LEIOMYOMAS OF FEMALE GENITAL TRACT
Leiomyomas constitute the most common benign uterine tumors (20–30% of reproductive age females).
Clinical presentation
Most patients are asymptomatic.
Symptoms are related to the number,
size,
and location of the tumors.
Due to their hormonal sensitivity,
they shrink in menopause and occasionally may grow and bleed in patients receiving progestational therapy or who are pregnant.
Typical appearance
Location within the myometrium of the uterine corpus (FIGO classification).
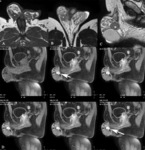
FIGO0-FIGO8 (Fig. 1): submucosal,
intramural,
subserosal and others.
Subserosal and submucosal tumors may be polypoid or pedunculated (Fig. 2)
- Submucosal tumors may undergo torsion or prolapse through the cervical os
- Subserosal tumors may detach from their pedicle and result in a parasitic leiomyoma
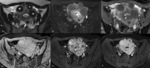
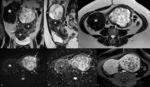
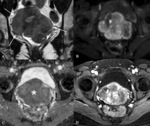
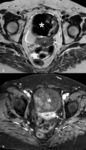
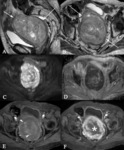
MR imaging (Fig. 3):
- Single or multiple (75%),
round or oval well-circumscribed masses
- T1-weighted images.
Homogeneous and isointense to myometrium
- T2-weighted images.
Homogeneous low signal intensity (Figure 3A)
- Calcification (4%) appears of low signal intensity that does not change on T1 and T2-weighted images
- Edema (50%) may be diffuse and extensive (high signal intensity on T2- weighted images)
- In some cases,
leiomyomas have a hyperintense rim on T2-weighted images related to dilated veins,
lymphatics,
or edema
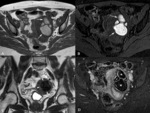
- Diffusion-weighted images (DWI).
Hypointense on both DWI and apparent diffusion coefficients (ADC) maps (blackout phenomenon) (Figures 3B and 3C)
- Contrast-enhancement.
Variable,
usually early homogeneous enhancement,
parallels to myometrium (Figure 3D,
3E and 3F)
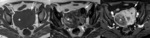
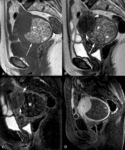
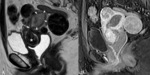
Most leiomyomas (60%) have focal or diffuse hyaline degeneration (deposits of collagen fibers into areas of the leiomyoma with insufficient vascular supply).
- Similar MR imaging features to non-degenerated leiomyomas,
but minimal or no contrast-enhancement (Fig. 4).
Atypical appearance
Degenerated leiomyomas
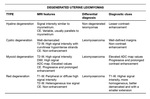
Table 1 summarizes the MRI findings of degenerated leiomyomas and the diagnostic clues to differentiate between them and from leiomyosarcoma and other genital tumors.
Cystic or hydropic degeneration
Focal (50%) or diffuse (4%) edematous changes may be accompanied by myxoid degeneration.
These tumors pose a significant diagnostic dilemma due to rapid growth. Elevation of CA-125 and associated pseudo–Meigs causing more challenge in diagnosis.
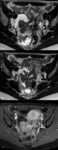
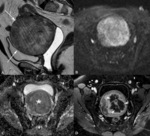
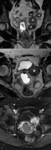
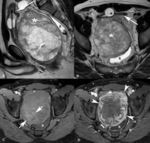
MR imaging ( Fig. 5):
- Large or small round well-demarcated cystic areas
- T2-weighted images.
Hyperintense with curvilinear hypointense strands (split fiber sign) corresponding to fibers split up the fluid accumulation and edema
- Contrast-enhancement.
Non-enhancement or peripheral enhancement
Myxoid degeneration
Cystic foci of gelatinous material,
either abundant or interspersed between
smooth muscle cells.
Myxoid degeneration may also be seen in leiomyosarcomas.
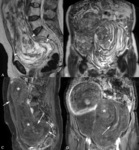
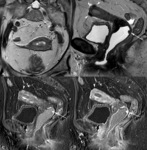
MR imaging ( Fig. 6 and Fig. 7):
- Hyperintense on T2-weighted images
- Diffusion-weighted images (DWI).
Hyperintense on both DWI and ADC maps
- Contrast-enhancement.
Progressive and prolonged contrast-enhancement
Red degeneration
Coagulative necrosis secondary to sudden venous thrombosis within the periphery of the lesion.
Acute red degeneration
Most often during pregnancy and with oral contraceptive use. Usually causes systemic symptoms such as low abdominal pain,
pyrexia,
and leukocytosis.
