Type:
Educational Exhibit
Keywords:
Head and neck, Interventional non-vascular, Thyroid / Parathyroids, Ultrasound, Education, Treatment effects, Education and training
Authors:
I. CASES SUSARTE, C. Vázquez Ólmos, S. Torres del Rio, I. M. González Moreno, B. Márquez Argente del Castillo, M. J. GAYÁN BELMONTE, M. Lozano Ros, J. Trejo Falcón, A. García Chiclano; MURCIA/ES
DOI:
10.26044/ecr2019/C-1442
Findings and procedure details
Our experience with percutaneous EA consists of 7 patients with benign (anatomopathological diagnosis) cystic or mixed predominantly cystic thyroid nodules who were admitted to our medical center between March 2016 until the present.
Patients were complaining about either cosmetic or pressure symptoms.
The EA procedure was performed as we have already explained by one of the two neuroradiologists of our service,
with 10 and 15 years of thyroid US experience.
No major or minor complications were observed.
Follow-up and outcome assessment
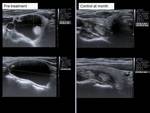
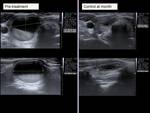
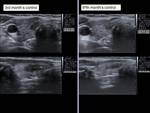
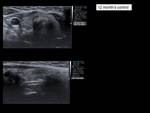
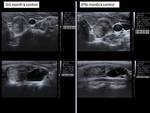
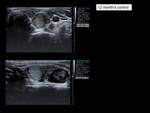
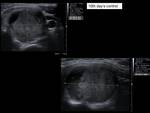
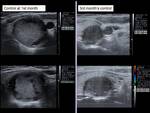
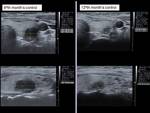
We performed ultrasound controls at a month,
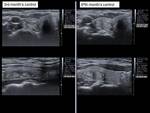
3 months,
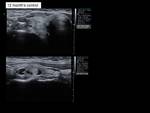
6 months and 12 months,
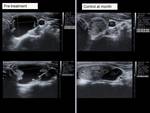
assessing the reduction of the volume of the nodule (Vol = πabc / 6) according to the formula (Initial volume-Last volume) / Initial volume (Fig.6-14).
The reduction percentages are shown in table 1.
The mean volume reduction at 1-year control was 82.9%.
Table 1.
% Of nodules volume reduction
|
Patient
|
Control at month (%)
|
Control at 3 months (%)
|
Control at 6 months (%)
|
Control at 1 year (%)
|
|
1
|
80
|
88
|
90
|
86
|
|
2
|
78
|
85
|
82
|
83
|
|
3
|
88
|
96
|
97
|
98
|
|
4
|
48
|
85
|
96
|
99
|
|
5
|
*
|
31
|
75
|
88
|
|
6
|
25
|
33
|
50
|
60
|
|
7
|
71
|
79
|
76
|
68
|
*That patient didn’t come for the first’s month control
In two patients small intracystic bleeding occurred during the ethanol injection,
however,
the procedure was equally effective (patients 4 and 5).
Also,
in one of them,
the bleeding increased one week after the procedure,
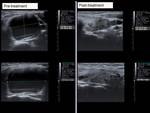
with the nodule reaching the initial size but with a very good evolution (patient 4,
Fig.
14-18).
Only in one patient we observed a slight growth in size at 6 and at 12 months control due to an increase in the cystic component (patient 7).