018 in Maadi Military Hospital,
and in a private center in Egypt.
Inclusion criteria were patients of age above 28,
with female patients being non-pregnant,
patients found to have one or more solitary pulmonary nodule on chest x-ray or CT chest.
Exclusion criteria were patients of age less than 28,
or pregnant or diabetic patients or allergic to contrast media,
or patients with renal impairment expressed by high serum creatinine.
Each case,
after written consent had full history; including any medical disorders or drug intake,
type of diabetes,
smoking,
history of cancer,
lesion parameters:diameter,
position,
CT value,
density,
spiculation,
calcification,
cavitation.
Previous CTs was recorded.
Imaging Protocol:
Soon after discovery of one or more lung nodules on Chest X-ray or CT chest,
18-FDG PET/CT procedure was done as follows,
18F-FDG was administered to the patient.
after measuring blood glucose level,
with mean dose about 9 mCi.Fasting for 4-6 hours to improve the absorption and distribution of 18-fluoro-deoxy-glucose (18-FDG).
Oral hydration,
muscle relaxants and assessment of blood glucose control with intravenous insulin to its standardization.
They were instructed to prevent any mental or physical activity before the test.
The patient was positioned in the PET scanner,
approximately about 60 minutes after injection of the radiopharmaceutical agent.
A low dose non contrast CT for attenuation correction and anatomic localization followed by PET images acquisition from the skull base to the mid thigh were obtained.
A diagnostic 128 MDCT post contrast examination was taken after I.V non-ionic contrast administration of the same regions.
Images of CT and corresponding functional PET images are taken in axial,
coronal and sagittal planes.
Patient data was anonymized and results of previous CT examinations,
PET/CT studies and further histopathological results for cases with suspicious or intermediate probability of malignant SPN,
were compared and tabulated.
Reporting for PET/CT was done by 2 consultant radiologists and a nuclear medicine consultant.
The Machines used for CT and PET/CT was Philips Ingenuity TF (Philips Medical Corporation,Eindhoven,Netherlands)and GE Discovery IQ (GE Medical,
Milwaukee,
USA).
Each SPN was evaluated using: semiquantitative values of SUV,
max.SUV and visual (Qualitative) interpretation of the uptake.
Values of max.SUV >2.5 were considered positive (high probability of malignancy).
Values of max.SUV <2.5 were considered negative.
Nodules with max.SUV <2.5,
yet showing increased visual metabolic activity were considered intermediate nodules.
Lesions that showed benign values were advised to follow up using HRCT assessing doubling time and clinical follow up.
A p-value of less than (0.05) was considered significant.
Limitations: high cost,
limited availability of PET/CT scanners,small sample size available,
with different routes of obtaining the pathologies.
Results:
The definitive malignant diagnosis of the 24 cases retrospectively reviewed was 15 (62%),
with malignant lesions seen were: poorly differentiated adenocarcinoma,
undifferentiated Large cell carcinoma,
adenocarcinomas,
neuroendocrine carcinoid tumor,
Small cell lung carcinoma,
in addition to incidental metastatic malignancy of known and unknown primaries.
6 (25%) cases were found definitive bening,
while 3 (12%) were considered indeterminate (equivocal ),
which showed max.SUV <2.5,
yet with increased visual metabolic activity than the physiologic background uptake,
meaning that PET/CT didn’t show definitive result whether it’s benign or malignant,
yet they were as low probability of malignancy (considered suspicious).
The mean SUVmax value was statistically significantly higher in patients with proven malignancies compared to patients with benign SPN.(P <0.001)
The difference between the benign and malignant cases relative to lesion diameter was highly significant.
A positive correlation between lesion diameter and SUVmax value uptake in malignant nodules which was statistically significant.
These results were the confirmed results of the final diagnosis of histopathological investigation which were obtained either by CT guided biopsy,
fine needle biopsy,
Endoscopic Ultrasound guided,
or open surgery.
Table(1) shows comparison between results of CT,
PET/CT,
and histopathological examination in each patient.
Table(2) shows the max.SUV values of each nodule.
of the 24 patients.
With exclusion of the intermediate nodules, diagnostic accuracy in patients with positive or negative results in PET-CT,
had a sensitivity,
specificity,
PPV and NPV of 100% agreement between histopathology and PET-CT.
(table 3)
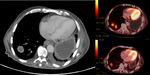
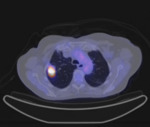
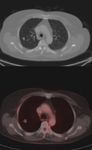
Figures(1-9) show cases clinical presentation.
Discussion:
PET-CT proves a very high sensitivity (89-100%),
but with a lesser specificity (69-100%) and an accuracy of 89-96%,
according to (Jeong et al.)[7]
Though,
What has been proven that not all metabolically active nodules are malignant and indeed an arbitrary cut off value of 2.5 cannot be regarded as wholly accurate.[6]
Benign lesions can occasionally have quite intense uptake and some malignant lesions may be quite quiescent.
Also,
some carcinoid and neuroendocrine lesions have been reported as being causes of false negative studies.
In addition,
scar adenocarcinomas and bronchoalveolar carcinomas can be difficult to detect [6].
In our experience however these lesions often do show low grade but abnormal uptake.