MR imaging:
- Well-circumscribed mass with peripheral dilated vessels
- Peripheral rim,
hyperintense on T1-weighted images and hypointense on T2-weighted images (attributed to the proteinaceous content of blood and intracellular methemoglobin in the obstructed vessels)
Chronic red degeneration phase
Most patients are asymptomatic.
MR imaging (Fig. 8):
- T1-weighted images.
Diffuse high signal intensity
- T2-weighted images.
Heterogeneous hypointense signal
- Contrast-enhancement.
Non-enhancement
Variant subtypes
Table 2 summarizes the MRI findings of variant subtypes of leiomyomas and the
diagnostic clues to differentiate between them and from leiomyosarcoma and
other genital tumors.
Cellular leiomyoma
Compact smooth muscle cells with little or no extracellular matrix.
MR imaging (Fig. 9):
- T1-weighted images.
Isointense to myometrium
- T2-weighted images.
High signal intensity
- DWI.
Hyperintense with a low ADC value
- Contrast-enhancement.
Early and moderate to intense enhancement (greater than ordinary leiomyoma)
Lipoleiomyoma
An uncommon tumor (postmenopausal women and usually associated with uterine leiomyomas.
Asymptomatic (most patients) or abnormal uterine bleeding,
palpable mass,
urinary frequency,
or abdominal pelvic pain.
MR imaging features are diagnostic (Fig. 10):
- Well-circumscribed mass
- Heterogeneous signal intensity (areas with signal intensity similar to fat,
hypointense septa on T2-weighted sequences and septal contrast-enhancement)
Smooth muscle tumors of uncertain malignant potential (STUMP)
Rare masses with histologic features that are categorized between leiomyomas
and leiomyosarcomas.
- Without atypia or mild atypia with coagulative necrosis with mitotic index <
10/10 <10 high-power fields)
MR imaging features can mimic nondegenerated leiomyomas or leiomyosarcomas.
Imaging findings suggestive but non-specific include (Fig. 11):
- Large,
heterogeneous well-demarcated tumor
- Hypointense T1 signal and moderate T2 signal intensity
- Contrast-enhancement.
Cystic necrotic areas with marked enhancement of solid areas
- DWI.
Solid areas appear hyperintense with low ADC values
Unusual locations and growth patterns
Prolapsed leiomyoma
Prolapsed leiomyoma may be cervical or submucosal (5%) origin and can prolapse (2.5%) through the cervical canal or even into the vagina.
Prolapsed submucosal leiomyomas may undergo torsion and necrosis,
might be infected and cause prolonged vaginal bleeding (impairment of the blood supply through the pedicle).
MR imaging:
- The origin of the mass and its stalk is accurately identified by sagittal MR imaging (Fig. 12)
- Signal intensity similar to non-degenerated leiomyomas or heterogeneous signal when undergo torsion or necrosis
Parasitic leiomyoma
Parasitic leiomyomas are pelvic benign SMT separate from the uterus.
Origin:
- Pedunculated subserosal leiomyomas that lose their original connection to the uterus by torsion and attach to other structure with parasitic vessels
- Usually,
there is a previous history of laparoscopic hysterectomy (39%) or myomectomy (44%) with power morcellation,
may recur after surgical resection or show hormone responsive behavior
Most leiomyomas of the broad ligament are parasitic leiomyomas or subserosal
uterine leiomyomas that extends between the folds of the broad ligament.
These tumors may be associated with pseudo–Meigs syndrome (nonmalignant ascites and/or pleural effusion caused by solid pelvic tumors),
produce an elevated CA-125 level and may mimic a solid ovarian tumor.
MR imaging features (Fig. 13):
- Irregular configuration
- Signal intensity similar to uterine ordinary or degenerated leiomyoma
- Identification of feeding or draining vessels arising from the myometrium is helpful in distinguishing an intraligamental leiomyoma from retroperitoneal tumor
Cervical leiomyoma (0.6%-2% of all leiomyomas)
Symptoms vary from urinary retention,
frequency,
dyspareunia to rare clinical
presentations such as prolapsed cervical fibroid polyp which may mimic
procidentia or even uterine inversion.
MR imaging features (Fig. 5 and Fig. 12):
- Sagittal and coronal planes are usually most useful to identify the cervical origin of the mass
- Signal intensity similar to ordinary or degenerated leiomyomas
Leiomyomas of vagina and vulva
These rare tumors may have estrogen and progesterone receptors and enlarge during pregnancy.
MR imaging features are similar to uterine leiomyomas (Fig. 14):
- T1-weighted images.
Intermediate signal intensity
- T2-weighted images.
Low signal intensity
- MR imaging can accurately differentiate vaginal leiomyoma from prolapsed uterine or cervical leiomyoma or from other vaginal masses
Ovarian leiomyoma (0.5%-1% of benign ovarian tumors)
Ovarian leiomyomas are usually asymptomatic,
may be associated with pseudo–Meigs syndrome and coexist with uterine leiomyomas (80%).
