The patients were considered as symptomatic having a left upper quadrant (LUQ) or epigastric pain without other obvious pain cause rather than pancreas.
Clinically abdominal pain was the most common clinical feature in all three groups.
Other symptoms included post-prandial pain,
cramps etc.
LECs were most common in middle-aged males (nine males,
one female),
ranging between 43 to 63 years (mean: 50).
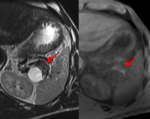
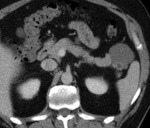
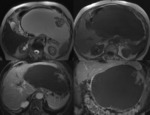
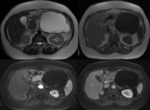
All patients revealed a well-defined exophytic lesion within the tail (70%) or body (30%) of the pancreatic parenchyma,
without communication with the pancreatic duct.
The mean size was 6.1 cm (2.7-22 cm).
MCNs on the contrary presented most exclusively in the middle-aged woman (nine female,
one male) with the age range of 37 to 67 years (mean age 57.7).
The lesions had a solitary / macrocystic appearance in the distal pancreas with a mean size of 5.9 cm.
In all cases pancreatic tail was involved,
with 3 out of 10 occupying both body and tail of the pancreas.
There was no connection to the pancreatic duct as well.
IPMNs were found in both sexes showing a slight male predominance (6 male and 4 female).
The mean patient age was higher than in the both two groups having a mean value of 70.3 years (rage 55 to 78 years).
6 out of 10 affected the head of the pancreas (with one lesion involving the entire pancreas and the other one the pancreatic head and tail),
4 were found in the pancreatic tail.
Mean size was significantly smaller than in the fist two groups with the mean size of 1.9 cm.
The key differential feature was an evidence of communication to the main pancreatic duct,
which was most easy to confirm using MRCP images (when available).
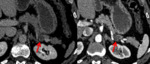
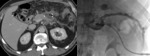
We were able to identify generally three imaging subtypes of LEC.
20% of the LECs where simple cystic lesions (Fig.
1).
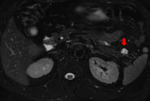
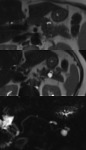
80% of LEC where solid-cystic lesions with different morphology: 30% of them had diffuse solid component (Fig.
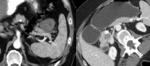
2 and 3) and 50% with one mural nodule (Fig.
4,
5 and 6).
Four LECs where unilocular,
six multilocular and seven had septa.
All of them showed a non-enhancing cystic component (mean UH: 23),
hypo/isointense in T1w and hyperintense on T2w.
Both the septa and the solid components showed contrast enhancement in the multiphase studies.
None of the lesions caused pancreatic/bile duct dilatation or pancreatic atrophy.
We found this feature beneficial in differentiating the LEC to IPMNs,
with IPMNs showing a slight dilatation of MPD in 50% of cases with the mean diameter of 4 mm (cutoff of 3mm,
ranged 3 to 7).
After surgery,
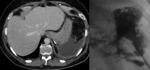
up to 60% of the patients had complications: four had fluid collections that had to be drained,
one had a pancreatic fistula and one developed a pseudocyst.
All complications were treated with radiological interventions without need of the additional surgical procedure (Fig.
7,
8,
9 and 10).
In three occasions,
radiological features where indistinguishable from other cystic neoplasms:
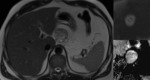
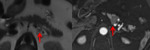
1) The first example of the differential diagnosis difficulties shows a case of 43-year-old male with a small cystic lesion in the pancreatic tail,
which had a similar appearance to an IPMN (Fig.
11 and 12).
Even thought there was no clear connection with the pancreatic duct on the MRCP images,
the diagnosis was not certain and the lesion was resected.
2) 20% of SCNs have a subsolid imaging character.
In such cases small cystic components are not distinguishable on CT images showing a sponge like appearance.
Similar features were found in some LECs in our group,
which is demonstrated in the following example.
In such cases a precise attention should be put on the clinical data of the patient such as sex and age,
as the most SCN are found in the older women.
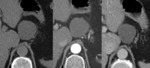
A 46-year-old male had a cystic lesion in the pancreatic tail,
without contrast enhancement.
Even though this patient was a male,
it was difficult to differentiate from a serous cystic neoplasm (Fig.
13),
so the diagnosis was done after histopathological evaluation.
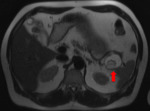
3) Finally,
the only female in our study group was 47 years old and had the similarappearance like a mucinous cystic neoplasm (Fig.
14 and 15),
therefore,
surgery had to be done.