The (SUV) of (SPN) inversely correlates with the lesion’s doubling time.
Lesions with SUV <10,
median survival is approximately 24 months.
Lesions with (SUV) >10,
median survival is only about 11 months.[8]
PET/CT has the advantage that whole body images are obtainable and therefore an assessment can be made of potential distant metastatic disease.[6]
PET/CT is considered the gold standard in the evaluation of single pulmonary nodules that are not amenable to percutaneous biopsy and the assessment of lymphadenopathy[9]
In our study,
A positive correlation between lesion diameter and SUVmax value (i.e.
FDG uptake) in malignant nodules was found .
This correlation was statistically significant,
agreeing with (Dalli A.
et al.)[10]
FDG uptake is observed to be higher in fast-growing and metabolically active lesions with large diameter.
There was a positive correlation between the nodule diameter and risk of malignancy,
agreeing with (Dalli A et al.)[10]
Lesions with high FDG uptake are generally of malignant nature.
However,
false positivity should always be considered.
In patients with another known organ malignancy along with a SPN,
small nodular lesions with low or absent FDG uptake showed a high risk of being malignant as well.
Various strategies may be used to evaluate indeterminate solitary pulmonary nodules.
Growth rate assessment is an important and cost-effective step in the evaluation of these nodules.
Clinical features (eg,
patient age,
history of prior malignancy,
presenting symptoms,
smoking history) can be useful in suggesting the diagnosis and aiding in management planning.[11]
PET/CT is more accurate than CT alone for characterizing pulmonary nodules,
resulting in fewer equivocal findings,
and higher specificity.
Low to intermediate risk nodules ≥ 8 mm should be evaluated by PET/CT,
when the pre-test probability of malignancy is not deemed negligible,
whereas high-risk nodules should be biopsied or excised.[12]
For subsolid nodules, initial follow-up CT is performed at 3 months to determine persistence,
because lesions with an infectious or inflammatory cause can resolve in the interval.
CT enhancement studies are not applicable for subsolid nodules,
and PET is of limited utility because of the low metabolic activity of these lesions.[13]
Lesions like bronchioloalveolar carcinoma,
carcinoid tumor and tiny lesions are causes of limiting PET/CT sensitivity due to low metabolic activity resulting in false negatives.
Lesions with false positive uptake like processes such as tuberculosis,
fungal infections,
and sarcoidosis infectious and inflammatory lesions are also a limitation.[14]
FDG-PET could be a potentially useful tool in determining prognosis and guiding therapy for patients with early-stage NSCLC.[15]
A meta-analysis by (Ruilong Z.
at al.) [16] included 12 studies, total 1297 patients and 1301 pulmonary nodules showed pooled sensitivity,
specificity,
positive likelihood ratio,
and negative likelihood ratio with corresponding 95% confidence intervals (CIs) were 0.82 (95% CI,
0.76-0.87),
0.81 (95% CI,
0.66-0.90),
4.3 (95% CI,
2.3-7.9),
and 0.22 (95% CI,
0.16-0.30).
Radiotherapy planning and response
To quantify the metabolic response of therapy within the tumor ,
as FDG uptake relates well to tumor growth and proliferation rates.
A decline of SUV of more than 20% following therapy correlated well with the overall response to therapy.
Imaging six weeks after chemotherapy has finished and at least three months after radiotherapy is generally regarded as more accurate.
This helps to avoid the problems with false positive reports due to radiation induced pneumonitis.
PET/CT is excellent at delineating tumor from atelectasis.[6]
PET/CT offers advantages in radiation therapy,
including reduced risk of geographic misses; a minimized dose of ionizing radiation to non-target organs,
definition of radiation treatment field of tumor in atelectasis.[13]
The American College Of Chest Physicians Lung Cancer Guidelines recommends that pulmonary nodules should be evaluated by estimating probability of malignancy either by clinical judgment or using a validated model as the Mayo Clinic model,
VA model,
and mathematical model described by (L.
Wang et al.)[2]
(Hou S.
et al.)[17]showed a correlation of histopathological type of lung cancer in SPN and the values of max.SUV’s,
stating that the SUVmax of squamous cell carcinoma was higher than that of the adenocarcinoma,
and that of bronchioloalveolar carcinoma ,
the difference were both statistically significant(P<.001). There were both no significant difference between adenocarcinoma and bronchioloalveolar carcinoma (P = .722),
tuberculosis and inflammatory nodules (P = .858).
Higher the value of SUVmax,
greater the risk of malignancy.
However,
when the SUVmax ranges between 2.5 and 8.0,
the lesion may be benign or malignant.
Our study showed similar results,
yet due to small number of patients,
the correlation of max.SUV with pathological type of the SPN can’t be reliably concluded,
so we recommend doing on far larger number of patients.
PET/CT in precision medicine
(PET/CT) contributes by interrogating tumor heterogeneity throughout the body.
As such,
it is extremely helpful,
not only to distinguish resectable from unresectable disease,
but also to suggest the most appropriate therapy at a metabolic-molecular level.PET/CT is thus a biomarker of prognosis in lung cancer.
[18]
Overall,
PET/CT offers improved diagnosis and staging of lung cancers,
more accurate identification and localization of disseminated malignancy and recurrent disease and planning and monitoring of surgical and adjuvant therapy .[19]