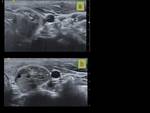
Thyroid nodules are a frequent clinical problem due to the increased use of ultrasonography (US).
Despite most of them are benign and do not require treatment,
some benign nodules may require treatment because of clinic or cosmetic problems [1].
Although surgical treatment is the elective treatment it has disadvantages such as general anesthesia,
postoperative,
scar formation,
increased cost,
risk of temporary/permanent complications,
and iatrogenic hypothyroidism.
Therefore,
during the past two decades nonsurgical minimally invasive treatment methods have been introduced: percutaneous ethanol ablation (EA) and radiofrequency ablation (RA).
In spite of simple aspiration is the treatment of choice,
is usually not successful in thyroid cysts with recurrence rates between 58% and 80%,
depending on the size,
volume and number of previous aspirations [2].
EA consists of an intranodular injection of ethanol that causes a reduction in the volume of cystic thyroid nodules by causing cellular dehydration,
protein denaturation,
coagulation necrosis,
small vessel thrombosis,
leading to reactive fibrosis [2].
This technique is used only for benign thyroid nodules,
cystic (cystic portion >90%) or mixed cystic-solid with a large fluid component (cystic portion of 50-90%) [2,3,4].
Indications (1 A criteria + 1 B criteria)
Criteria A:
- Symptoms: pain,
dysphagia,
dysphasia,
foreign body sensation,
cough.
- Esthetical problems
- Thyrotoxicosis in functioning thyroid nodules.
Criteria B: Surgical treatment is not considered due to
- High surgical risk
- Because postoperative hypothyroidism generates complications that are difficult to manage
- Patient refuses surgical treatment.
Complications [5]
EA is a relatively safe and well-tolerated technique with common side effects such as local pain that may radiate to the jaw or retroauricular area,
transient dysphonia,
flushing,
dizziness,
fever lasting a day,
and hematoma.
In the related literature,
severe but rare complications have been described,
such as jugular vein thrombosis and severe ethanol toxic necrosis of the larynx combined with necrotic dermatitis.
Moreover,
cases of Graves’ disease.
Preablation Assessment Ultrasound:
- It´s necessary two separate ultrasound-guided fine-needle aspiration cytology or biopsies that confirm the benign nature of the nodule [3,4].
- Three orthogonal diameters (ie,
the largest diameter and two other perpendicular diameters) of each nodule were measured,
and the volume of each nodule was calculated by using the equation V = π abc/6,
where V is the volume,
a is the largest diameter,
and b and c are the other two diameters [3,4].
- US to evaluate the surrounding anatomy: vascular structures (ACI,
VYI),
recurrent laryngeal nerve,
trachea and esophagus. Take especially care to the vascular structures along the approach route to prevent serious hemorrhage [2,3,4].
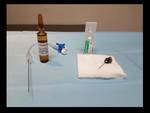
Equipment and materials (Fig.
1)
|
Ultrasound scan with a high-frequency linear transducer
|
|
Local anesthesia (2% Lidocaine)
|
|
95–99% Ethanol
|
|
Spino-scan needles (20-gauge).
|
|
3-Way stopcock with extension tube
|
EA procedure [2,3,4]
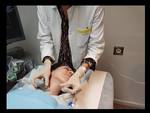
- Patients are in the supine position,
with mild neck extension (Fig.2).
- The puncture site and course are anesthetized with 2% lidocaine.
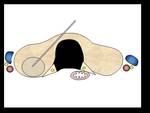
- Target nodules are approached using a transisthmic approach method under a transverse ultrasound view.
This technique prevents a change in the position of the needle and also eliminates leakage of injected ethanol to areas outside the thyroid gland (Fig.3).
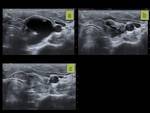
- After place the needle tip into the central portion of the cystic nodule the content is aspirated to the maximal (Fig.4).
- Slow injection of 95–99% ethanol into the cystic space of the nodule (the volume of ethanol injected corresponded to 50% of the volume of aspirated fluid).
This will produce a shaded effect under the needle (Fig.5a).
- After 10 minutes with the needle in place,
the injected ethanol is completely removed.
Then,
we measure the remaining nodule (just composed of a solid portion) for future controls (Fig.5b).
- The patient is observed for 30 minutes by nursing.
If no complications,
discharge.
Bits of Advice:
- Explain the procedure steps to the patient in order to diminish its anxiety.
- Ask the patient to be calm,
not to swallow and keeping superficial breathing.
- The tip of the needle should be continuously visualized to prevent complications.