Most common unilateral in middle-aged woman.
In young women usually are bilateral and not coexist with uterine leiomyomas.
MR imaging features.
Similar to uterine leiomyomas:
- T1-weighted images.
Intermediate signal intensity
- T2-weighted images.
Low signal intensity
Main differential diagnosis:
- Ovarian fibroma/fibrothecomas (similar signal intensity on T1 and T2-weighted images)
- Diagnostic clues (Fig. 15).
Uterine leiomyomas show early homogeneous enhancement,
parallels to myometrium,
while ovarian fibroma/fibrothecomas show delayed weak contrast-enhancement
- Subserosal uterine leiomyomas
- Diagnostic clues (Fig. 16).
Continuity of adnexal mass with the adjacent myometrium and bridging vascular sign (feeding vessels that arise from the uterine arteries,
which course through the myometrium and supply large exophytic myomas)
Diffuse uterine leiomyomatosis
It is a rare condition that usually affects younger women (30-40 years-old) and presents similar symptoms to uterine leiomyomas.
MR imaging features (Fig. 17):
- Innumerable,
mostly small,
poorly defined confluent nodules with near complete replacement of the myometrium
- Symmetrical uterine enlargement
Main differential diagnosis:
- Multiple leiomyomas (Fig. 18)
- Diagnostic clues.
Well-circumscribed nodules and asymmetrical uterine enlargement and distortion
LEIOMYOSARCOMAS OF FEMALE GENITAL TRACT
Leiomyosarcomas are aggressive tumors that can develop de novo or,
less
commonly,
as a result of malignant degeneration of a leiomyoma.
They are the
most common uterine sarcoma variant.
Unfortunately,
differentiation between benign degenerating cellular leiomyomas
and leiomyosarcomas is challenging due to considerable overlap
MR imaging features of leiomyomas with atypical features overlap with leiomyosarcomas.
Combination of ≥ 3 of the following MR features suggest leiomyosarcoma (Fig. 19):
- Large,
ill-defined infiltrating myometrial mass with heterogeneous signal intensity
- Heterogeneous hyperintense areas on T1-weighted (hemorrhage) and on T2-weighted images (cystic necrosis).
- DWI.
Hyperintense with restricted diffusion and hypointense on ADC map (overlap with cellular leiomyomas)
- Contrast-enhancement.
Heterogeneous (hemorrhage and necrosis).
Most difficult differential diagnosis:
- Leiomyomas with red degeneration (Fig. 8)
- Diagnostic clues.
T1 signal intensity.
Higher signal intensity,
more homogeneous,
better demarcated and with a smaller extension than leiomyosarcomas
- Cellular leiomyomas (Fig. 9)
- Diagnostic clues.
T2 signal intensity.
Most homogeneous T2-weighted hyperintense masses than leiomyosarcomas
SMOOTH MUSCLE TUMORS OF MALE GENITAL TRACT
Male genital leiomyomas and leiomyosarcomas (penis,
prostate,
seminal
vesicles,
testis,
spermatic cord,
and scrotum) are very uncommon neoplasms
that often escape clinical recognition.
Only isolated case report or small series have been previously reported in the literature.
Epididymal leiomyomas
Leiomyoma is the most common smooth muscle tumors of the male genital tract and the second most common neoplasm of the epididymis (6%) after adenomatoid tumors (30%).
Most common in middle-aged man and appear as solitary nontender hard mass
with indolent clinical behavior.
MR imaging features (Fig. 20):
- Unencapsulated but well-circumscribed
- Intermediate to low T1 signal intensity
- Intermediate to high T2 signal intensity
- Contrast-enhancement.
Early homogeneous enhancement
Leiomyosarcomas
Leiomyosarcoma is rarer and usually found at spermatic cord (10% of
spermatic cord sarcomas) and prostate (25% of prostatic sarcomas).
Patients often present with rapid onset of urinary obstruction and early
pulmonary and hepatic metastases.
MR imaging features (Fig. 21):
- Large,
well-circumscribed masses
- T1-weighted images.
Homogeneous or heterogeneous signal intensity
- T2-weighted images.
Heterogeneous high signal intensity
- DWI.
Varying degrees of restricted diffusion
- Contrast-enhancement.
Heterogenous,
early and avid enhancement
Main differential diagnosis:
- Adenocarcinoma
- Diagnostic clues.
Lesser size and homogeneous appearance
- Embryonal rhabdomyosarcomas
- Diagnostic clues. Large lobulated masses,
often protruding into the bladder lumen in children and adolescents
- Alveolar rhabdomyosarcomas
- Diagnostic clues.
Age of presentation (children and adolescents) and more infiltrative and less well-defined masses